Photo Essay: Ensuring Adequate Reduction with the Reverse Preparation Technique
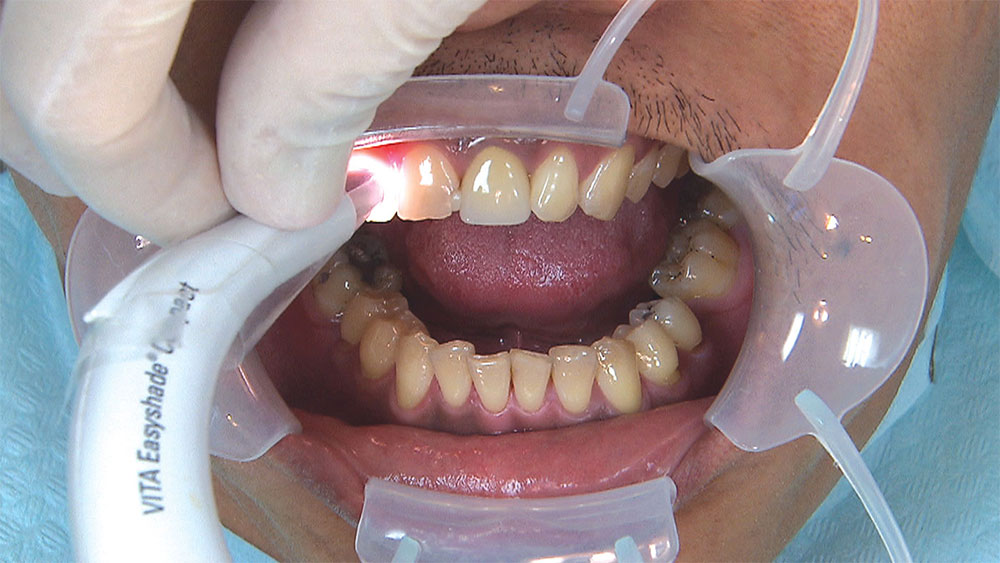
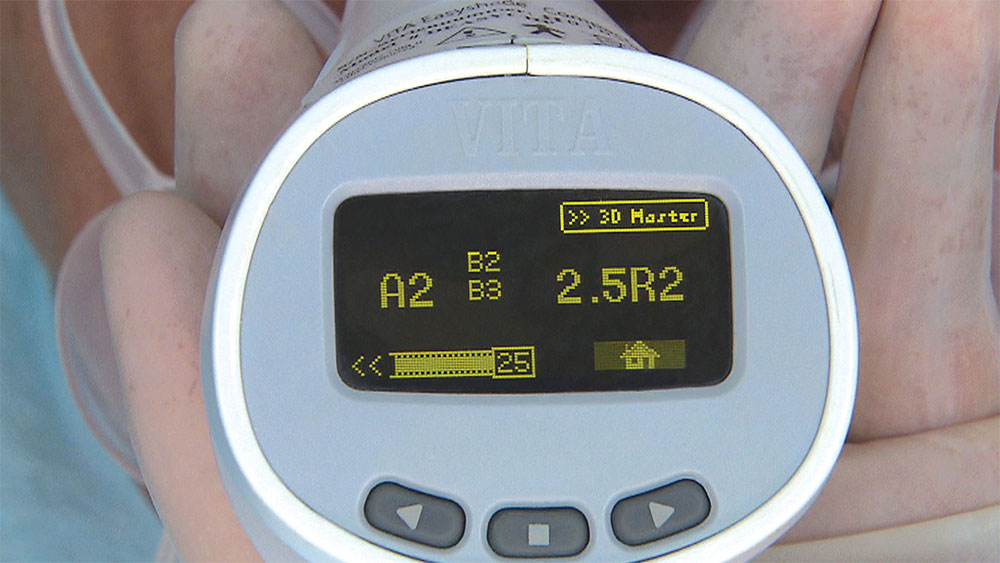
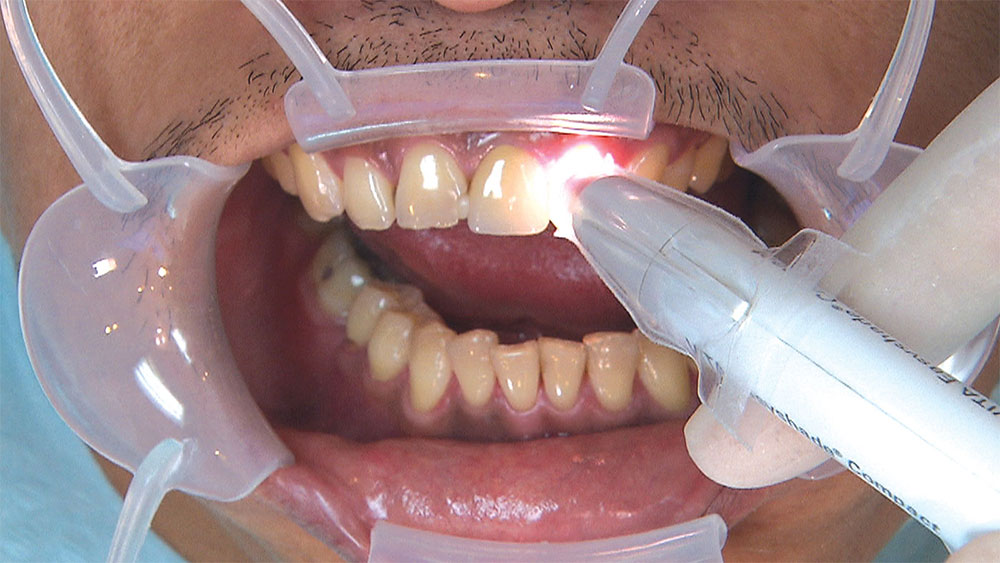
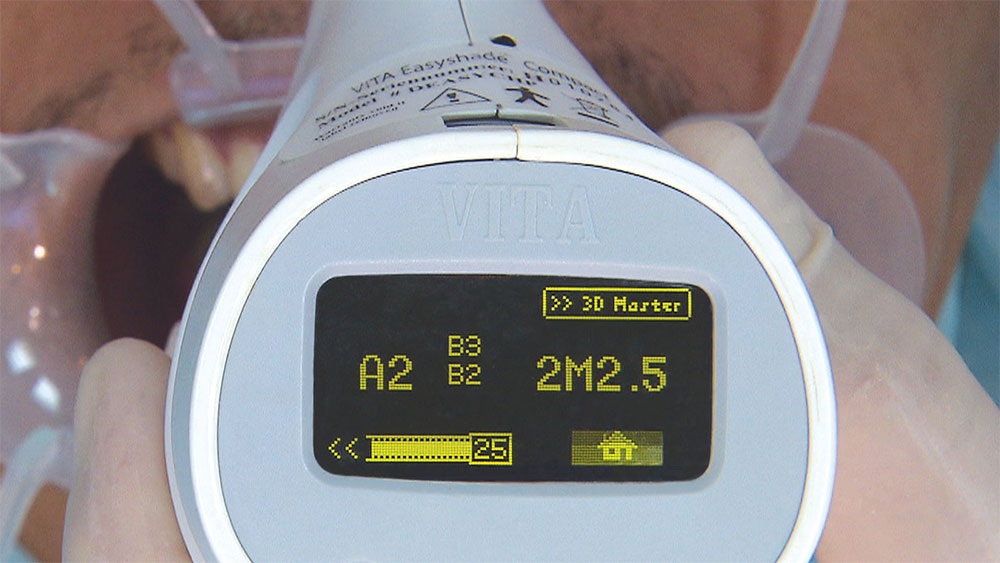
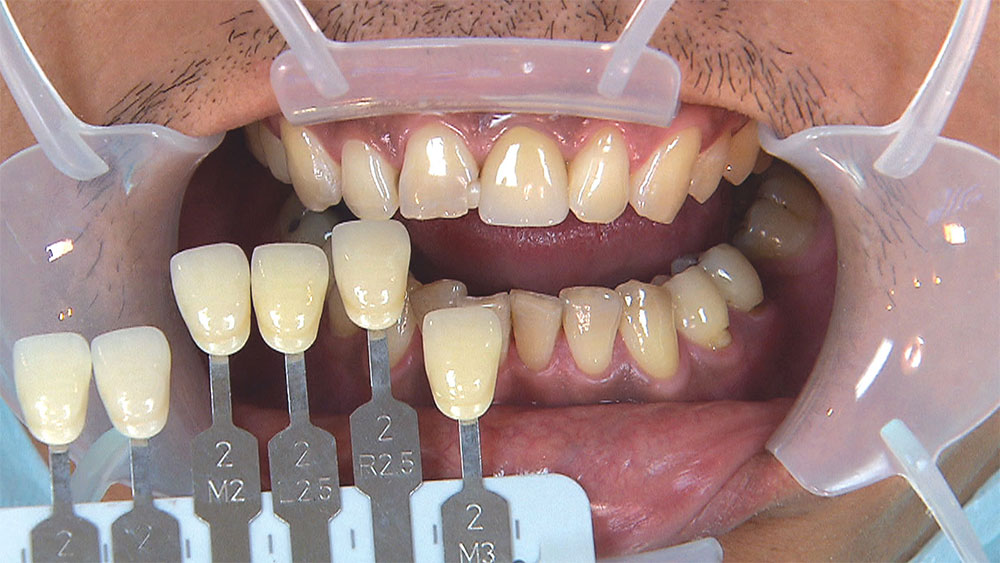
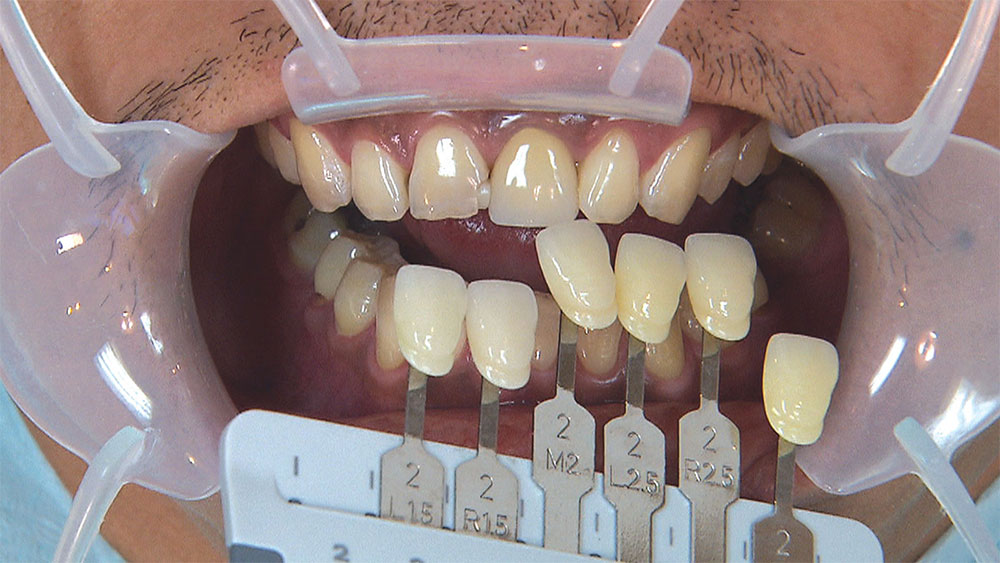
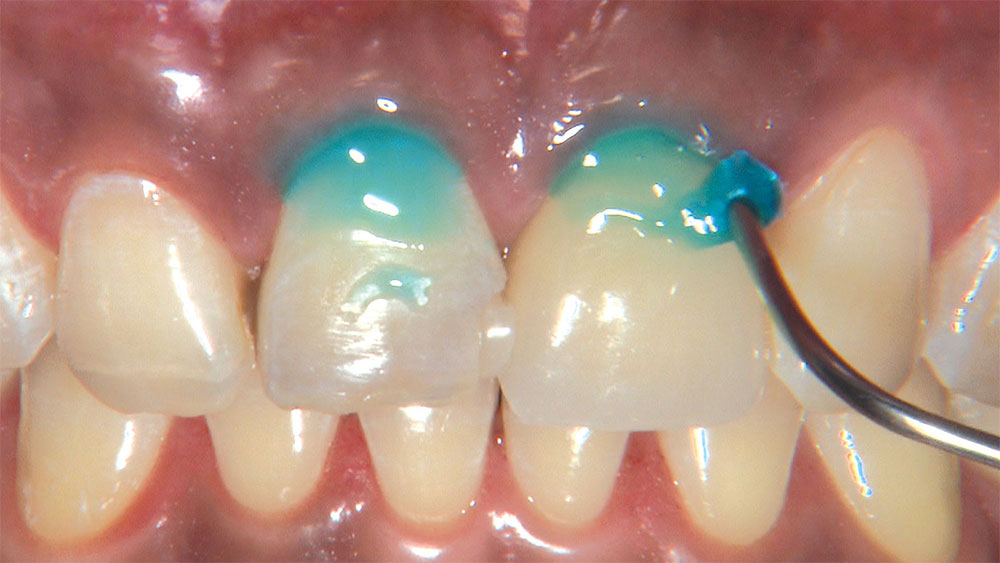
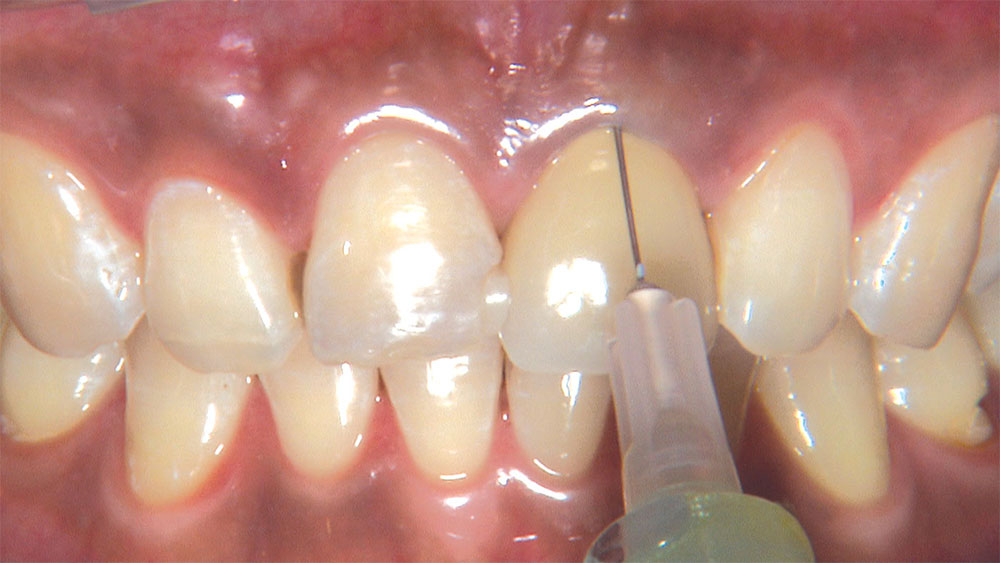
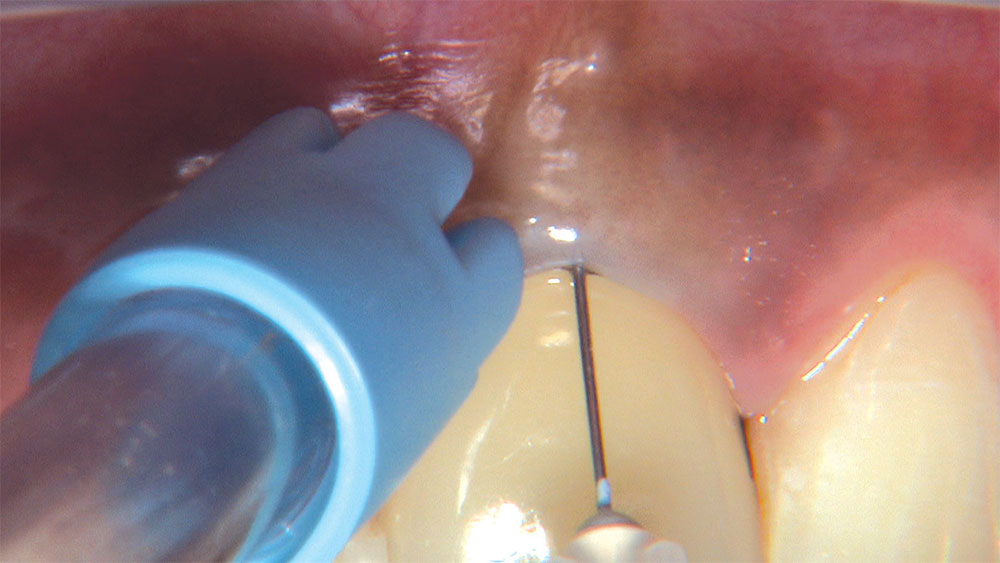
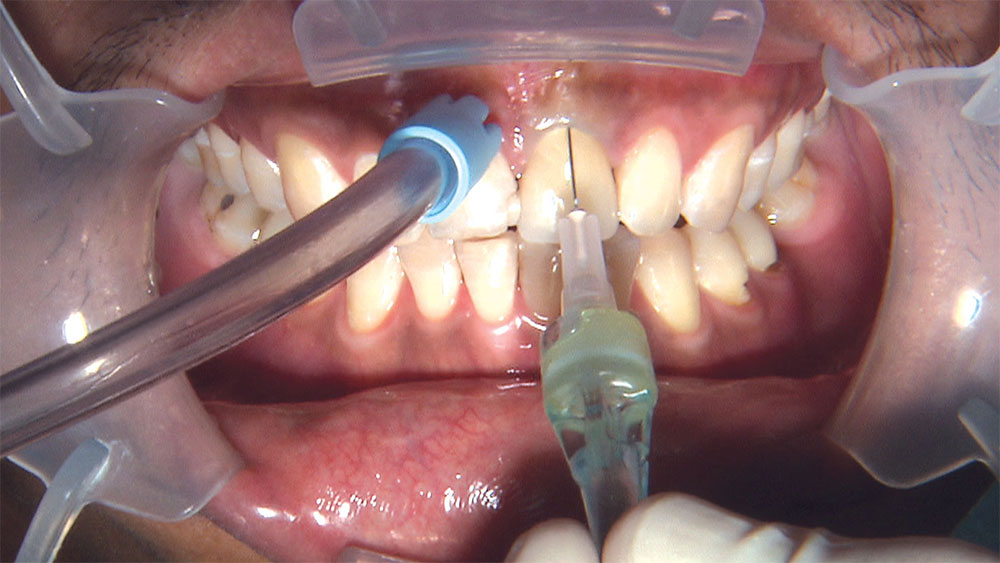
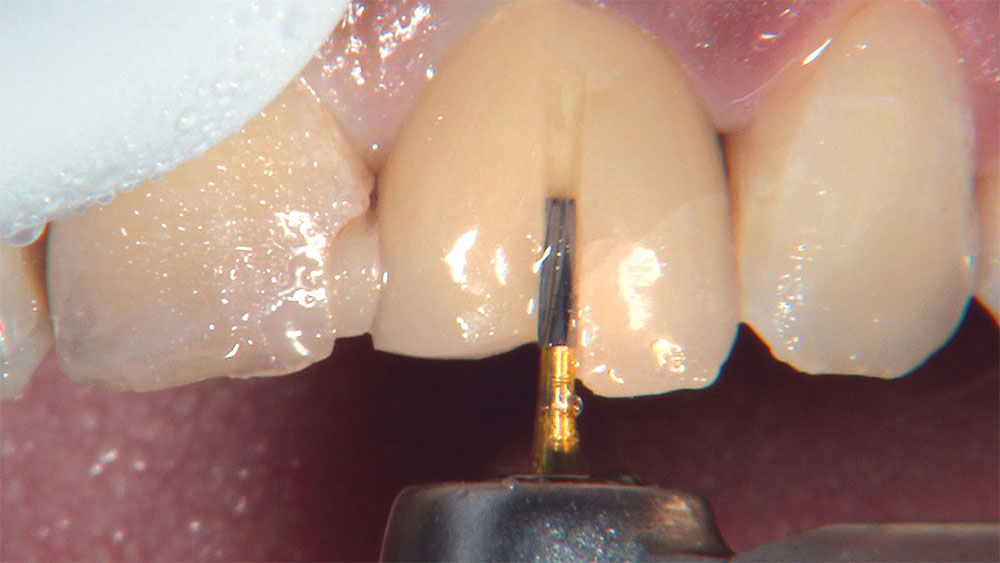
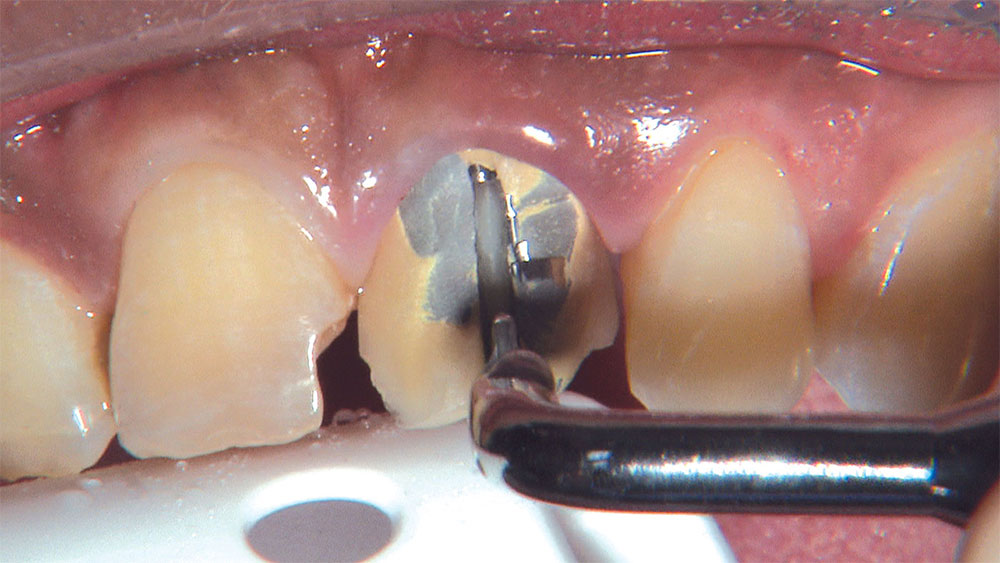
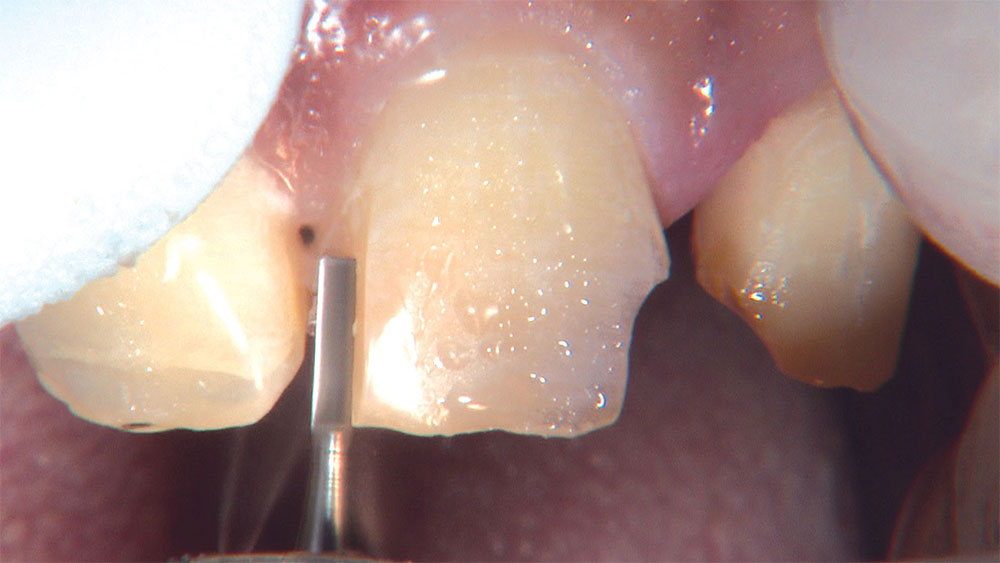
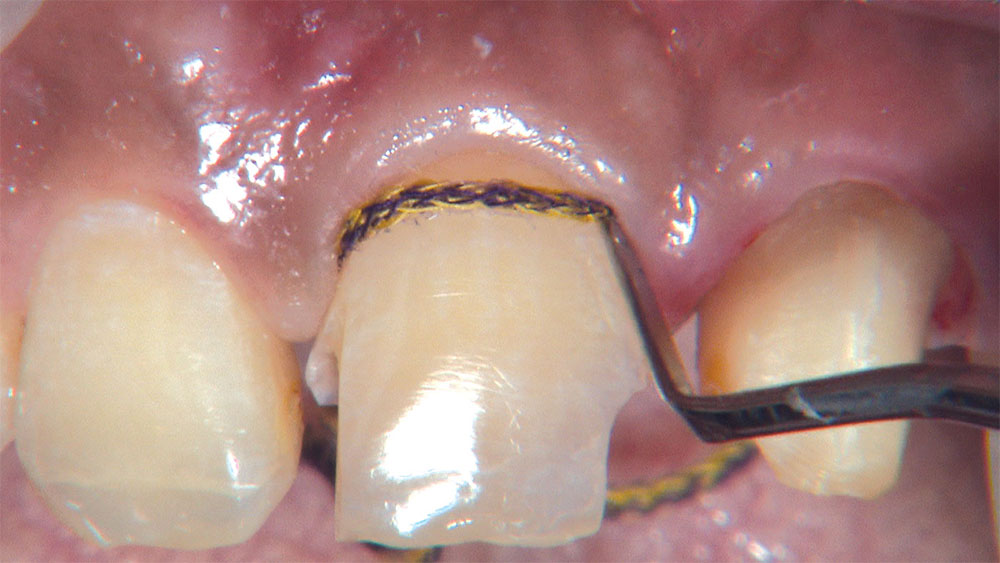
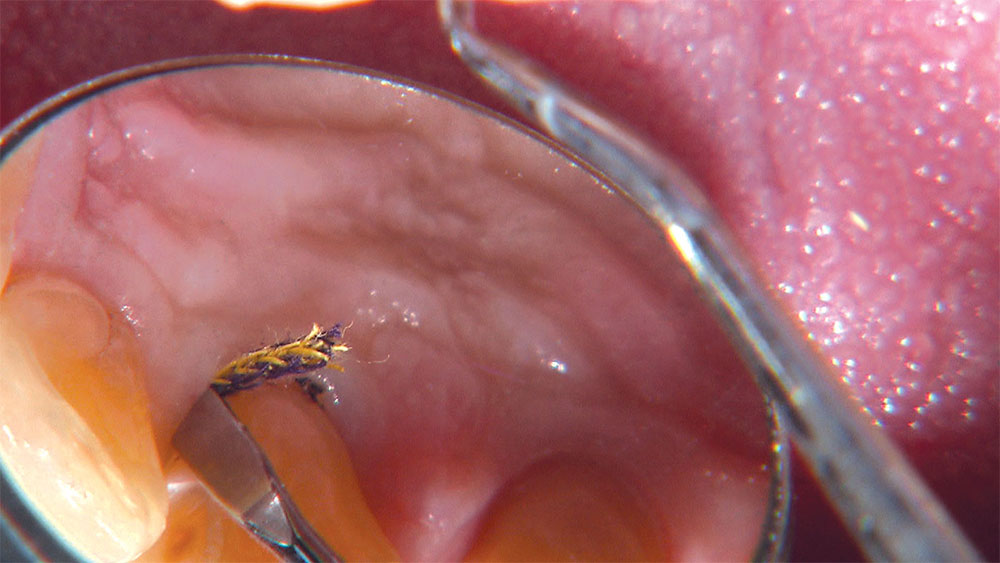
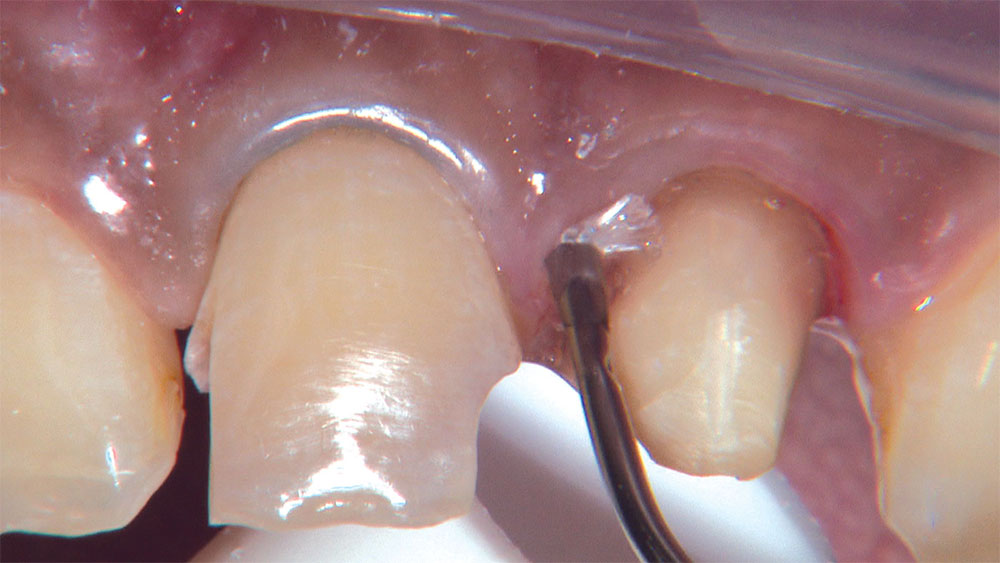
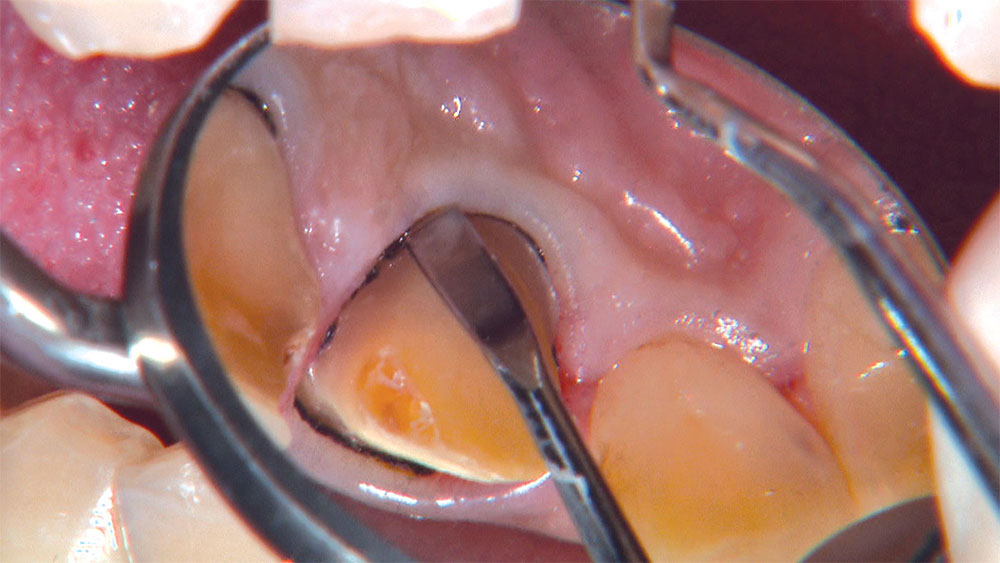
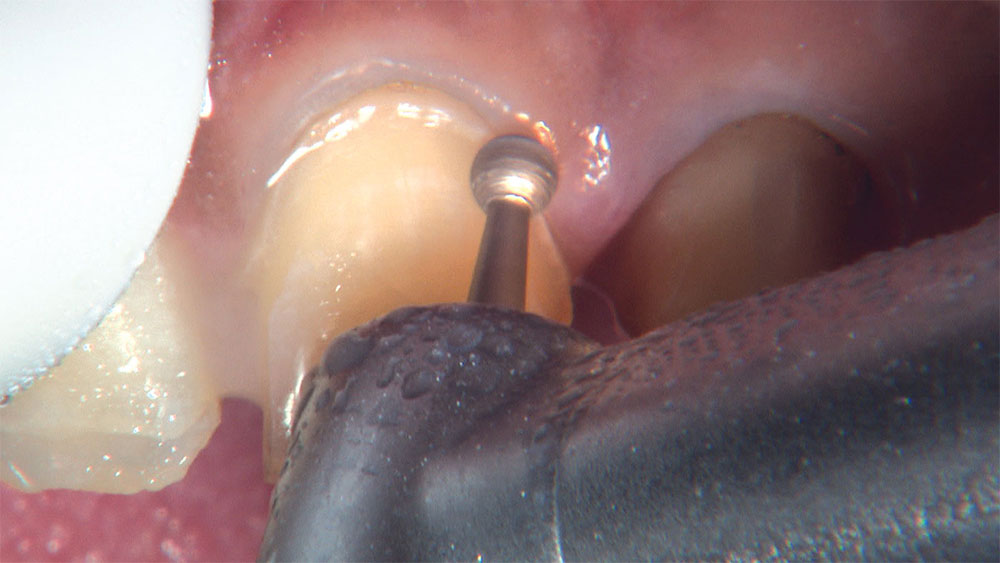
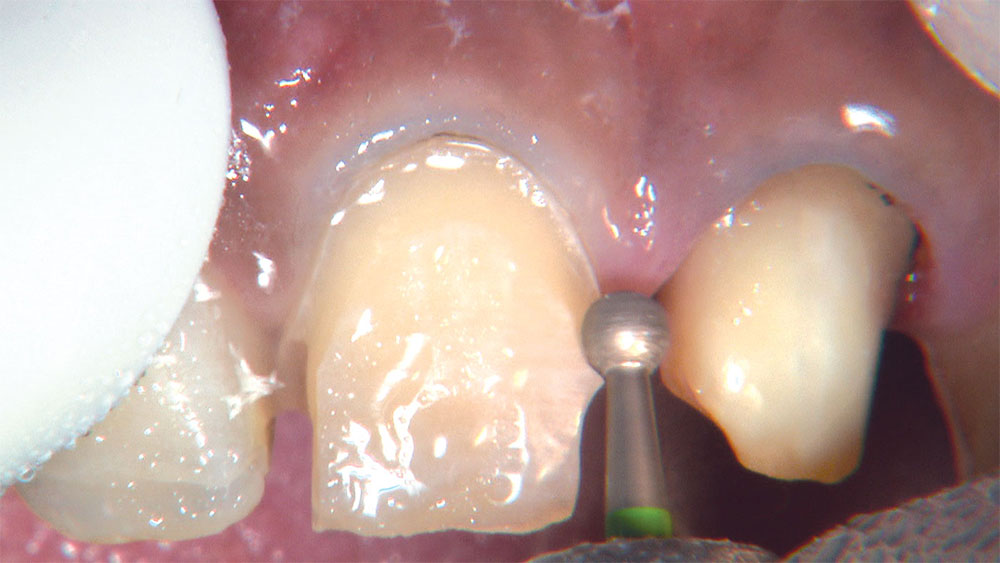
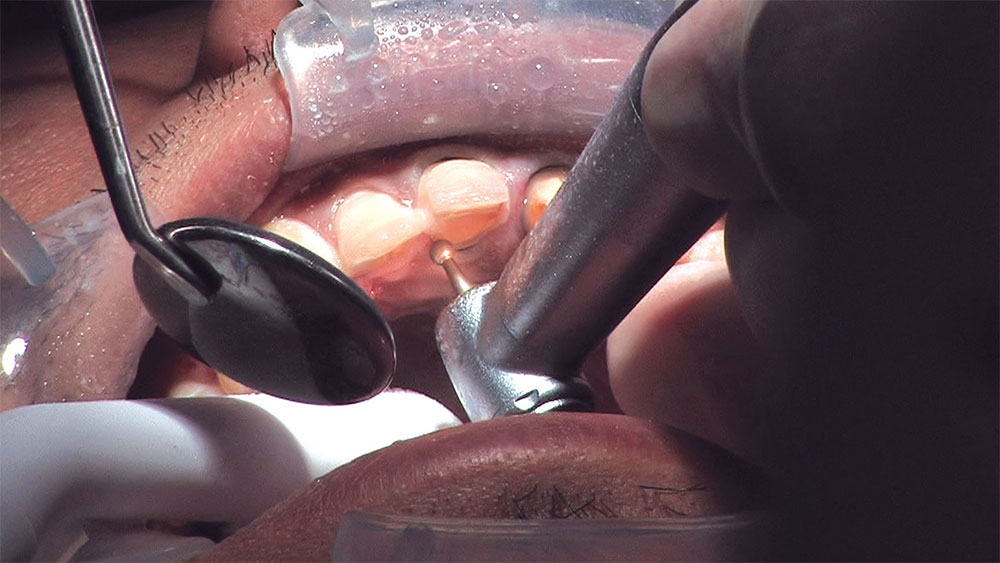
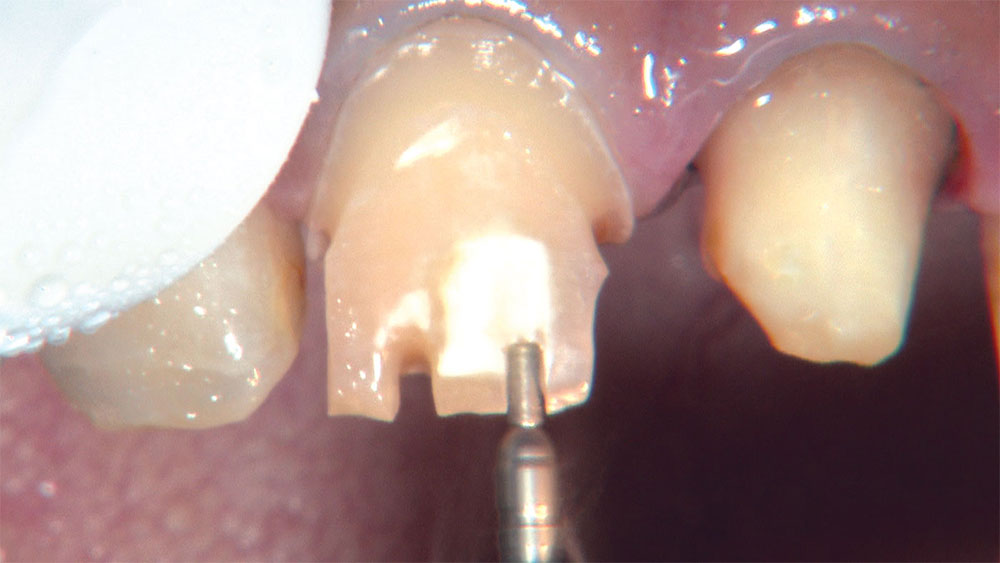
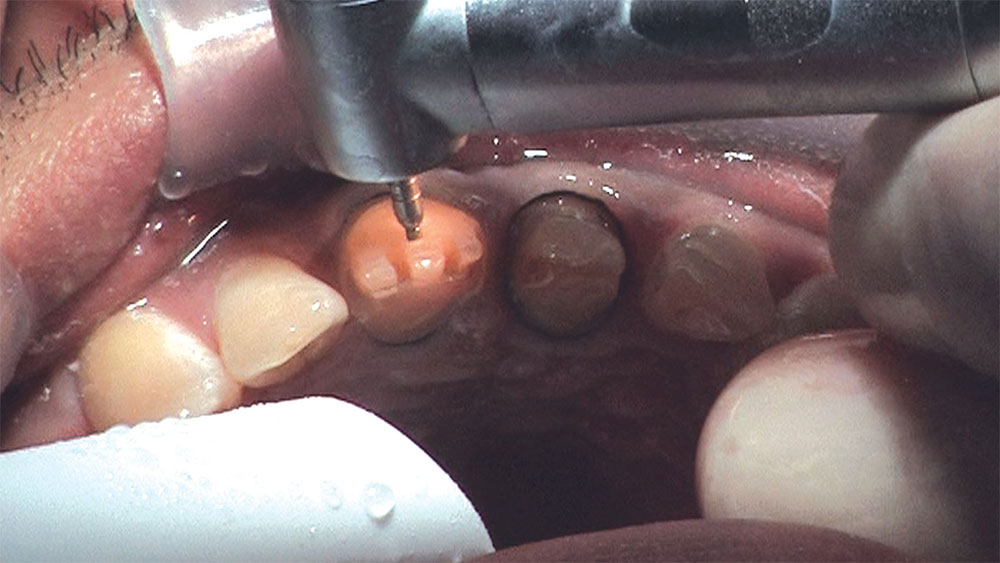
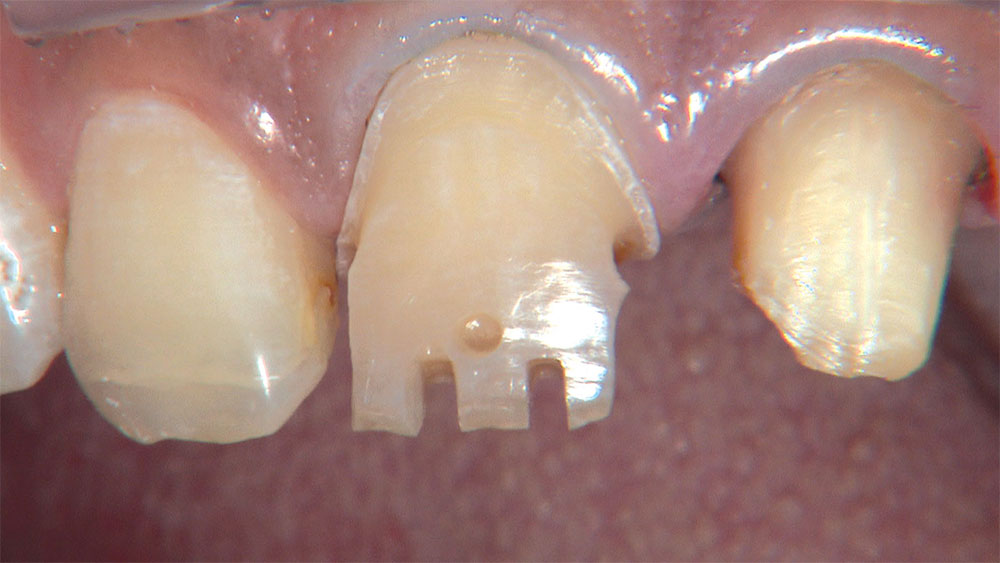
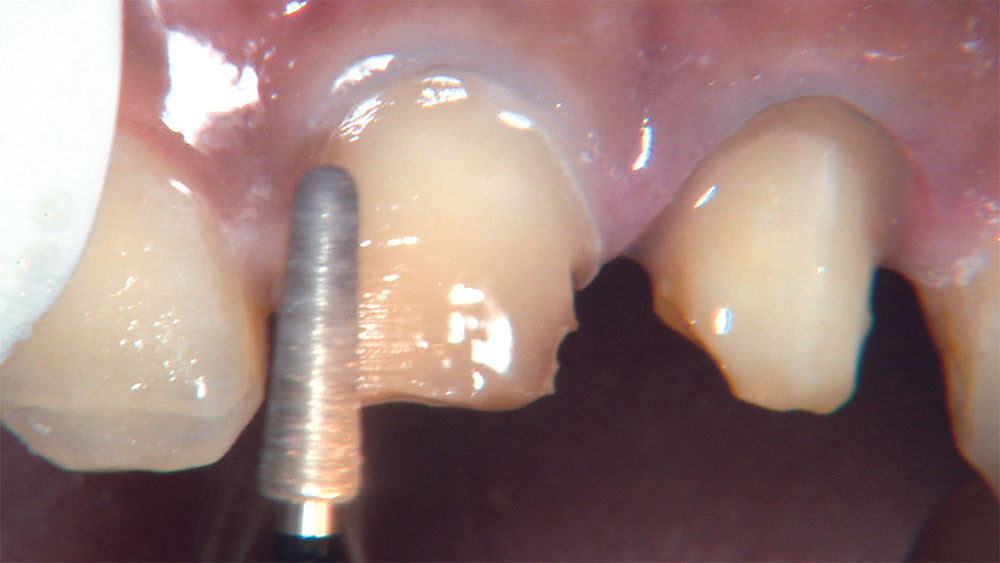
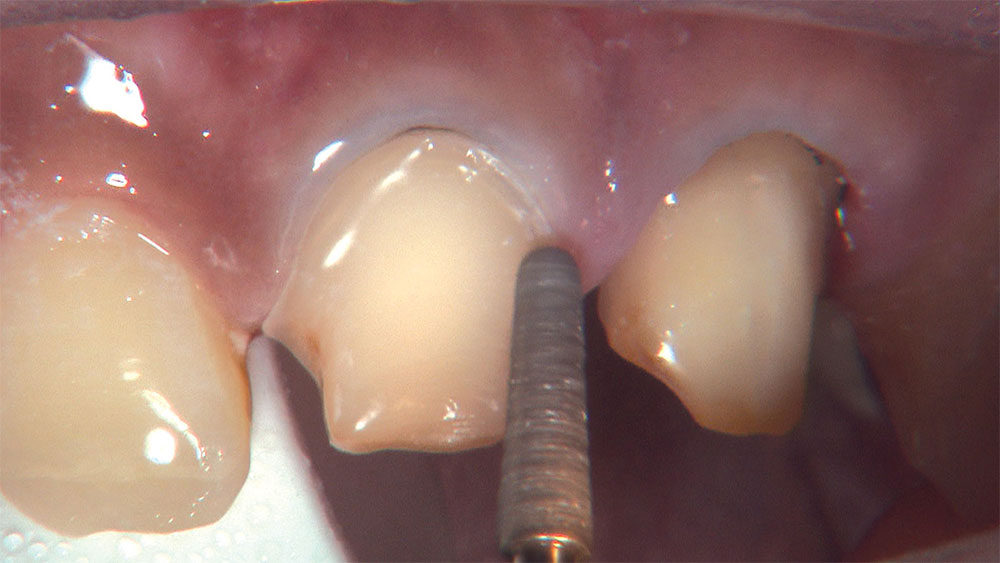
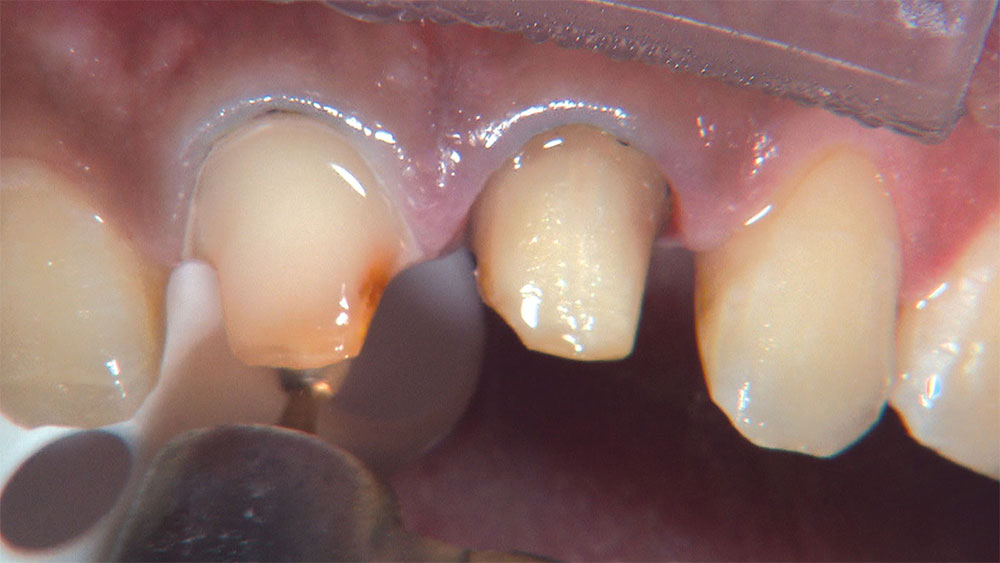
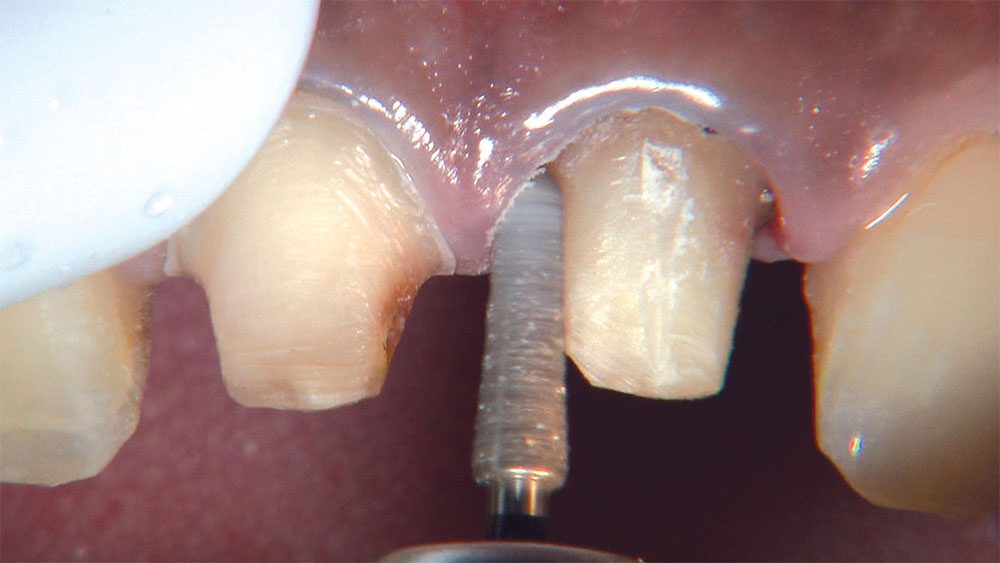
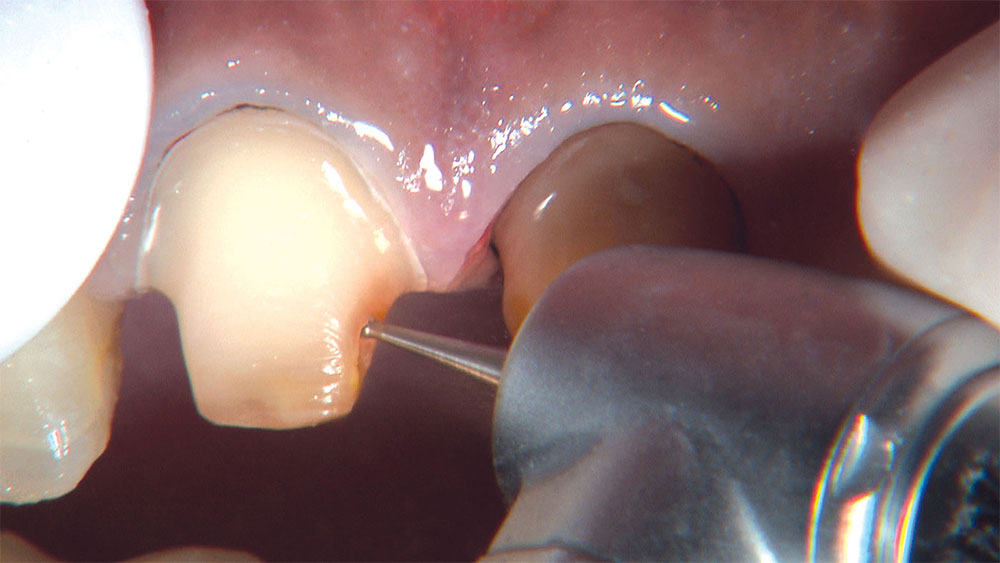
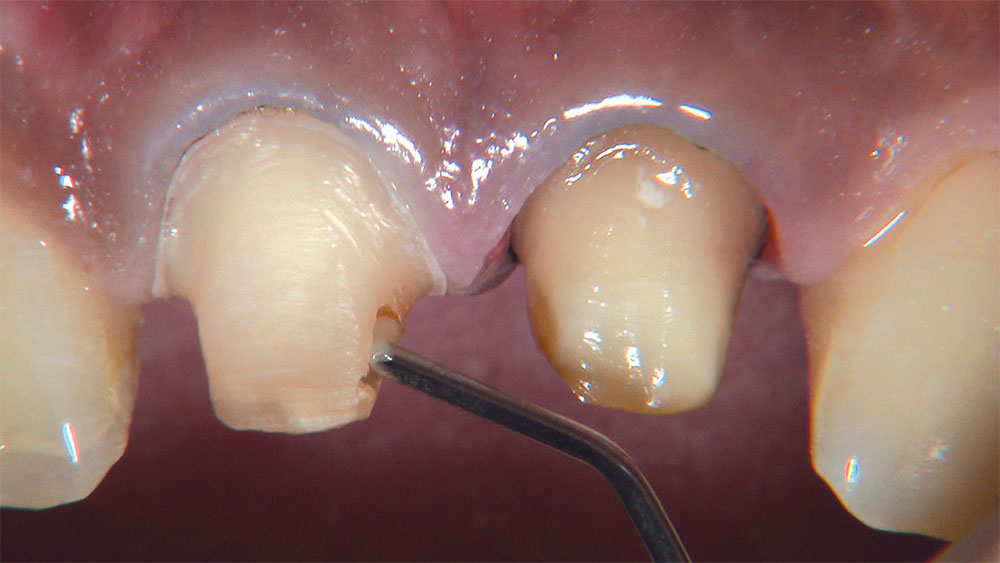
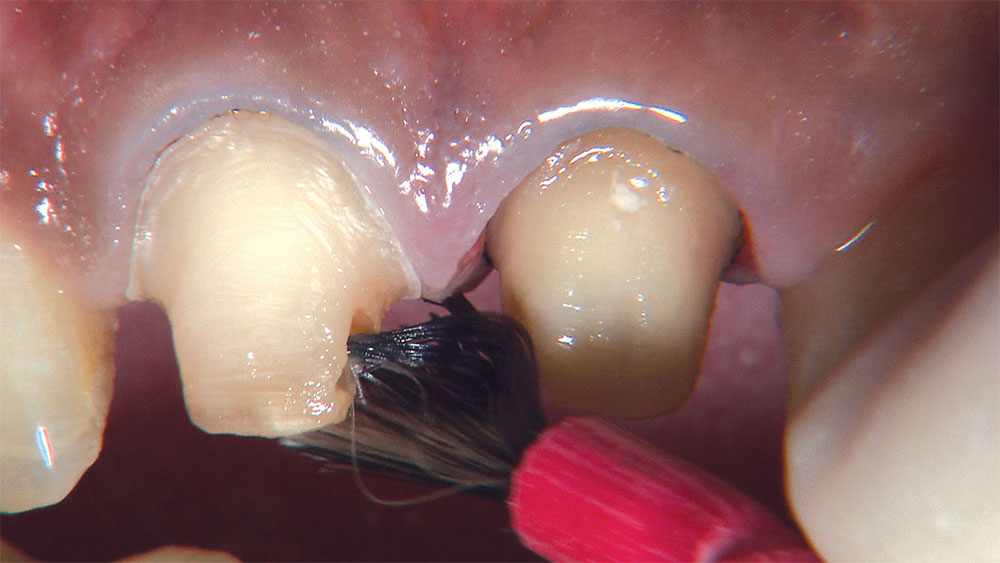
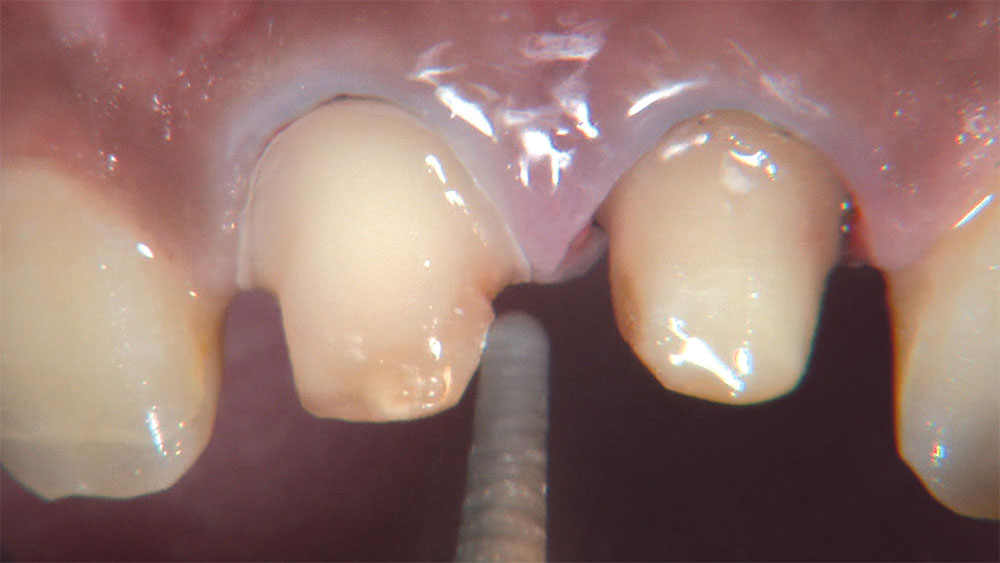
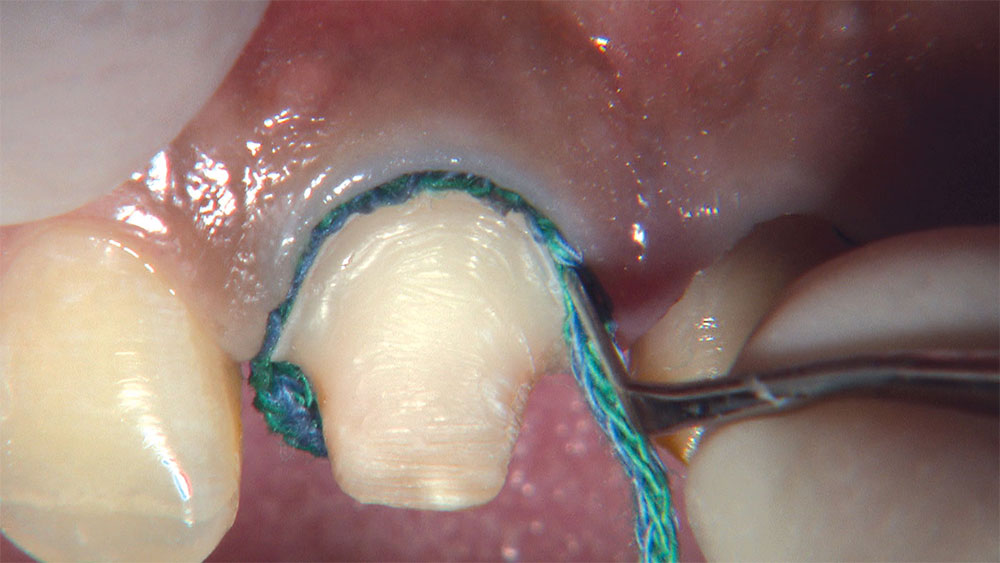
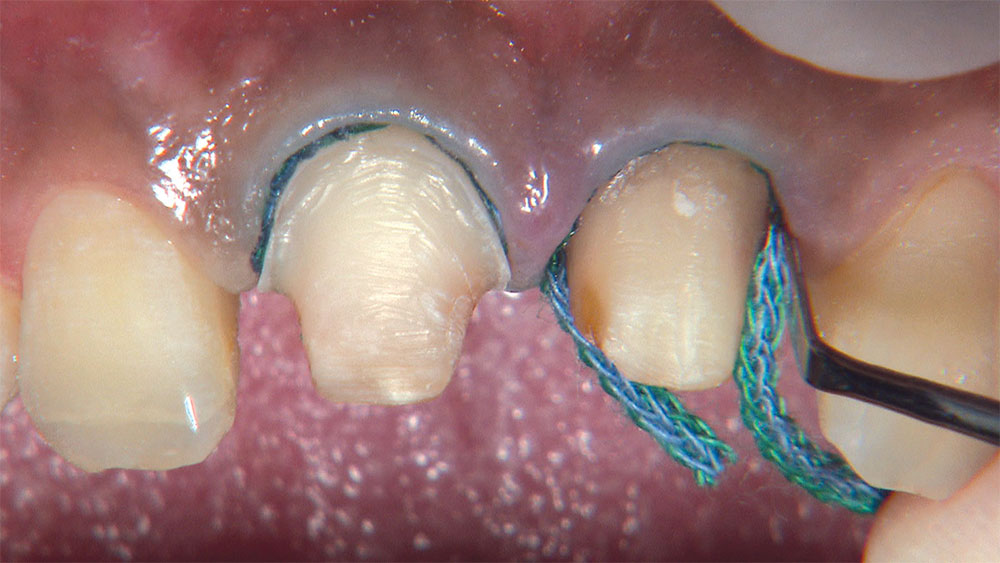
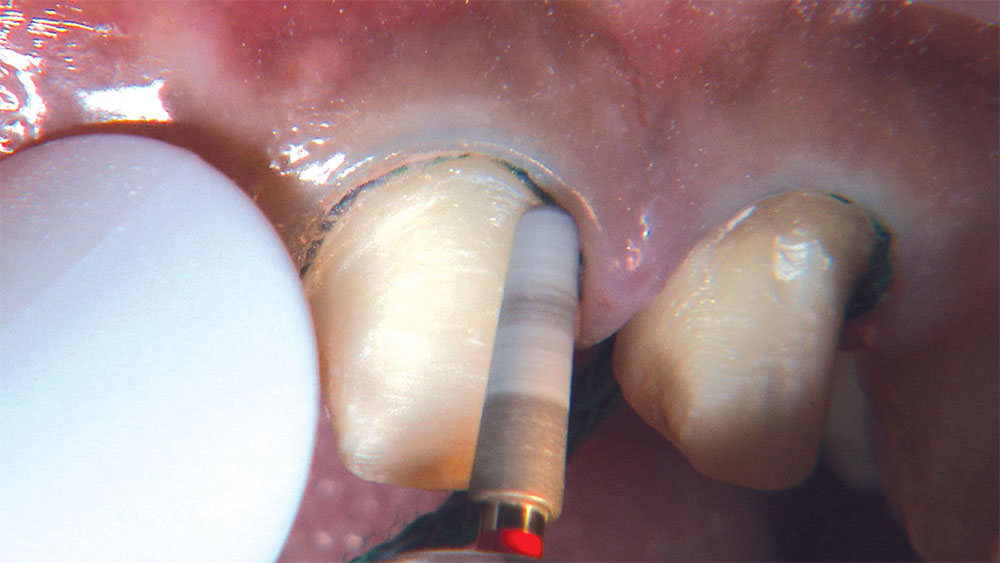
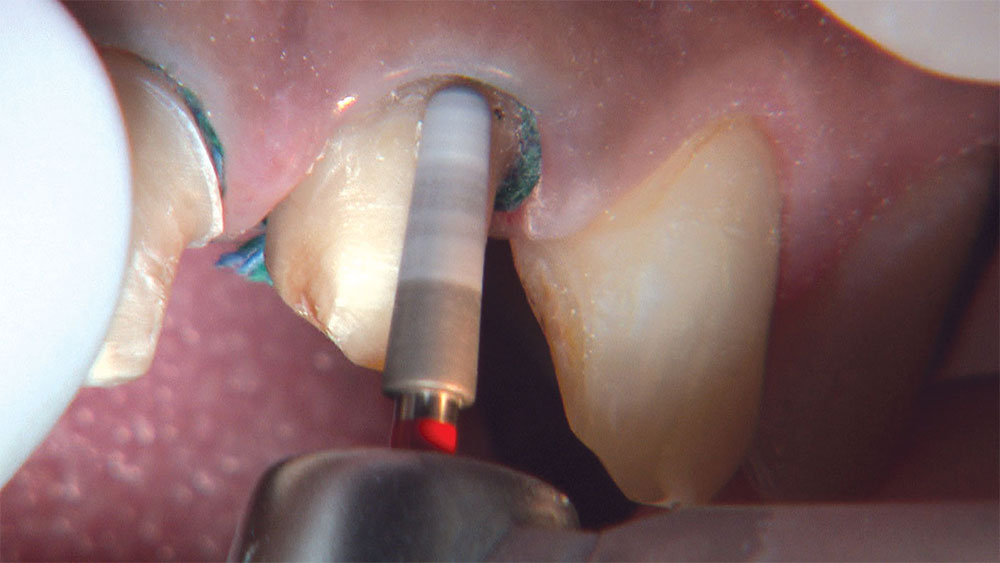
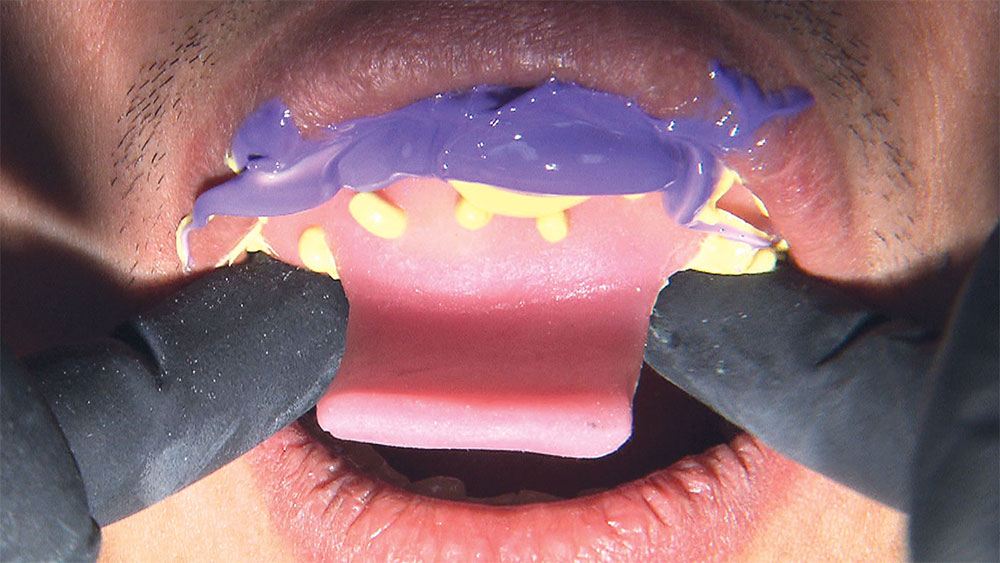
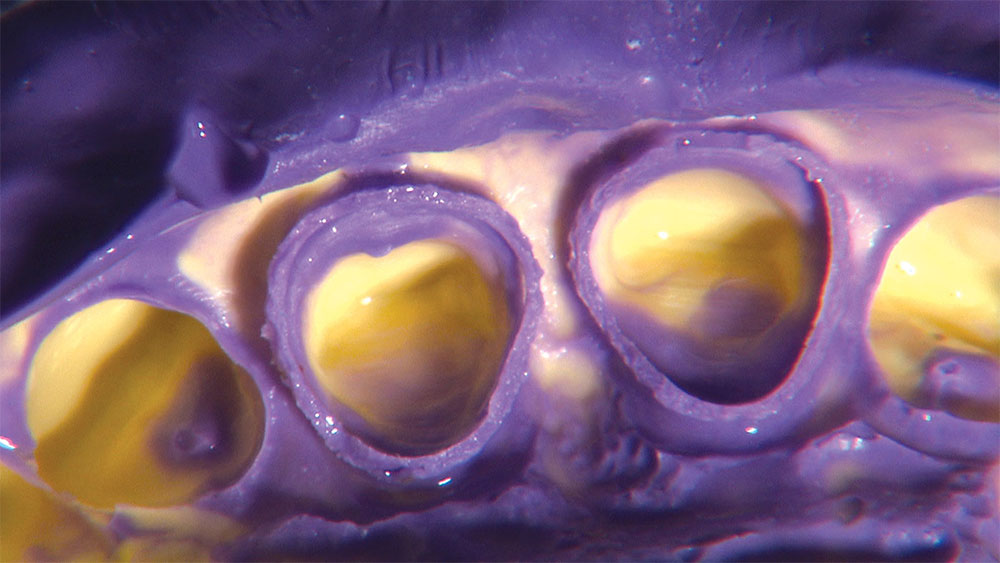
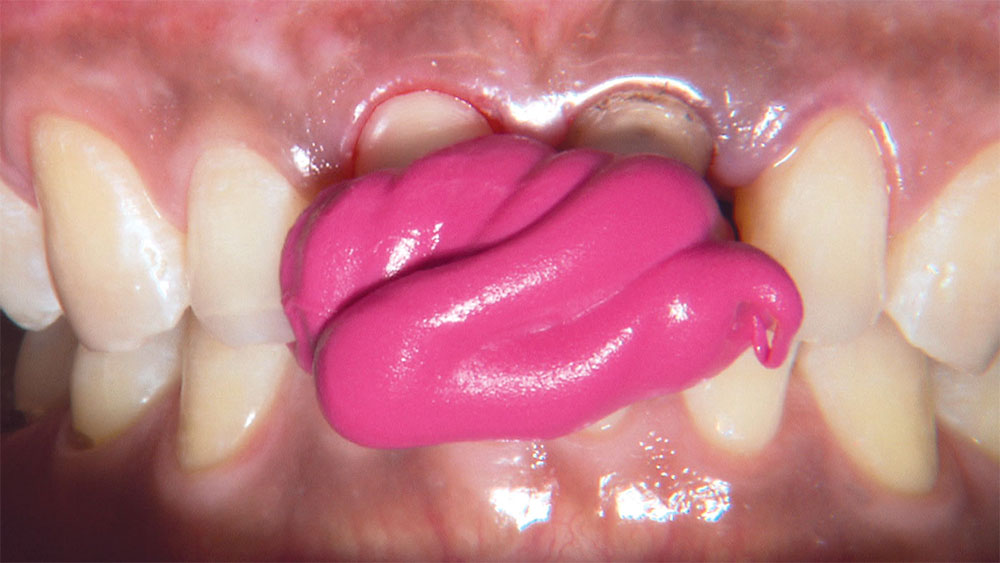
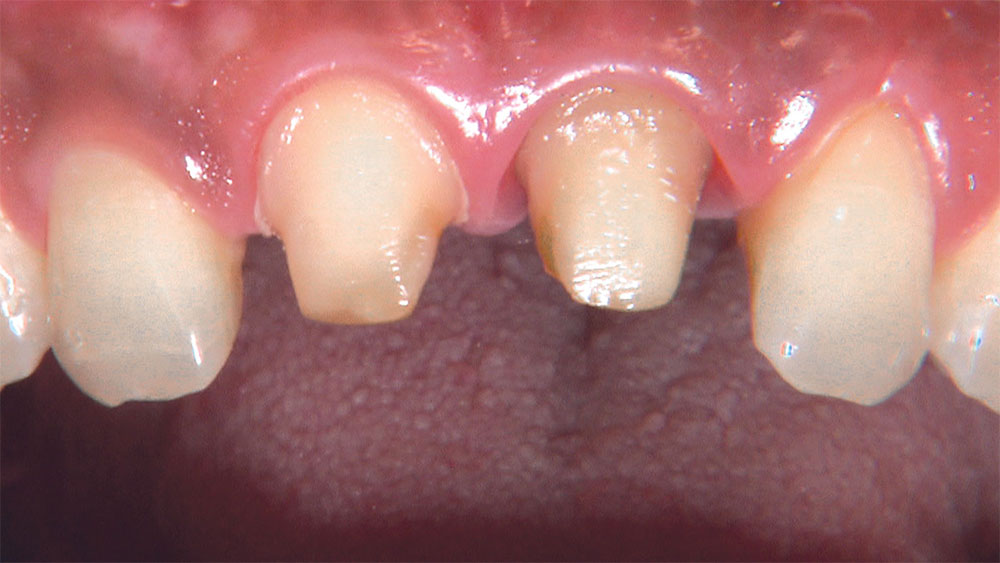
As I mentioned in the Editor’s Letter, an inadequate amount of reduction on crown and bridge preparations continues to be the biggest challenge faced by all of the U.S. dental laboratories that I communicate with regularly. In this case, I get to utilize the Reverse Preparation Technique on one of the crowns, but not on the other because the tooth was previously prepared. While working on a previously prepared tooth seems easier because some of the reduction has already been done, I know I have more control using the Reverse Prep Technique, where I always know exactly how much tooth I have removed. I am doing BruxZir® Anterior crowns on teeth #8 and #9; it will be interesting to see how they blend with the surrounding natural dentition.
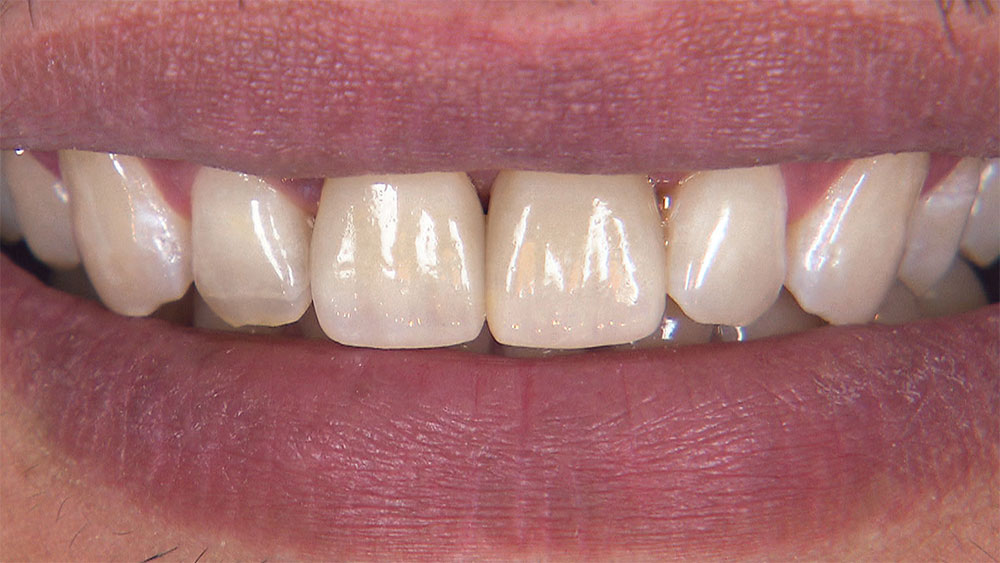
Figure 55: Here are the cemented final crowns on teeth #8 and #9. Having an in-house technician makes it easier for me to match the shade on these BruxZir Anterior crowns. The esthetics of BruxZir Anterior are great. In fact, it’s my go-to restoration in the esthetic zone; it has a higher flexural strength than lithium disilicate, and has translucency and color similar to natural dentition. We are getting ever closer to using high-strength monolithic materials for every indication.