A Better Quality of Life with Implant-Retained Overdentures
Introduction
The need for crowns, bridges and full dentures is steadily increasing, in part because the generation that filled schoolrooms in the 1950s is now arriving in great numbers in their dentists’ offices. Life expectancy in America is growing, and baby boomers are known for the premium they place on quality of life, so it’s not surprising that many will consider implant-supported prostheses. One way that dentists can meet the needs of a society in which 16% of the population is age 62 or older1 is to incorporate into their practices the use of small-diameter implants. Patients’ acceptance of prosthetically driven treatment plans increases when they are offered this minimally invasive and cost-effective alternative to conventional implants. The efficacy of small-diameter implants, along with resulting patient satisfaction, is supported by a growing body of clinical data.2,3,4,5 They have several advantages over conventional-size implants: Flaps or sutures are not required, so a general dentist can place them relatively easily and quickly, resulting in less pain and quicker healing for the patient; they can be placed in as little as 3 mm of bone in the buccal-lingual dimension, while the placement of conventional implants requires about 6 mm; they offer immediate loading6 due to being supported on both sides by cortical plates and because the auto-advancing design compresses and condenses the bone to help facilitate primary stability; multiple smaller-diameter (and mini-diameter) implants provide more stability than conventional implants if one loses viability; and small-diameter implants allow more patients to move ahead with implant-supported overdentures.
Case Report
Diagnosis and Treatment Planning
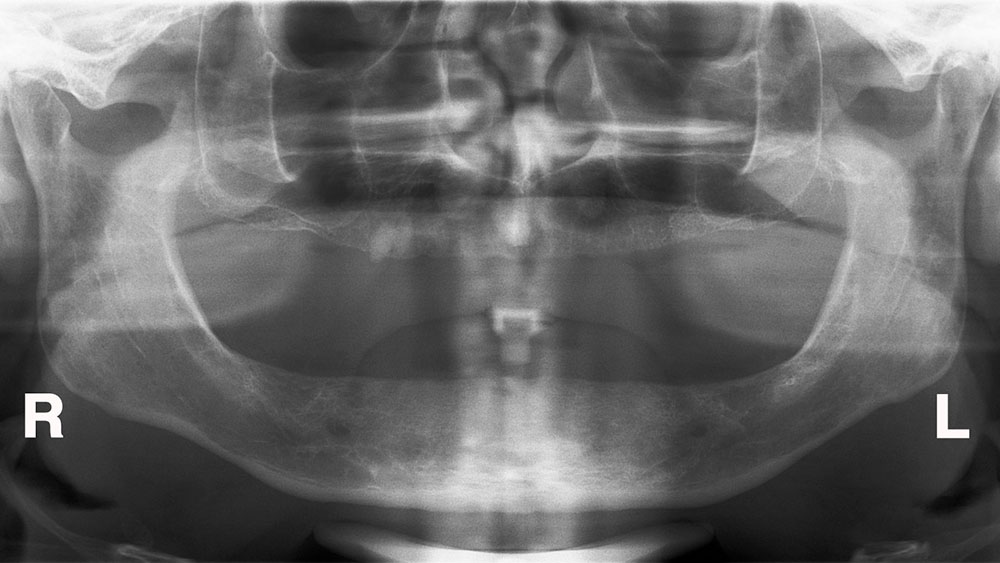
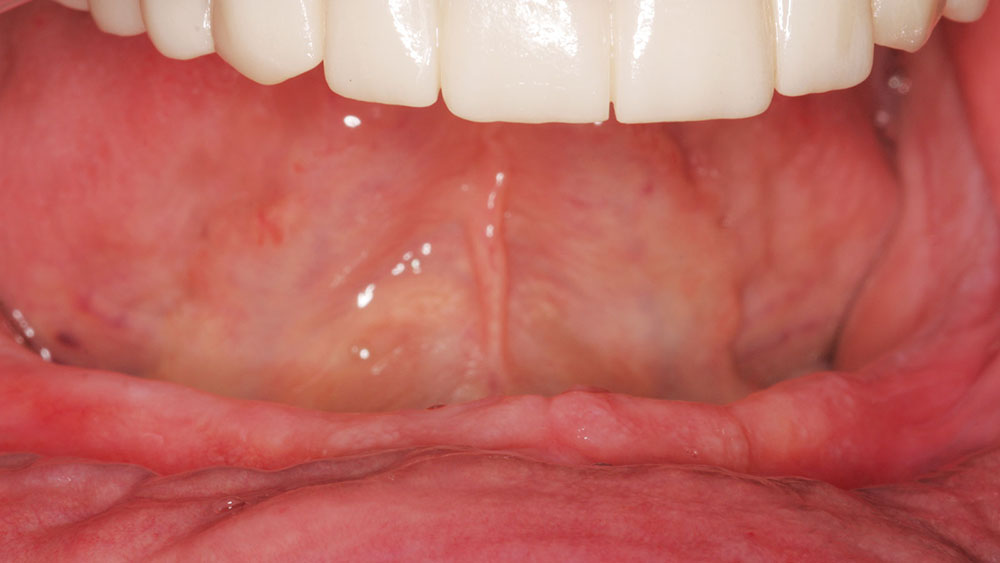
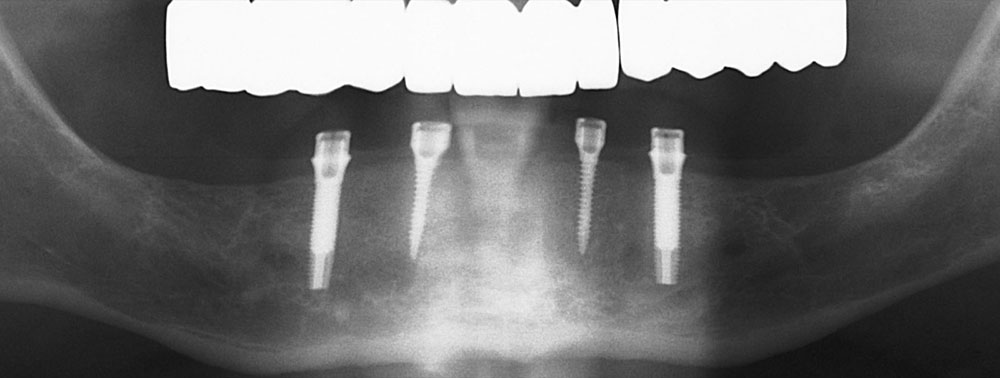
A 54-year-old male patient presented in good general health with a history of having had Bell’s palsy. He had all of his teeth extracted more than five years ago due to poor oral hygiene and lack of care (Fig. 1). He was dissatisfied with his dentures because they were nonretentive, and thus interfering with his ability to enjoy eating and to be in public without worry. His mandibular ridge was resorbed, but he had enough bone width to place two small-diameter and two mini-diameter implants in the anterior mandible. The height and width of bone was insufficient to place the conventional-size implant behind the mental foramen at the appropriate angle without additional surgery, indicating the need to place all four between the foramina (Fig. 2).
The implants chosen were a one-piece design with a Zest Locator® attachment (Zest Anchors LLC; Escondido, Calif.). The Zest Locator provides greater patient satisfaction while offering a self-aligning feature and a lower profile than the typical O-ball attachment.
Surgical Phase
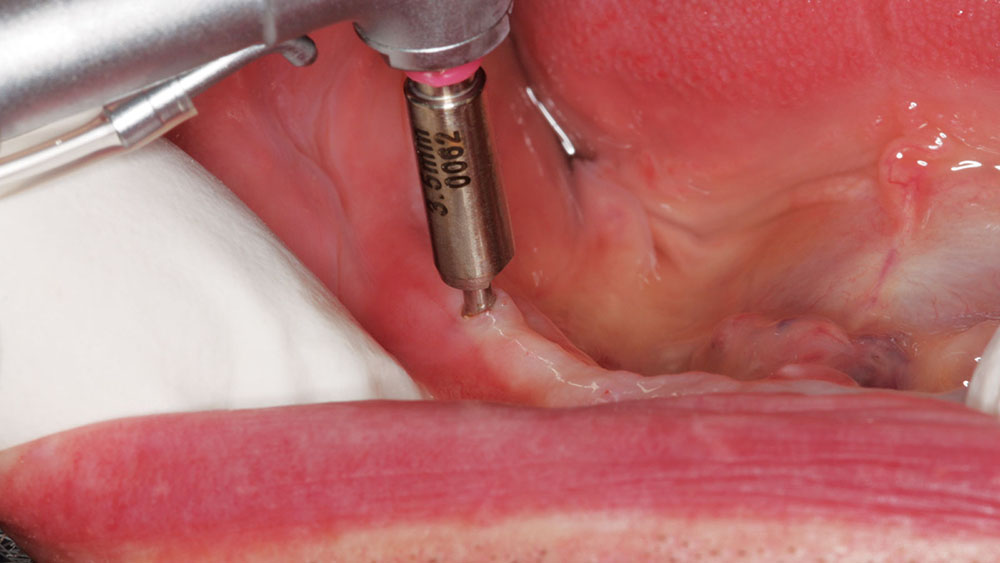
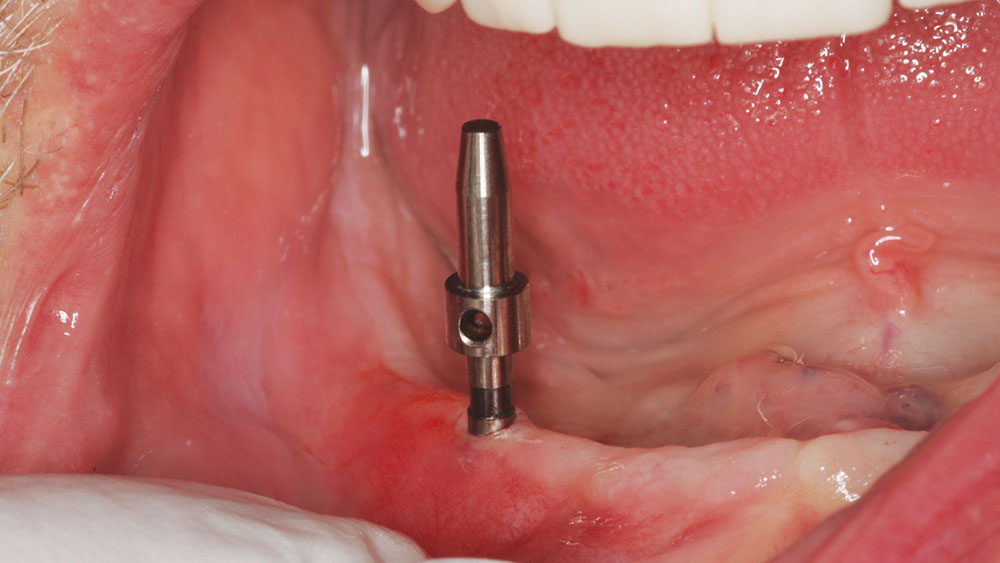
A periodontal probe was used at the original diagnosis/treatment appointment to determine the soft-tissue depth, which was reconfirmed at the surgery appointment. Ridge mapping was completed at a prior appointment, and it was determined that a flapless procedure could be performed. If complications were to occur, a surgical flap procedure could be initiated at any time. A tissue punch (OCO Biomedical; Albuquerque, N.M.) was used to gain access to the bony ridge instead of reflecting the soft tissue back (Fig. 3). A step pilot drill was then used to create the initial osteotomy for the small-diameter implant at 1,250 rpm in an implant handpiece (Nouvag MD 20 [Nouvag AG; Goldach, Switzerland]). The drill was taken to the length of the implant to be placed. A parallel pin (Salvin Dental Specialties, Inc.; Charlotte, N.C.) was placed to determine depth and to ensure that the final position of the Zest Locator would be at the correct angle (Fig. 4). A final 2.8 mm drill was used to depth to complete the drilling sequence. If there had been dense bone, a 3.25 mm bone tap could have been used to create a thread pattern in the bone that would replicate the thread pattern on the implant.
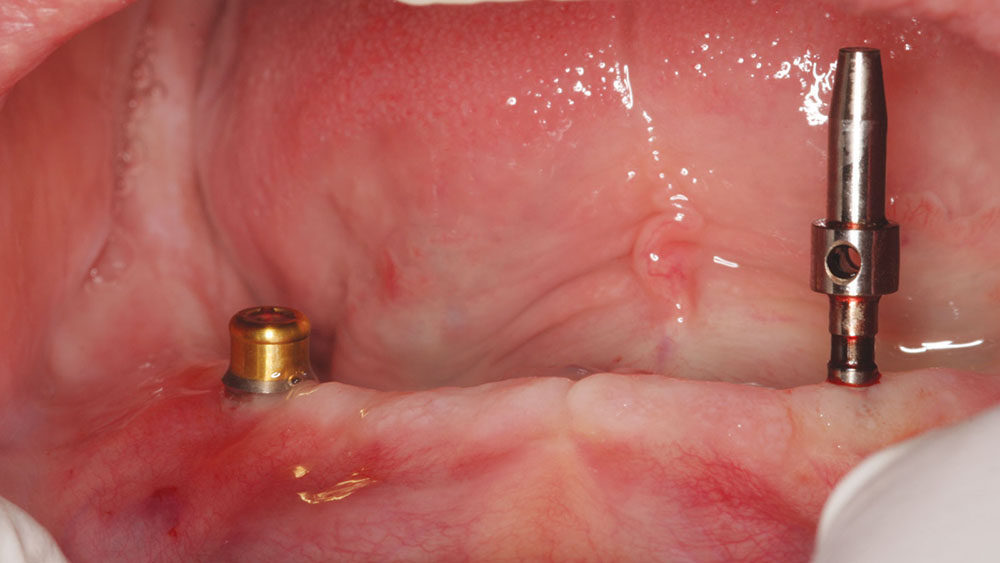
The sterile vial was opened so that the contra-angle driver engaged the Locator head without touching the implant. The vial was rotated and the implant removed, with the driver keeping the implant secure to the surgical site. The small-diameter implant was placed at 20 rpm with a maximum torque of 40 Ncm. Once fully inserted, the driver was removed.
The process was then repeated on the opposite side. Careful repetition of the process ensured the correct angulation and that the Locator attachments were the same distance from the front of the mouth.
The mini dental implants were placed following the same procedure but using a 0.8/1.6 mm diameter step drill. The drill speed was from 900 to 1,200 rpm, but the drilling depth was only 4 mm. The use of parallel pins helps to ensure correct angulation (Fig. 5). Up to 15 degrees between implants can typically be accommodated without undue stress on the implant-attachment-overdenture system (Fig. 6).
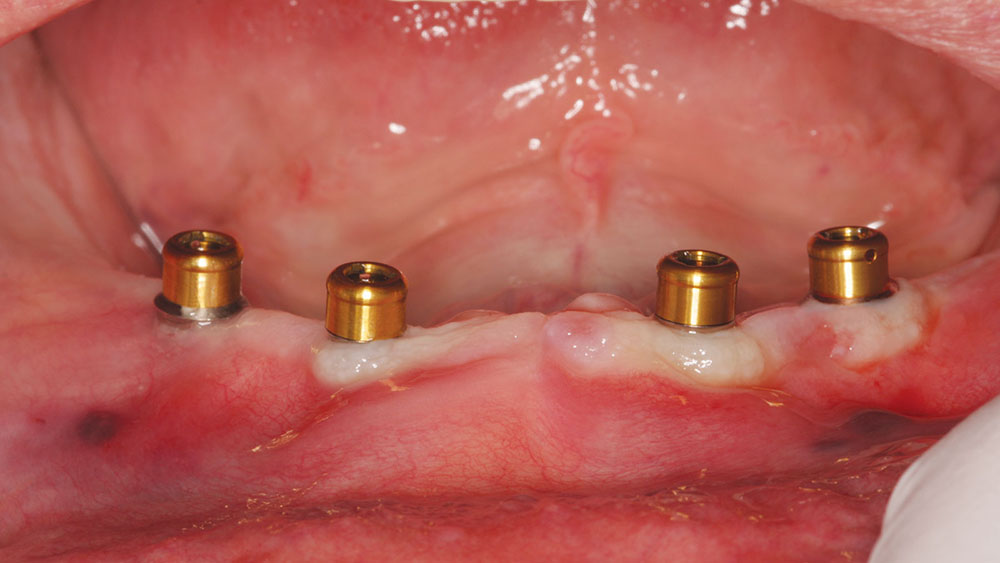
After completing the surgical phase, one appreciates finally having a mini-implant system available that incorporates the low-profile Locator attachment (Fig. 7). Patient satisfaction is greatly improved due to the self-aligning feature, and off-angle implants can be better managed by the clinician with extended-range nylon inserts.
Prosthetic Phase
For the prosthetic phase, a set of Locator impression caps was placed over the mini implants. These look like champagne glasses and communicate the exact location of the one-piece Locator implants to the dental laboratory team at Glidewell Laboratories. An impression was taken with soft putty (Capture® VPS Impression System [Glidewell Laboratories; Newport Beach, Calif.]) to ensure that all pertinent landmarks were captured, including land areas, retromolar pads, frenal attachments and, of course, the Locator impression caps.
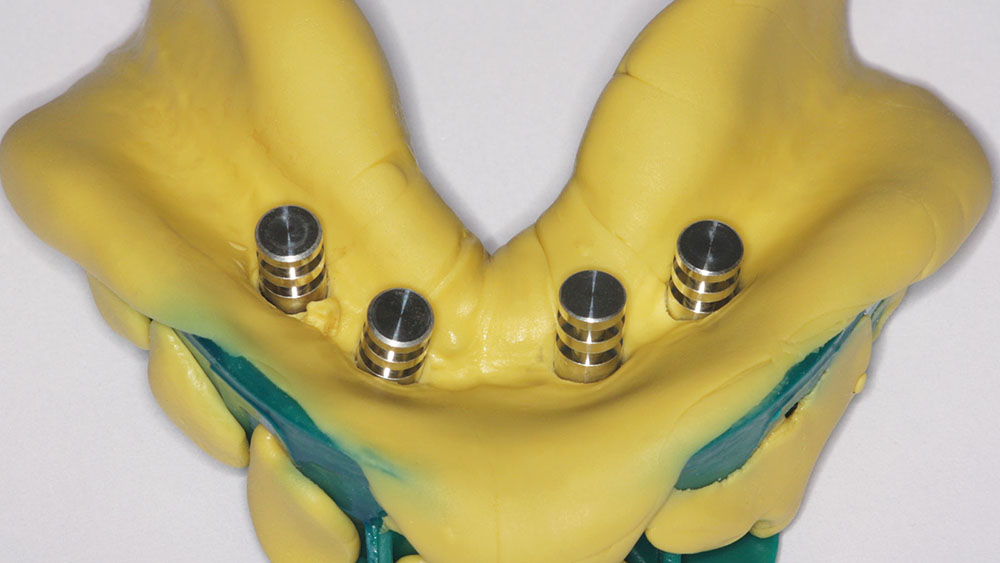
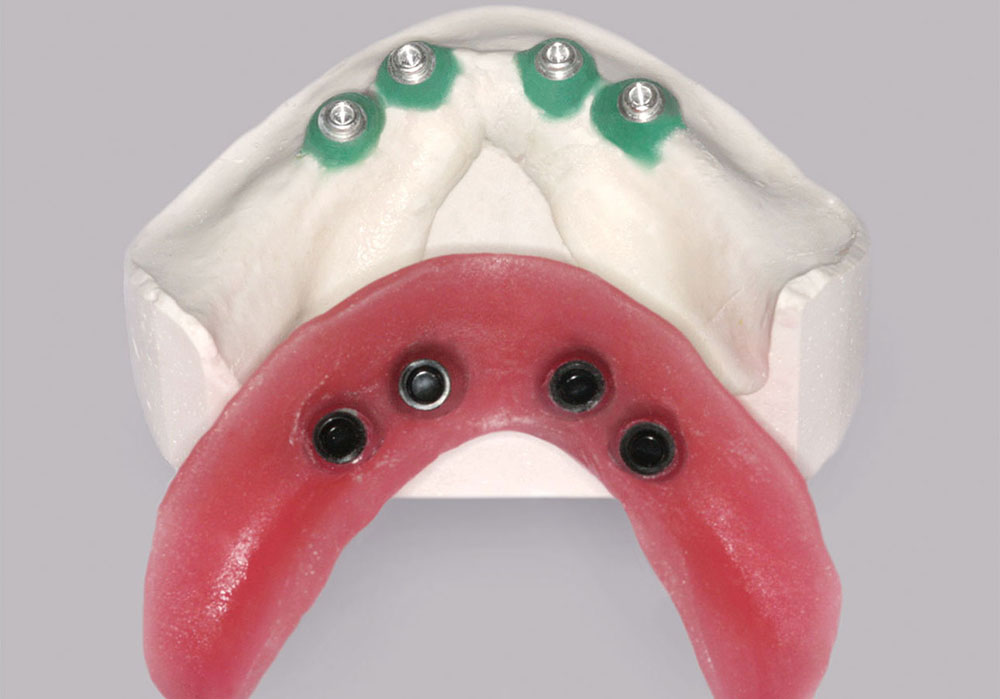
The Locator Lab Analogs (Zest Anchors) were then inserted into the impression caps (Fig. 8). A wax rim was made to record how the jaws came together and sent to Glidewell Laboratories to guide the team in placing the denture teeth for the optimal bite. The author asked the dental technician to incorporate the Locator housings into the acrylic base. This allowed the wax rim to be tried in and verified for fit and passive retention. If they had been incorrect, it would have been very easy to heat up the acrylic and to reposition the housing (Fig. 9).
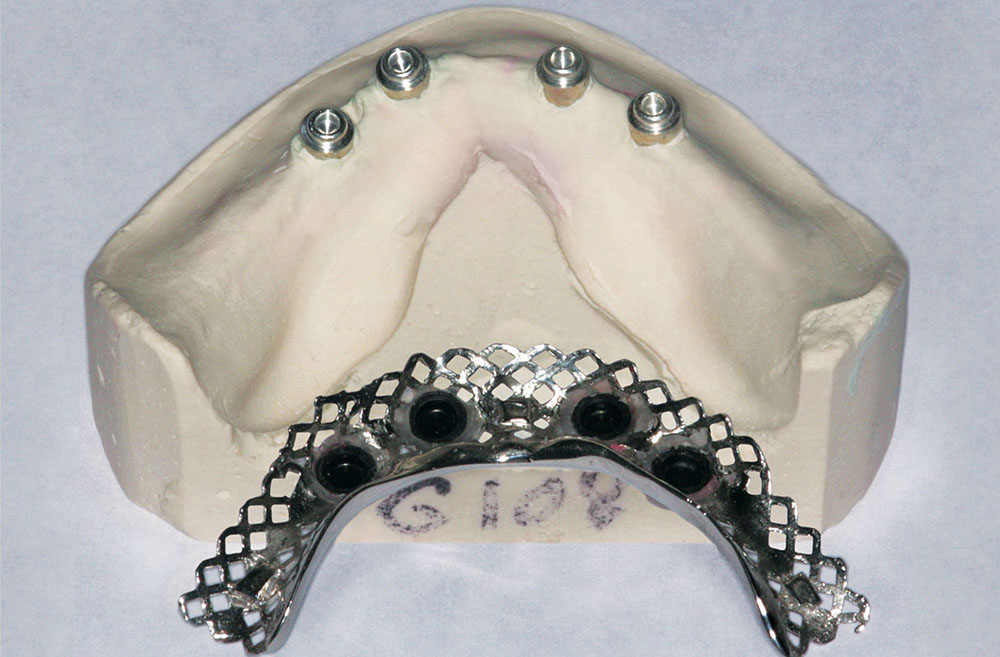
One of the complications that can occur with implant snap-in/snap-out dentures is fracture of the pink plastic. For this reason, the dental laboratory team was asked to incorporate a cast metal framework to increase the strength.
One of the complications that can occur with implant snap-in/snap-out dentures is fracture of the pink plastic. For this reason, the dental laboratory team was asked to incorporate a cast metal framework to increase the strength. Figure 10 shows the metal framework with the black processing rings embedded into the metalwork. These black “snaps” will be replaced with a more retentive nylon Locator ring.
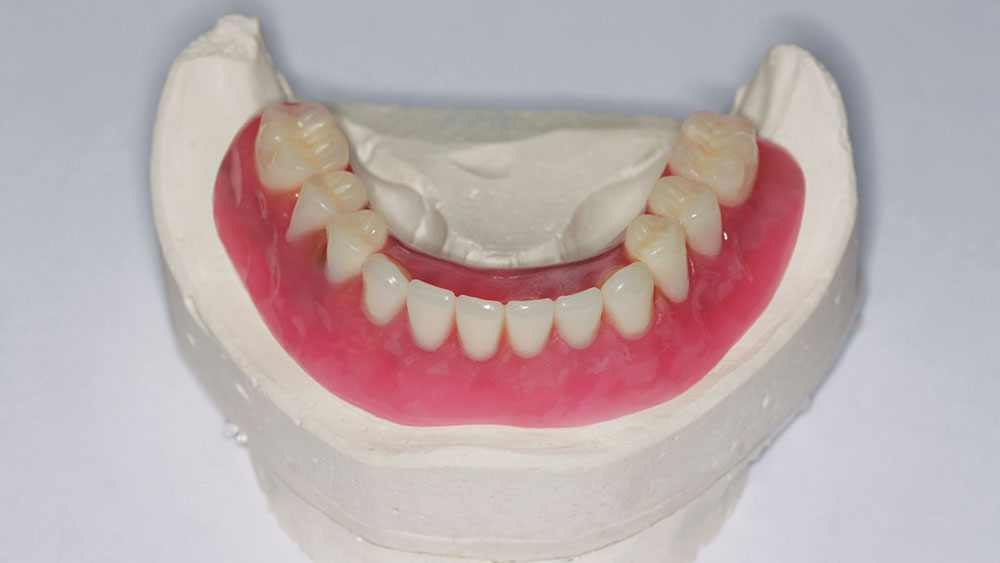
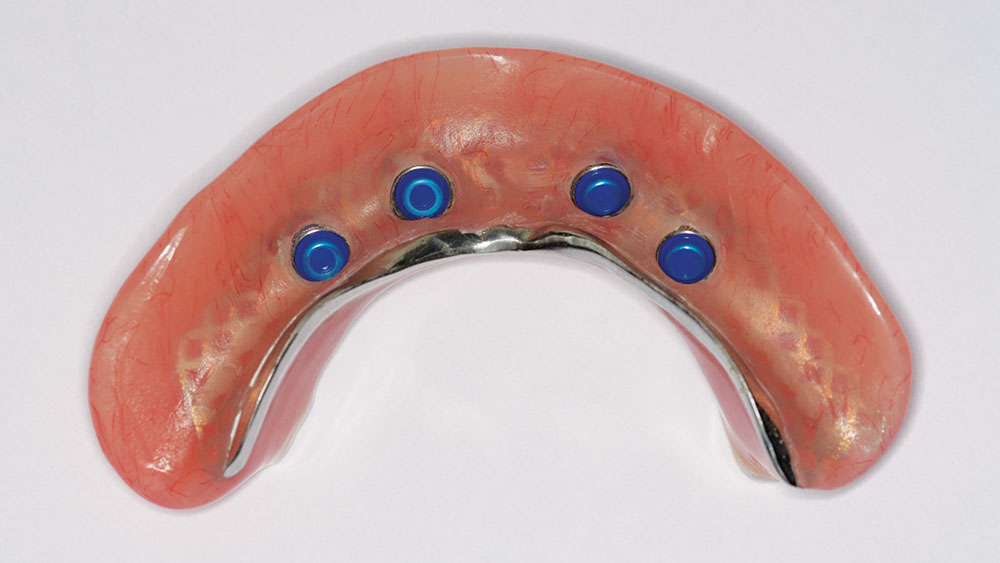
The bite was then taken from the wax rim, the Locator snaps were verified to ensure they fit over the implants, and the dental technician set denture teeth (Portrait® IPN® [DENTSPLY Prosthetics; York, Pa.]) in the wax for a try-in (Fig. 11). After patient approval of the wax setup, the denture was processed with an internal metal frame. At delivery, if the denture is too retentive, then different nylon rings can be placed to decrease the retention. If it is not tight enough, stiffer rings can be placed to increase it (Fig. 12).
The patient was highly satisfied. He experienced less pain and quicker healing than he had expected. After he had worn the lower denture for four weeks, he said he was relieved to be able to enjoy eating again and to be able to spend time with friends and acquaintances without the nagging worry that his loose dentures would cause him embarrassment.
Closing Comments
This patient’s quality of life was improved through utilization of some of the best technologies available today for implant overdentures. These technologies (including small-diameter implants, the Zest Locator attachment, a metal frame incorporated into the denture, high-quality composite denture teeth, and lab-processed attachments) will help general dentists successfully meet the needs of an aging population unwilling to let inadequate dentures compromise their lives.
Dr. Paresh Patel has placed more than 2,500 small-diameter implants and has worked as a lecturer and clinical consultant on mini implants for various companies. Contact him at pareshpateldds2@gmail.com or dentalminiimplants.com.
Disclosure: Dr. Patel reports no disclosures.
Dr. Brown has a private practice in Forth Worth, Texas, focused on implant and restorative care. He is president of the American Academy of Small-Diameter Implants and a diplomate of the International Academy of Mini Dental Implants. Contact him at 817-560-0414 or at stevebrowndds.com.
Disclosure: Dr. Brown reports no disclosures.
Dr. Nazarian maintains a private practice in Troy, Michigan, with an emphasis on comprehensive and restorative care. He can be reached at 248-457-0500 or at aranazariandds.com.
Disclosure: Dr. Nazarian reports no disclosures.
References
- ^Howden LM, Meyer JA; United States Census Bureau. Table 1. In: Age and Sex Composition: 2010 Census Briefs. Washington, DC: US Department of Commerce, Economics and Statistics Administration, US Census Bureau; Issued May 2011:2.
- ^Misch K, Neiva R. Small-diameter implants for optimal stabilization of implant-supported overdentures. Pract Proced Aesthet Dent. 2007 Aug;19(7):428-31.
- ^Shatkin TE, Shatkin S, Oppenheimer AJ, et al. A simplified approach to implant dentistry with mini dental implants. Alpha Omegan. 2003 Oct;96(3):7-15.
- ^Bulard RA, Vance JB. Multi-clinic evaluation using mini-dental implants for long-term denture stabilization: a preliminary biometric evaluation. Compend Contin Educ Dent. 2005 Dec;26(12):892-7.
- ^Nazarian A. Mini dental implants: immediate gratification for patient and provider. Dent Today. 2005 Oct;24(1):110, 112.
- ^Ahn MR, An KM, Choi JH, Sohn DS. Immediate loading with mini dental implants in the fully edentulous mandible. Implant Dent. 2004 Dec;13(4):367-72.
Reprinted by permission of Dentistry Today, ©2012 Dentistry Today.