Optimizing Occlusal Results for Crown & Bridge Prostheses
When preparing a single-unit crown or multiple-unit bridge, dentists inevitably follow a similar routine. The prepared teeth are impressed in a good-quality impression material, such as a polyether, or the most widely used impression material, an addition silicone vinyl polysiloxane (VPS),1 which accounts for 95% of the impressions sent to the dental laboratory.2 The impressions are taken in a full-arch stock or custom tray, the bite registration is taken after the preparations are completed, and an opposing model is fabricated from alginate to allow mounting of the case in the laboratory. The prosthesis is then returned to the dental practitioner and inserted. If it is found to be high in occlusion, the dental technician is often blamed for an error in technique.3 In reality, it is the built-in variability of the above technique sequence and material selection, which is still routinely taught in many dental faculties, that leads to clinical frustration and valuable time wasted in trying to make the unit(s) “fit.” Why is it that a 12 times greater accuracy in the maximal intercuspal position is found with the dual-arch cast?4
This article looks at the “normal” sequence described above, identifies the variables and describes how to minimize them.
Bite Registrations
Why is it that as dental students we are taught to take the bite registration after tooth preparation and after the patient has been anesthetized? This approach certainly makes sense for extensive restorations, or when involving terminal teeth in the arch as abutments for a multiple-unit restoration. However, if the clinician is preparing a single-unit restoration, which represents the majority of the crown & bridge impressions at dental laboratories,5 why not take the bite registration before the patient is anaesthetized and still has proprioception? In doing so, there is an increased likelihood that the casts will be mounted in the patient’s acquired centric. In addition, if the dentition is intact, the working stone model of the single preparation will be mounted more accurately using this bite registration.
Why is it that as dental students we are taught to take the bite registration after tooth preparation and after the patient has been anesthetized?
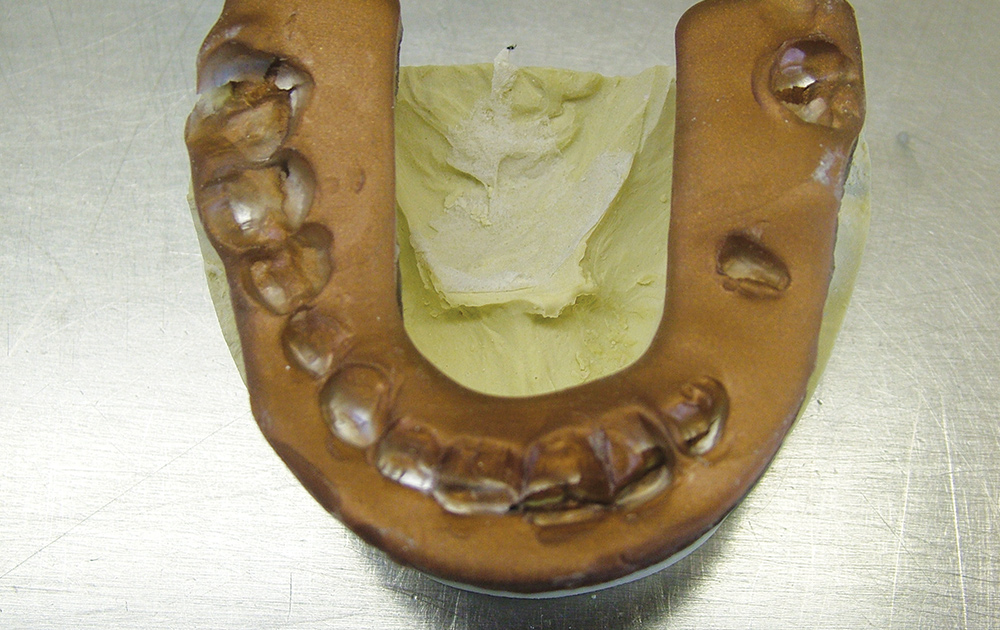
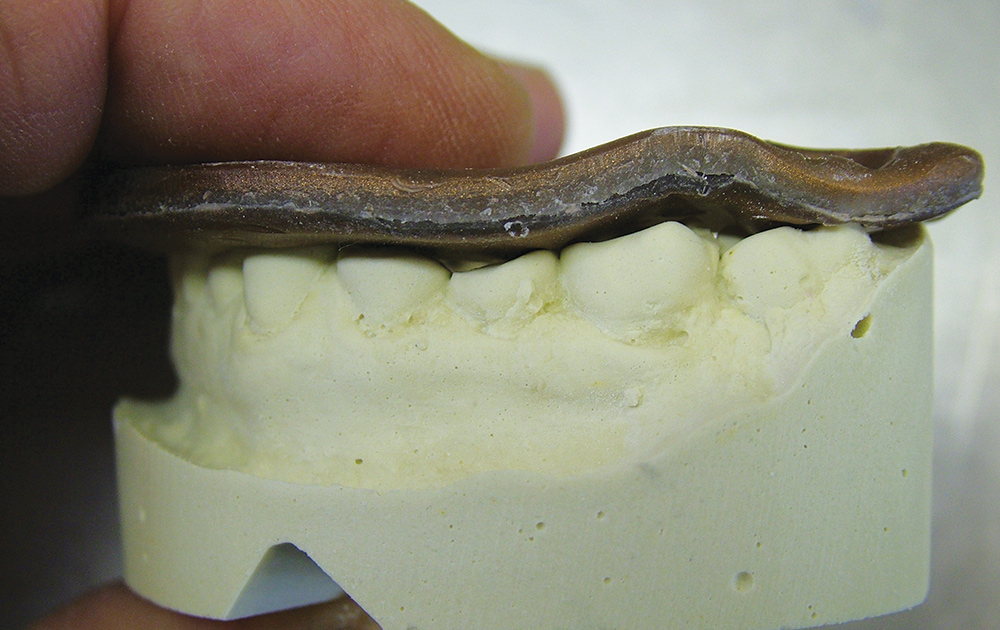
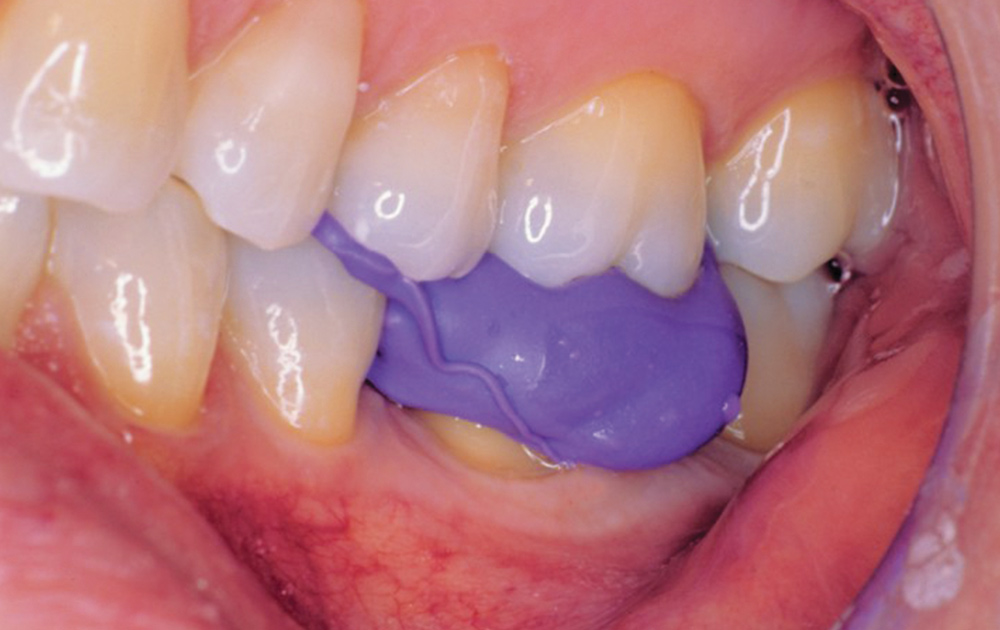
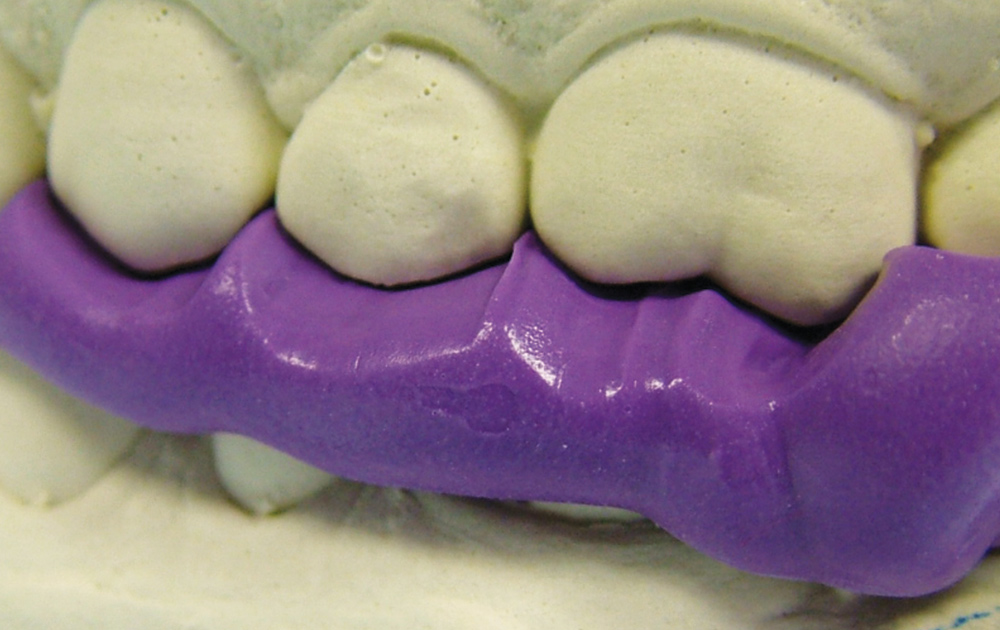
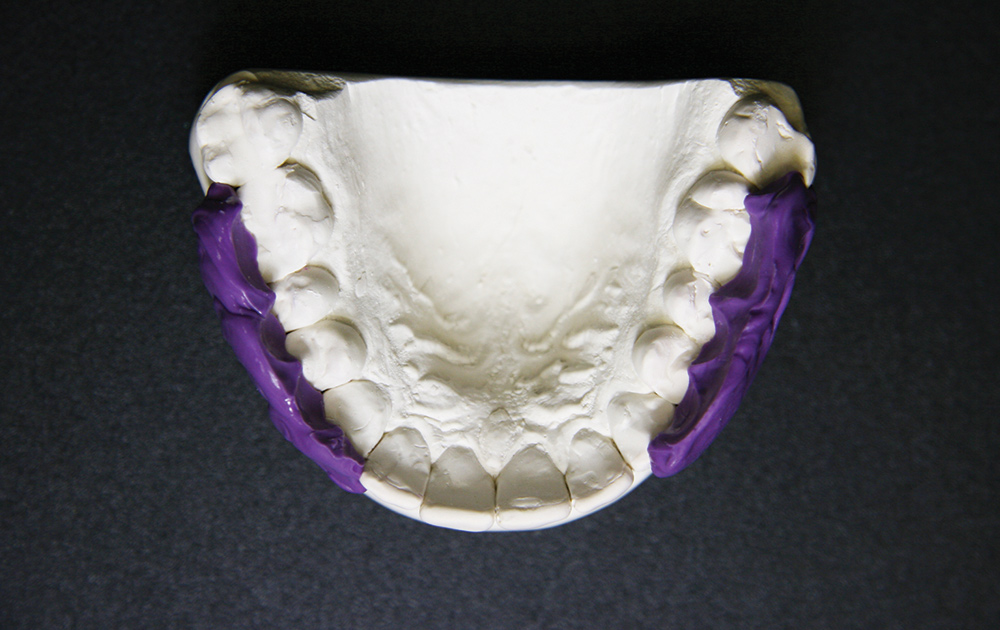
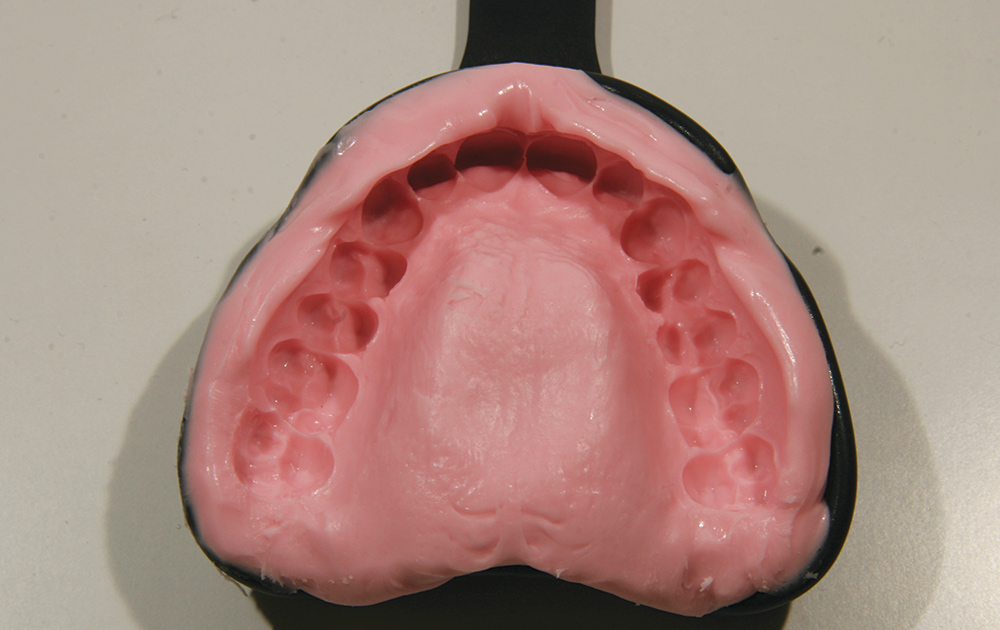
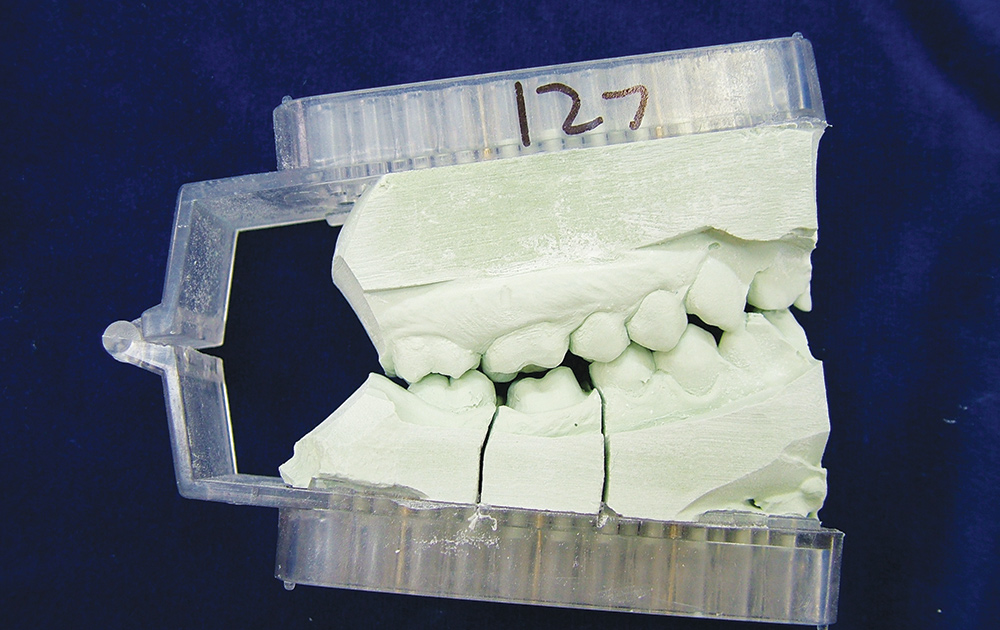
Bite registration or interocclusal records are taken with many different registration materials in many different ways; can the dental laboratory technician actually use them to relate the models in their proper orientation? Laboratories still receive wax bite registrations, which are unreliable due to dimensional changes when cooling.6 Furthermore, wax bite registrations are easily distorted on removal from the mouth, in transit or with temperature changes (Figs. 1, 2).7 The use of resin copings to record centric relation has been described by Anselm Wiskott and Nicholls,8 and a comparison between using impression plaster, wax and DuraLay acrylic resin (Reliance Dental Mfg. Co.; Alsip, Ill.) showed that hand articulation was the most accurate method of relating casts to maximum intercuspation.9 The use of polyether bite registration materials has been shown to result in vertical discrepancies in the interocclusal relationships of casts.10 Elastomeric materials may deform11 or distort when pressure is applied during mounting of a case (elastics are often used to hold the casts together), resulting in faulty restorations.12 Of course, VPS impression materials, designed to flex when withdrawing a full-tray impression from the mouth, cannot be used. It is critical not only for these bite registration materials to be dimensionally accurate but to be very stiff to resist distortion (such as AFFINITY™ Quick Bite [Clinician’s Choice; New Milford, Conn.], which has a durometer hardness of 90). When looking at impression materials — VPS Imprint™ Bite (3M™ ESPE™; St. Paul, Minn.), Silagum Automix Bite (DMG America; Englewood, N.J.), O-Bite (DMG America), Blu-Mousse® Classic (Parkell; Edgewood, N.Y.), Exabite™ II (GC America; Alsip, Ill.); one polyether, Ramitec™ (3M ESPE); and one dimethacrylate base material, LuxaBite® (DMG America) — Chun, et al.13 found that these materials presented significantly different polymerization shrinkage kinetics and showed dimensional changes even after the setting time indicated by the respective manufacturers. However, a study by Millstein and Hsu14 looking at Coe Bite Crème (GC America), Blu-Mousse, Correct Bite (Pentron Clinical Technologies), Blue Velvet (J. Morita; Irvine, Calif.), Memosil D.D. (Heraeus Kulzer; South Bend, Ind.), and Ramitec showed that all brands were highly accurate and dimensionally stable.
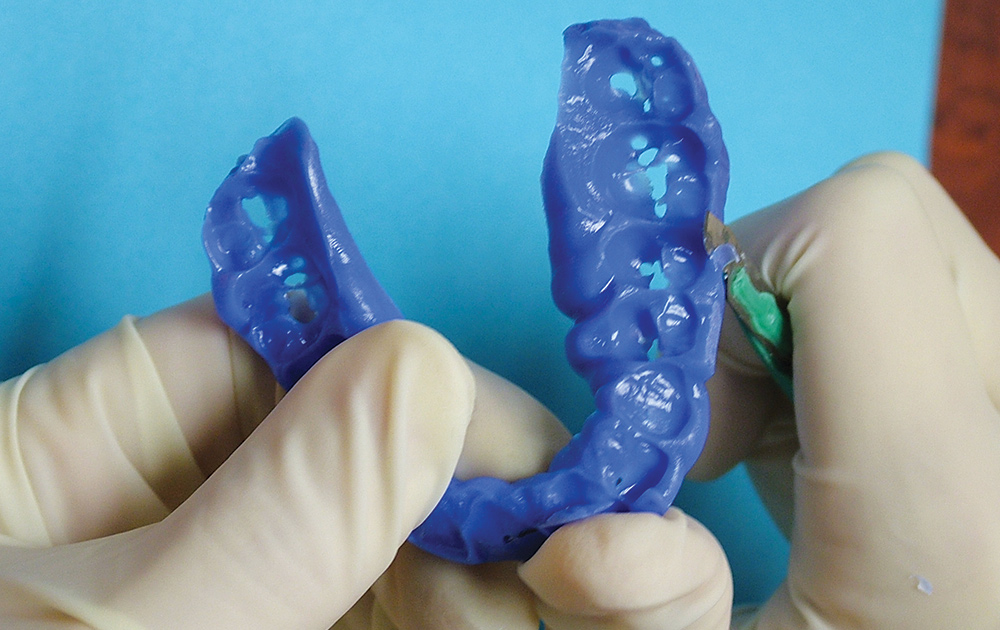
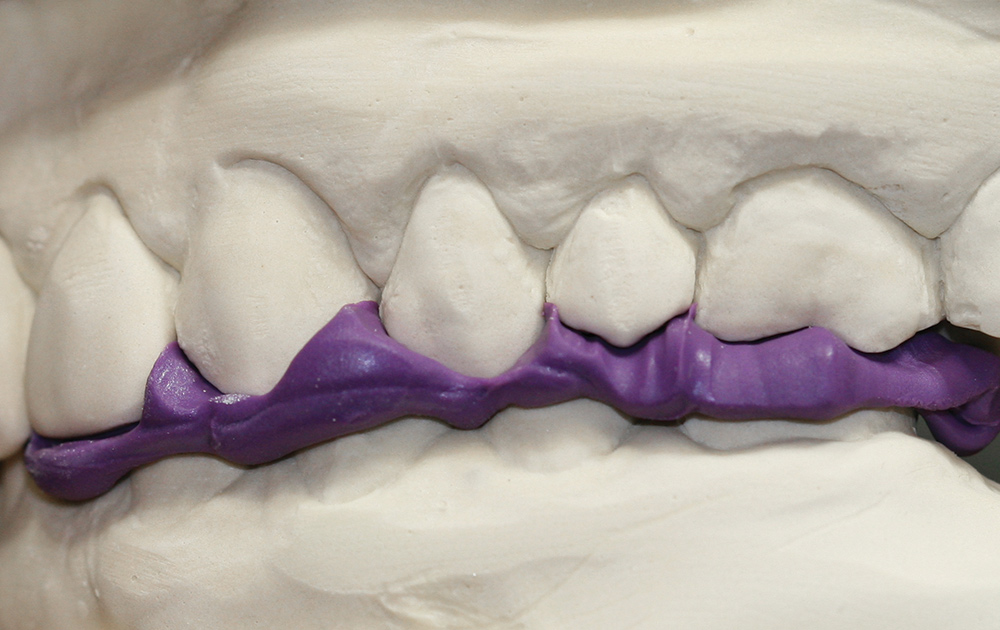
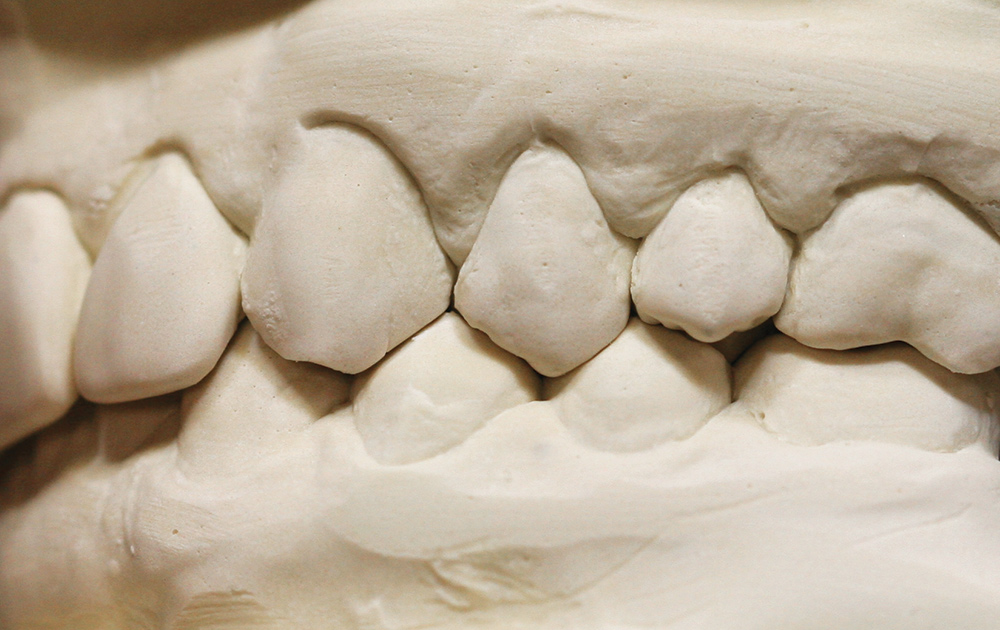
Dr. Gordon Christensen3 recommends the interocclusal record be trimmed so as to eliminate all material that touches soft tissue (Fig. 3), that extends to undercuts (Fig. 4) and that extends more than a tooth or two beyond the prepared teeth (Fig. 5). However, the advice of having a bite registration material between teeth on one side and not the other can cause an inaccurate mounting of the opposing models.
Opposing Casts
As mentioned earlier, for crown & bridge cases, most dental practitioners take the impression of the opposing arch in alginate. Alginate impressions can contribute significantly to a fixed partial denture (bridge) being too high.3 The quality of the alginate is compromised by a myriad of factors that include: the powder-to-liquid ratio is difficult to control, which affects flow, resultant accuracy and working time; the water temperature affects the speed of set and flow characteristics; syneresis (water leaving the gel) continues after the material is set, causing dimensional changes15; distortion occurs after a short time if the alginate is not poured up immediately16; the alginate can distort if disinfected17-21; if poured up in the office, the quality and dimensional stability of the resulting cast depends on the waterto-powder mix, as well as the method used for mixing of the dental stone22; the stone used in the office is not as accurate as the die stones used in the laboratory; the impression is not stable, as it is affected by temperature and humidity23-25; the type of tray used affects clinical accuracy26,27; and the use (or nonuse) of adhesives affect the final outcome.28,29
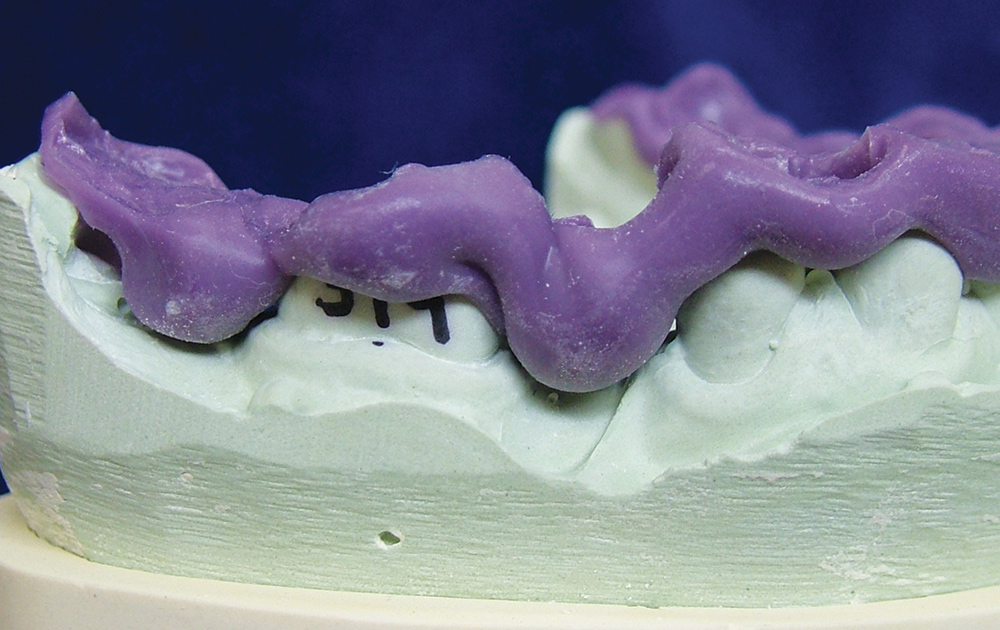
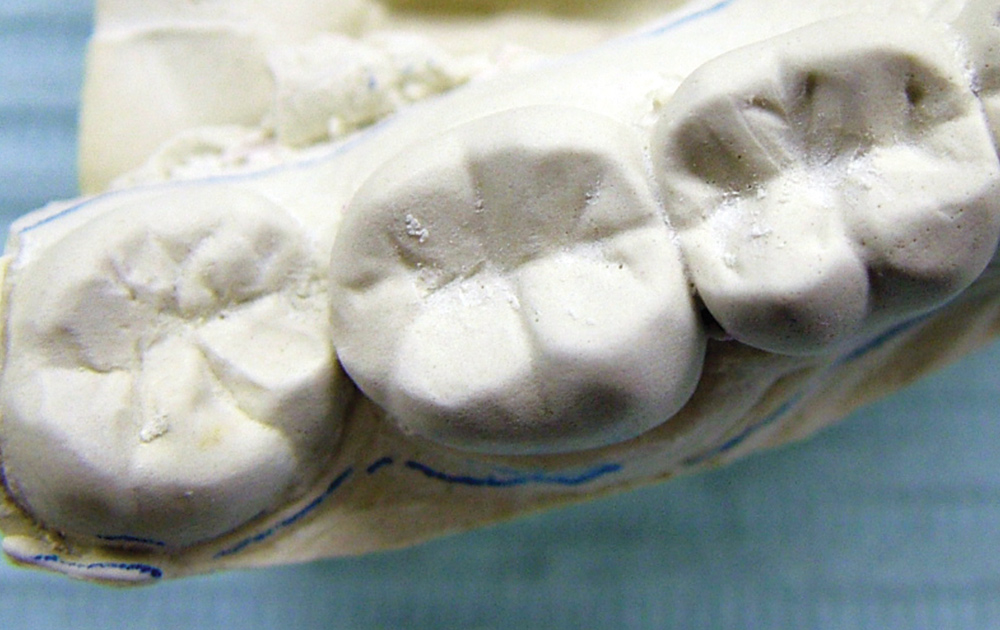
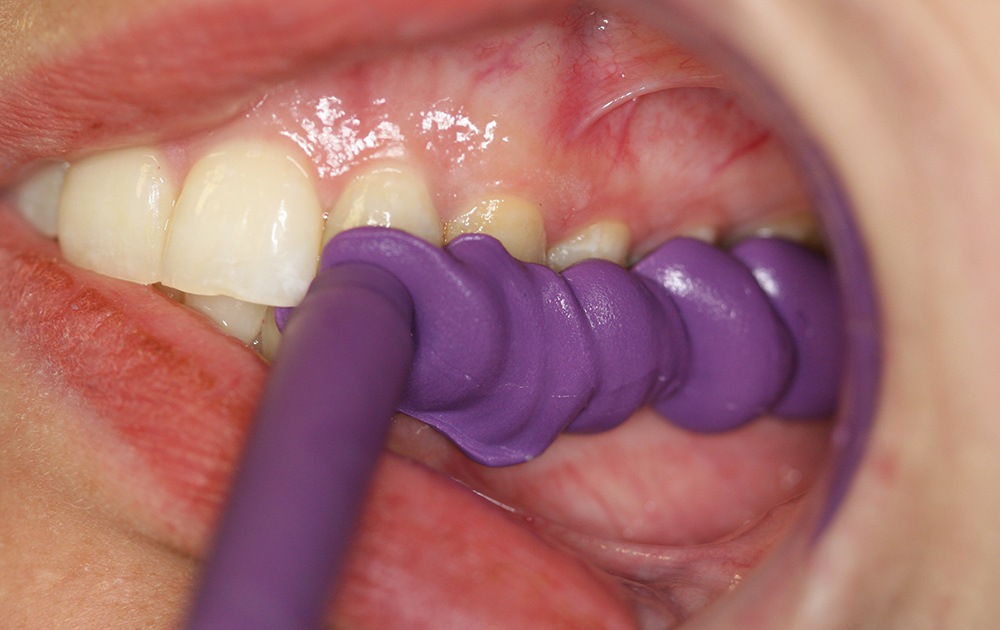
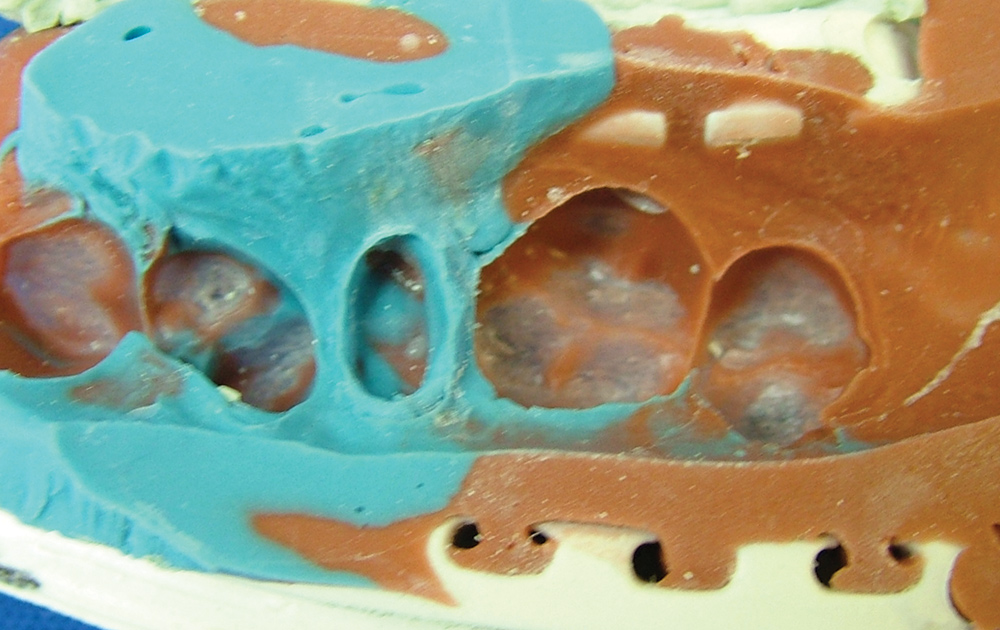
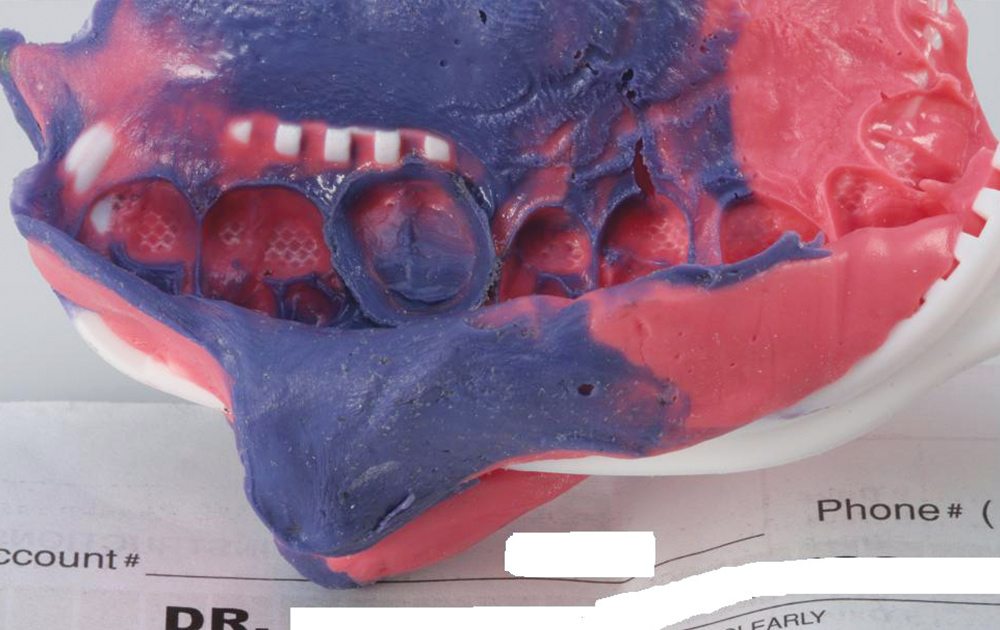
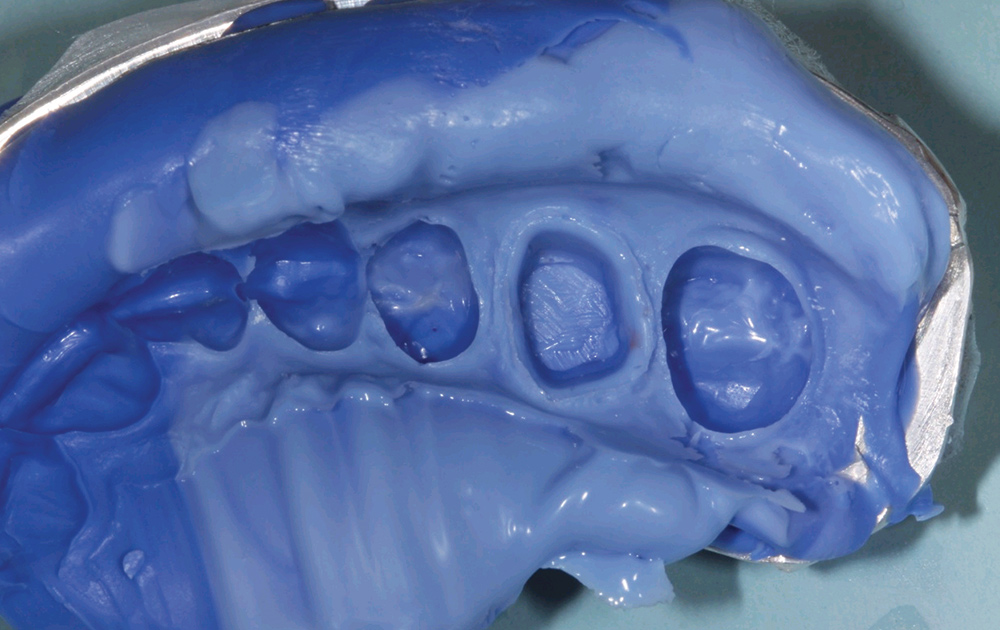
No matter which highly accurate, good flow, stiff, dimensionally stable bite registration material the clinician uses, the untrimmed bite registration will never fit on models derived from alginate (Fig. 6).30 This is due to the inherent mismatch in accuracy of the two materials, as the finely detailed occlusal anatomy picked up by high-flow VPS bite registration materials is not replicated by alginate, thus not allowing the bite registration to seat accurately on the alginate-derived stone model (Figs. 7, 8). If the clinician decides to continue using alginate impressions to generate opposing models, a lateral closed-bite registration is a better choice (Figs. 9, 10).
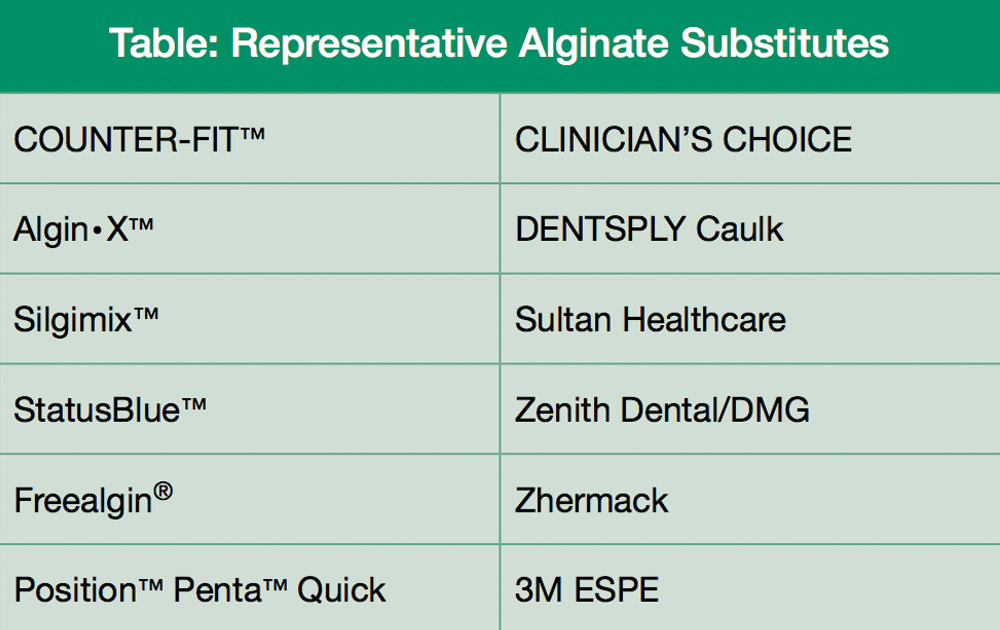
Alginate Substitutes
Alginate substitutes (Table) are essentially low-cost VPS materials that demonstrate all the favorable characteristics previously established for materials of the VPS category. Dr. Gordon Christensen31 has described these alginate substitutes as accurate, clean to use, and with no unpleasant taste or odor (Fig. 11). Furthermore, the addition silicones (VPSs) have been shown to be very accurate and dimensionally stable; stable enough to pour after a delay of time or when making additional pours of the same impression.2,32 Additionally, VPSs have higher tear strength than alginates (an important feature when they are poured multiple times), and are minimally affected by disinfection techniques.33,34 In using a VPS alginate substitute with a VPS bite registration and a working model derived from a VPS impression, mismatches that occur when using casts derived from alginate impressions can be eliminated (Fig. 12). This ensures the casts will be mounted by the dental technician in maximum intercuspation (Fig. 13), which reduces the incidence of high occlusion in the final prosthesis and thus minimizes or eliminates the time required for occlusal adjustments. An added side benefit is that, rather than having to pour up the opposing alginate impression in the dental office, this alginate substitute VPS can be shipped along with the impression of the prepared teeth and bite registration to the dental laboratory. Thus, the time and cost incurred for pouring up the impression in the dental office is removed. This opposing cast fabrication becomes part of the laboratory fee, which more than compensates for the increased cost of taking the impression with an alginate substitute.
No matter which highly accurate, good flow, stiff, dimensionally stable bite registration material the clinician uses, the untrimmed bite registration will never fit on models derived from alginate.
Dual-Arch Impressions
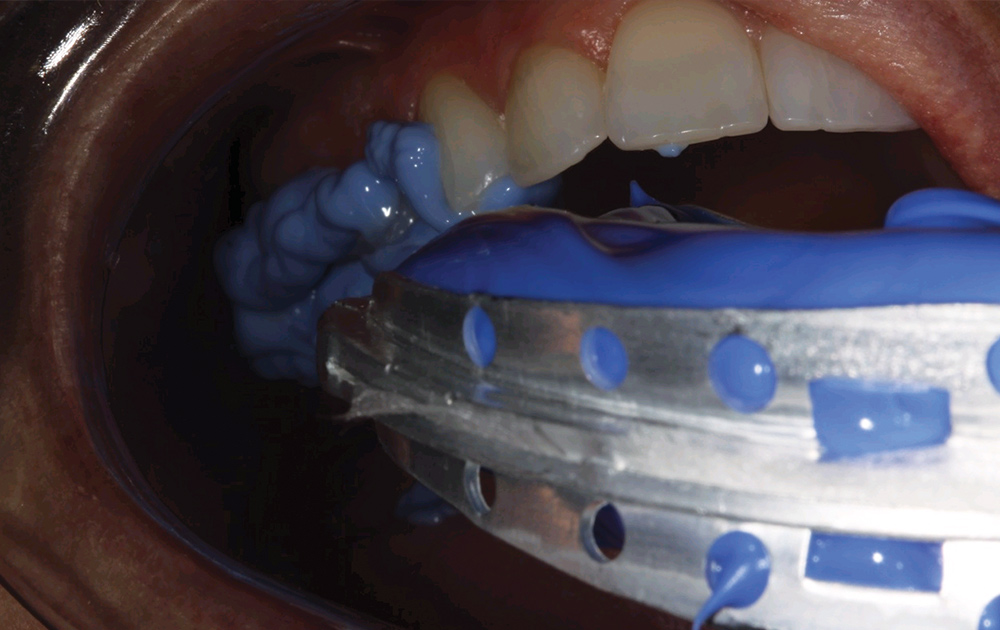
It should now be abundantly clear why properly fabricated dual-arch impressions “produce mounted casts with significantly more accurate maximal intercuspal relationships than mounted casts from full-arch impressions.”4 The dual-arch impression, as an all-in-one technique, is faster, uses less impression material, and is easier for the clinician and the patient.35 However, to be successful with the dual-arch impression tray, there are strict parameters for its use. The rear bar (connector) of the dual-arch tray must comfortably pass through the interocclusal retromolar area with no interference to proper closure. With the dual-arch technique, the prepared teeth should be bordered by intact teeth with centric stops (Fig. 14).36 Single-tooth preparations that fit this criteria are indicated, but multiple tooth preparations may be problematic.1,37 Because the articulators used for mounting dual-arch impressions are simple hinges (usually flexible plastic), the patient must have a cuspid rise (canine guidance) disclusion, not group function. Therefore, the canine tooth must be registered in the impression.5 This is facilitated by full-quadrant metal trays (such as the QUAD-TRAY® XL [Clinician’s Choice]) (Fig. 15). Plastic trays can flex, resulting in a distorted impression. Flexure occurs due to the hydraulic pressures of the impression material, tray side walls impinging on hard tissue (Figs. 16, 17), axial roll or vertical flex of the plastic side walls, the action of swallowing by the patient during impression-taking, and elastic rebound upon removal of the impression.38-40 The dual-arch tray must be rigid,41 making metal trays the tray material of choice. In addition, a complementary rigid (stiff) impression material will increase the chance of overall success with this technique (Fig. 18).36,38 The ADA, in its review of elastomeric impression materials, recommended an impression material with a strain in compression (stiffness) of less than 2%42 be used for the dual-arch impression technique. Nine of the 10 heavy body impression materials tested in this review did not meet this criterion; only Correct Plus® (Pentron Clinical Technologies; Wallingford, Conn.) was found to have a strain in compression of 1.5%. Another VPS material on the market, AFFINITY InFlex (Clinician’s Choice), is also especially well suited for the dual-arch impression technique and has a strain in compression of 1.3% (Fig. 19).
It should now be abundantly clear why properly fabricated dual-arch impressions “produce mounted casts with significantly more accurate maximal intercuspal relationships than mounted casts from full-arch impressions.
Conclusion
For predictability in mounting or articulating models, it is prudent to use materials of matching accuracy so that the components work in harmony. To ensure clinical success, use a high-flow, stiff (no bounce) bite registration material; remove soft-tissue interferences; use an alginate substitute for a high-quality opposing model resulting in better interdigitation of all of the components; or use an all-in-one dual-arch impression using a metal tray and technique-specific impression material.
The recommendations presented in this article will help the clinician in reducing occlusal adjustments on final crown & bridge prostheses, thus saving time and reducing stress at the delivery appointment.
Dr. Boksman is director of clinical affairs for Clinical Research Dental/Clinician’s Choice. He is also an adjunct clinical professor at the Schulich School of Medicine and Dentistry and maintains a private practice in London, Ontario, Canada. Contact him at lboksman@clinicalresearchdental.com.
Reprinted by permission of Dentistry Today, ©2011 Dentistry Today.
References
- Donovan TE, Chee WW. A review of contemporary impression materials and techniques. Dent Clin North Am. 2004 Apr;48(2):vi-vii, 445-70.
- Boksman L. Eliminating the variables in impression taking. Ont Dent. 2005;34:22-5.
- Christensen GJ. Making fixed prostheses that are not too high. J Am Dent Assoc. 2006 Jan;137(1):96-8.
- Parker MH, Cameron SM, Hughbanks JC, Reid DE. Comparison of occlusal contacts in maximum intercuspation for two impression techniques. J Prosthet Dent. 1997 Sep;78(3):255-9.
- Christensen GJ. Ensuring accuracy and predictability with double-arch impressions. J Am Dent Assoc. 2008 Aug;139(8):1123-5.
- Millstein PL, Clark RE. Determination of the accuracy of laminated wax interocclusal wafers. J Prosthet Dent. 1983 Sep;50(3):327-31.
- Lassila V. Comparison of five interocclusal recording materials. J Prosthet Dent. 1986 Feb;55(2):215-8.
- Anselm Wiskott HW, Nicholls JI. Fixed prosthodontics centric relation registration technique using resin copings. Int J Prosthodont. 1989 Sep-Oct;2(5):447-52.
- Urstein M, Fitzig S, Moskona D, Cardash HS. A clinical evaluation of materials used in registering interjaw relationships. J Prosthet Dent. 1991 Mar;65(3):372-7.
- Tripodakis AP, Vergos VK, Tsoutsos AG. Evaluation of the accuracy of interocclusal records in relation to two recording techniques. J Prosthet Dent. 1997 Feb;77(2):141-6.
- Lassila V, McCabe JF. Properties of interocclusal registration materials. J Prosthet Dent. 1985 Jan;53(1):100-4.
- Breeding LC, Dixon DL. Compression resistance of four interocclusal recording materials. J Prosthet Dent. 1992 Dec;68(6):876-8.
- Chun JH, Pae A, Kim SH. Polymerization shrinkage strain of interocclusal recording materials. Dent Mater. 2009 Jan;25(1):115-20.
- Millstein PL, Hsu CC. Differential accuracy of elastomeric recording materials and associated weight change. J Prosthet Dent. 1994 Apr;71(4):400-3.
- Boksman L, Tousignant G. Alginate substitutes: rationale for their use. Dent Today. 2009;28:104-5.
- Nichols PV. An investigation of the dimensional stability of dental alginates [dissertation]. Sydney, Australia: Faculty of Dentistry, University of Sydney; 2006. Available at: http://hdl.handle.net/2123/1270. Accessed Oct. 22, 2010.
- Taylor RL, Wright PS, Maryan C. Disinfection procedures: their effect on the dimensional accuracy and surface quality of irreversible hydrocolloid impression materials and gypsum casts. Dent Mater. 2002 Mar;18(2):103-10.
- Jagger DC, Al Jabra O, Harrison A, et al. The effect of a range of disinfectants on the dimensional accuracy of some impression materials. Eur J Prosthodont Restor Dent. 2004 Dec;12(4):154-60.
- Machado C, Johnston W, Coste A, et al. Simulated clinical compatibility of disinfectant solutions with alginate impression materials. Presented at: IADR General Session & Exhibition; July 1, 2006; Brisbane, Australia. Abstract 2467.
- Muller-Bolla M, Lupi-Pégurier L, Velly AM, Bolla M. A survey of disinfection of irreversible hydrocolloid and silicone impressions in European Union dental schools: epidemiologic study. Int J Prosthodont. 2004 Mar-Apr;17(2):165-71.
- Lu JX, Zhang FM, Chen YM, Qian M. The effect of disinfection on dimension stability of impressions [in Chinese]. Shanghai Kou Qiang Yi Xue. 2004 Aug;13(4):290-2.
- Frey G, Lu H, Powers J. Effect of mixing methods on mechanical properties of alginate impression materials. J Prosthodont. 2005 Dec;14(4):221-5.
- Perry R. Using polyvinyl impressions for study models: a case report. Dent Today. 2004 Oct;23(10):106-7.
- Chen SY, Liang WM, Chen FN. Factors affecting the accuracy of elastomeric impression materials. J Dent. 2004 Nov;32(8):603-9.
- Bayindir F, Yaniko lu N, Duymu Z. Thermal and pH changes, and dimensional stability in irreversible hydrocolloid impression material during setting. Dent Mater J. 2002;21:200-9.
- Mendez AJ. The influence of impression trays on the accuracy of stone casts poured from irreversible hydrocolloid impressions. J Prosthet Dent. 1985 Sep;54(3):383-8.
- Gordon GE, Johnson GH, Drennon DG. The effect of tray selection on the accuracy of elastomeric impression materials. J Prosthet Dent. 1990 Jan;63(1):12-5.
- Leung KC, Chow TW, Woo EC, Clark RK. Effect of adhesive drying time on the bond strength of irreversible hydrocolloid to stainless steel. J Prosthet Dent. 1999 May;81(5):586-90.
- Smith SJ, McCord JF, Macfarlane TV. Factors that affect the adhesion of two irreversible hydrocolloid materials to two custom tray materials. J Prosthet Dent. 2002 Oct;88(4):423-30.
- .Boksman L. Point of care: how do I minimize the amount of occlusal adjustment necessary for a crown? J Can Dent Assoc. 2005;71:494-5.
- Christensen GJ. Ask Dr. Christensen. Dental Economics. 2008;98:66.
- Karthikeyan K, Annapurni H. Comparative evaluation of dimensional stability of three types of interocclusal recording materials: an in vitro study. J Indian Prosthodont Soc. 2007;7(1):24-7.
- Waranowicz MT, O’Keefe KL. Alginates and alginate substitutes. The Dental Advisor. 2007;24 (special issue).
- Christensen G. Impression material disinfection: is it necessary? Clinician’s Report. Feb 2010:3, 4.
- Lane DA, Randall RC, Lane NS, Wilson NH. A clinical trial to compare double-arch and complete-arch impression techniques in the provision of indirect restorations. J Prosthet Dent. 2003 Feb;89(2):141-5.
- Kaplowitz GJ. Trouble-shooting dual-arch impressions. J Am Dent Assoc. 1996;127:234-40.
- Davis RD, Schwartz RS. Dual-arch and custom tray impression accuracy. Am J Dent. 1991;4:89-92.
- Boksman L. Clinical predictability with dual-arch impressions: plastic trays are not the answer. Dentaltown. 2009;10:18-21.
- Larson TD, Nielsen MA, Brackett WW. The accuracy of dual-arch impressions: a pilot study. J Prosthet Dent. 2002 Jun;87(6):625-7.
- Cox JR, Brandt RL, Hughes HJ. A clinical pilot study of the dimensional accuracy of double-arch and complete-arch impressions. J Prosthet Dent. 2002 May;87(5):510-5.
- Wilson EG, Werrin SR. Double arch impressions for simplified restorative dentistry. J Prosthet Dent. 1983 Feb;49(2):198-202.
- Elastomeric impression materials. ADA Product Review. 2007;2:9-14.