Clinical Predictability Using Fiber Posts
The restoration of endodontically treated teeth is often compromised by the minimal amount of residual tooth structure remaining to support and retain the final restoration. This may be due to endodontic overinstrumentation and flaring of the root canal during endodontic therapy, or to extensive structural defects from previous restorations, or the deleterious effects of the carious process.1 Many of these teeth require the placement of a post-and-core restoration for retention, whether the tooth is restored directly or indirectly with full or partial coverage. The dental literature supports the fact that a circumferential ferrule in combination with an endodontic post results in better long-term clinical success for crowned, endodontically treated teeth.2-4 However, many of these studies looked at cemented posts, while different ferrule designs have little, if any, influence on the fracture resistance of teeth with fiber posts, with no significant change in the resistance of teeth with fiber posts regardless of which ferrule design is incorporated. This unique property of these types of posts is an additional advantage in clinical practice.5
The gold standard for many years was the cast gold post-and-core; however, “given the scientific literature that has appeared, the creation of a conventional cast post/post core, even if passively cemented, is useless.”6 Goto et al., when looking at crown retention, have shown that fiber-reinforced dowels (posts) and bonded composite cores under fatigue loading provided significantly stronger crown retention than cast gold dowels and titanium alloy dowels with composite cores.7 A four-year clinical study comparing fiber posts and traditional cast posts showed that the cast post group had root fractures in 9% of the sample, while fiber posts had no root fractures.8 In a literature review by Heydecke, it has been shown that cast post-and-cores do not have a better performance than direct post-and-core restorations.9 Therefore, it seems that the current use of cast post-and-cores is difficult to justify.
The use of metallic posts for retention has been studied extensively. Stiff metallic posts work against the natural function of the tooth, creating zones of tension and shear, both in the dentin and at the interfaces of the luting cement and post.10 For teeth restored with stainless steel posts, a significantly lower load resulted in failure, as compared with those teeth restored with glass-fiber posts.11 There is a worse mechanical performance in teeth restored using stainless steel posts, with a high stress concentration due to the significant difference between the elastic moduli of the steel and surrounding materials.11,12 The use of fiber posts is preferable to titanium posts as well, with teeth restored with fiber posts exhibiting a significantly higher resistance to fracture than with titanium posts.13 In both static and fatigue fracture testing under vertical or oblique loadings, the fracture loads of the teeth restored with fiber posts were significantly greater than those of teeth restored with metallic posts.14 The more rigid metallic post can transfer more stress to the root than fiber posts, which increases the probability of vertical root fracture.15 Because fiber-reinforced posts have an elastic modulus that more closely approaches that of dentin,16 fiber posts produce less stress on the root dentin around the post tip than do metal posts.17 The nonmetallic posts comply more satisfactorily with the requirements necessary to provide a mechanical behavior more similar to that of the dental structure, the compatibility among the mechanical properties found in these systems and the dentin providing a biometric behavior, reducing the risk of failure or fracture of the root.18 If fracture does occur, fracture with metal posts is usually catastrophic, while fracture of teeth restored with fiber posts show fractures that would allow repeated repair.19 In a literature search looking at 1,984 abstracts on the failure modes of post systems, Fokkinga et al. concluded that the fiber-reinforced post system more frequently showed favorable failure modes compared to metal posts.20
Many metallic posts are parallel, which can require the removal of significant amounts of root dentin in the apical half, while not adapting well to the coronal aspect of the root structure. In contrast, an anatomical fiber post requires minimal tooth structure removal during canal reshaping, and allows for greater post-to-canal adaptation in the apical and coronal half of the canal, with an esthetic nature. This provides a favorable foundation for eliminating discoloration caused by a metallic post placed under all-ceramic crown systems.21
Because fiber-reinforced posts have an elastic modulus that more closely approaches that of dentin, fiber posts produce less stress on the root dentin around the post tip than do metal posts.
As an added clinical benefit, fiber posts can have twice the fatigue resistance of ceramic or metal posts.22 Statistically, as well, resin-supported polyethylene fiber and glass-fiber dowels show the lowest coronal leakage when compared with stainless steel and zirconia dowels at all time periods.23-25
Not all fiber posts are created equal. In a study by Seefeld et al., looking at eight types of fiber posts, the fracture load of the tested systems ranged from 60 to 96 N and the flexural strength from 565 to 898 MPa. The differences in fiber diameter ranged from 8.2 to 21 µm and the fiber:matrix ratio from 41% to 76%.26 These fiber posts can be: zirconia enriched, glass fiber, quartz fiber, glass fiber-zirconia enriched, and glass fiber and carbon fiber,27 with quartz fiber posts recording significantly higher failure loads.19 They can be translucent, white, dentin or color-changing translucent,27 and for light transmission they can be excellent, good, fair or poor.28 Posts with a high translucency facilitate excellent esthetic results, eliminating show-through and discoloration while allowing transmission of light polymerization energy.29 Fiber posts can be tapered, double-tapered, parallel, parallel with a tapered end, parallel-tapered and serrated,27 with the double-tapered post closely imitating the post-endodontic shape of a radicular canal, leaving a thin and uniform thickness of cement at the post/canal interface. This improved adaptation of the post promotes the mechanical properties of the quartz fiber/epoxy material, instead of the weaker composite resin cement.30 The quality, type and volume of fibers, the way the fibers are silanated, and the type of resin used affects the clinical performance of these fiber posts, with some failing in cyclic fatigue to fracture in a few cycles and others in over two million cycles (DT Double Taper Light-Post radiopaque [RTD]).31
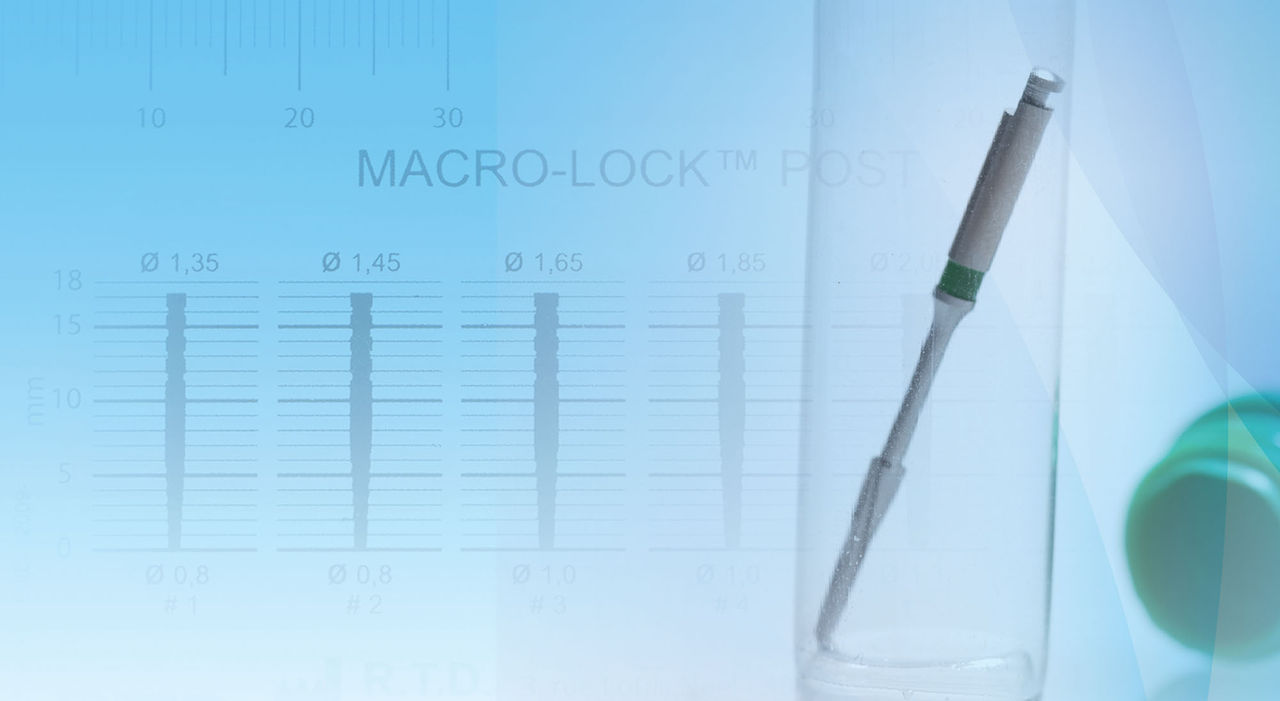
A new addition to the RTD family of fiber posts is the Macro-Lock Illusion post, which is fabricated with a high-percentage loading (80% vol) of pretensed long continuous translucent unidirectional quartz fibers with epoxy resin, and is radiopaque. Quartz crystal is the world’s purest form of silica. It is homogeneous and non-porous,32 and has an interface treatment of the fibers to achieve a perfect match between the thousands of fibers and the organic resin matrix. Color-changing technology allows for the post to disappear when seated at oral temperature and for it to be visible under water spray if retrieval is ever necessary. The Macro-Lock Illusion post has high translucency for good light transmission, an elastic modulus as low as 13 GPa (depending on the angle), and a flexural strength of 1600 MPa. It is unique in that it allows for micro and macro retention of the bonded core. A recent study by Dallari et al. showed that the Macro-Lock post with its macro retention reached one of the highest results when testing the retention of quartz fiber posts.33 No surface treatment of the post (etch, silane, sandblasting) is necessary before cementation.
Case Presentation
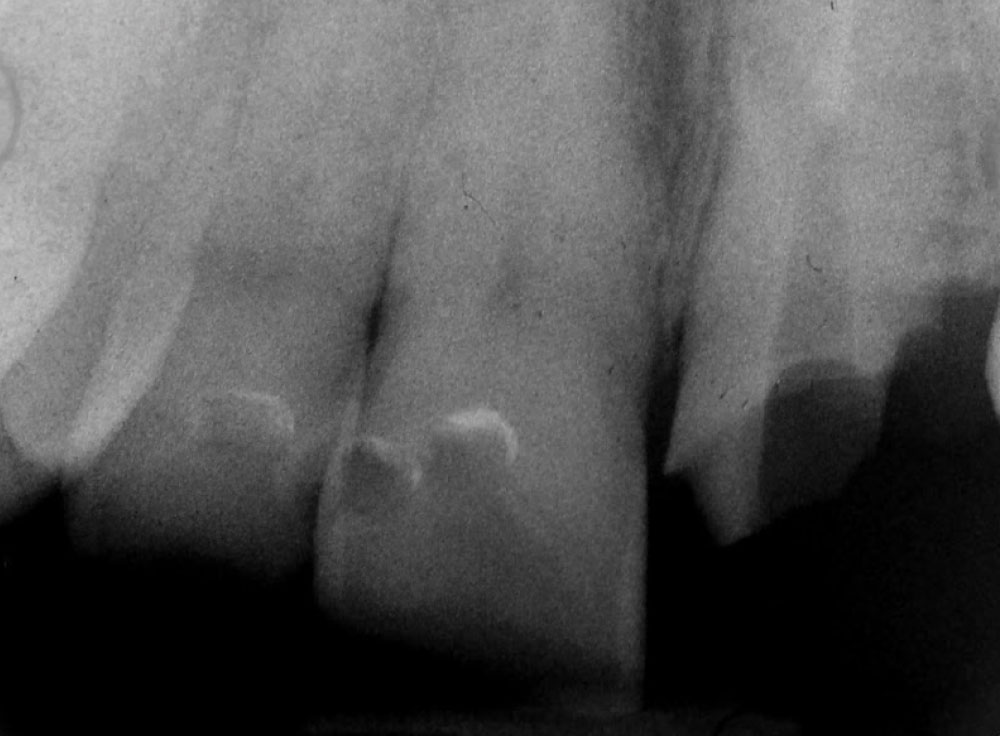
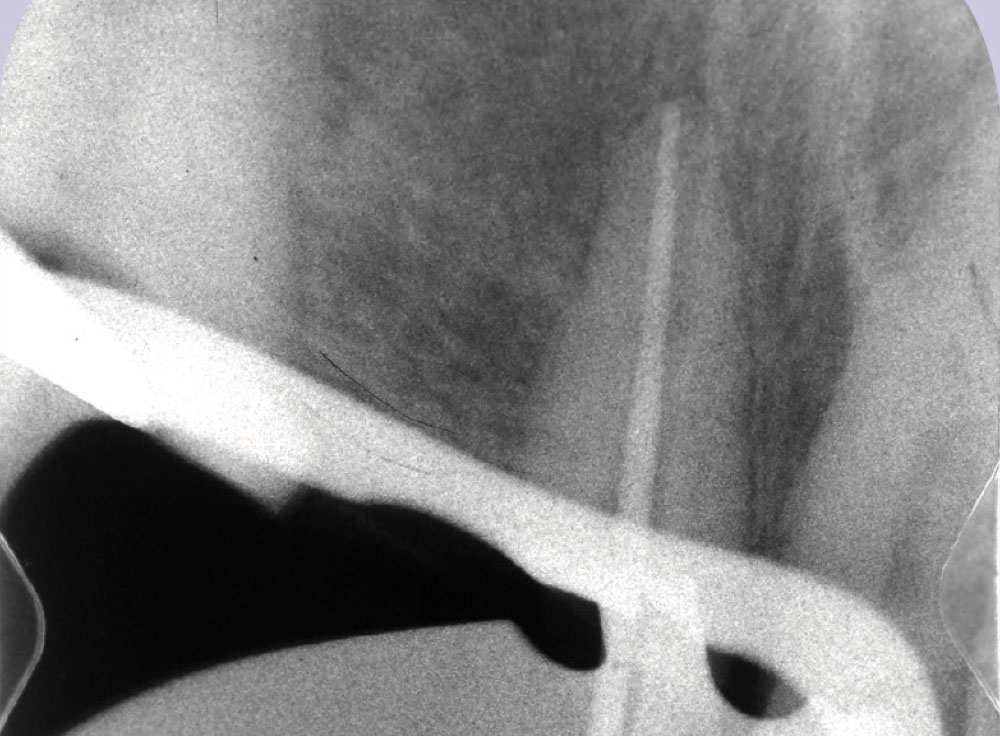
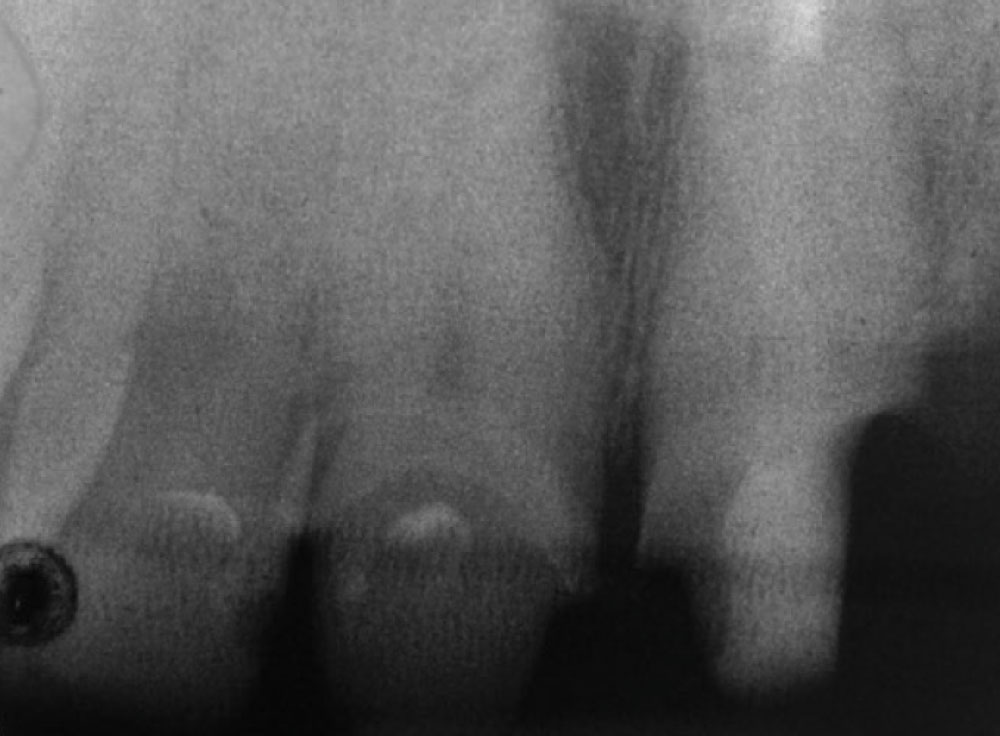
A patient presented to the office with a failed bridge from tooth #9 to tooth #11. The patient was advised that #11 was unrestorable and that one treatment plan option was to place a new 5-unit bridge from #8–12 with double abutments on the anteriors. The preoperative radiograph (Fig. 1) shows a short endodontic filling requiring retreatment, prior to placement of a post-and-core.
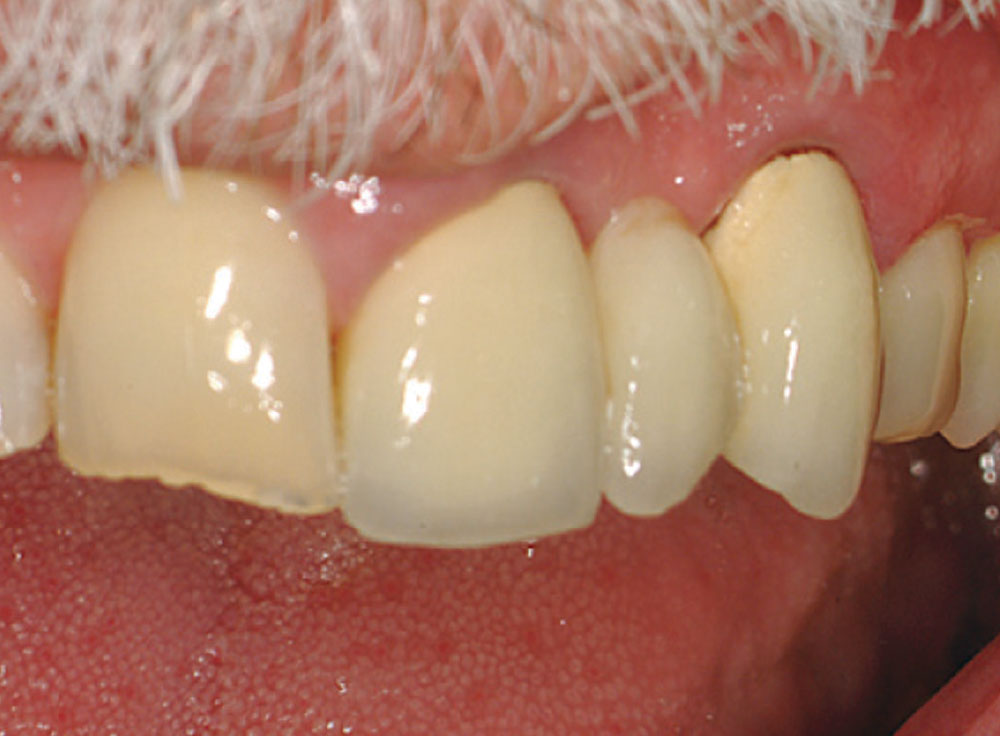
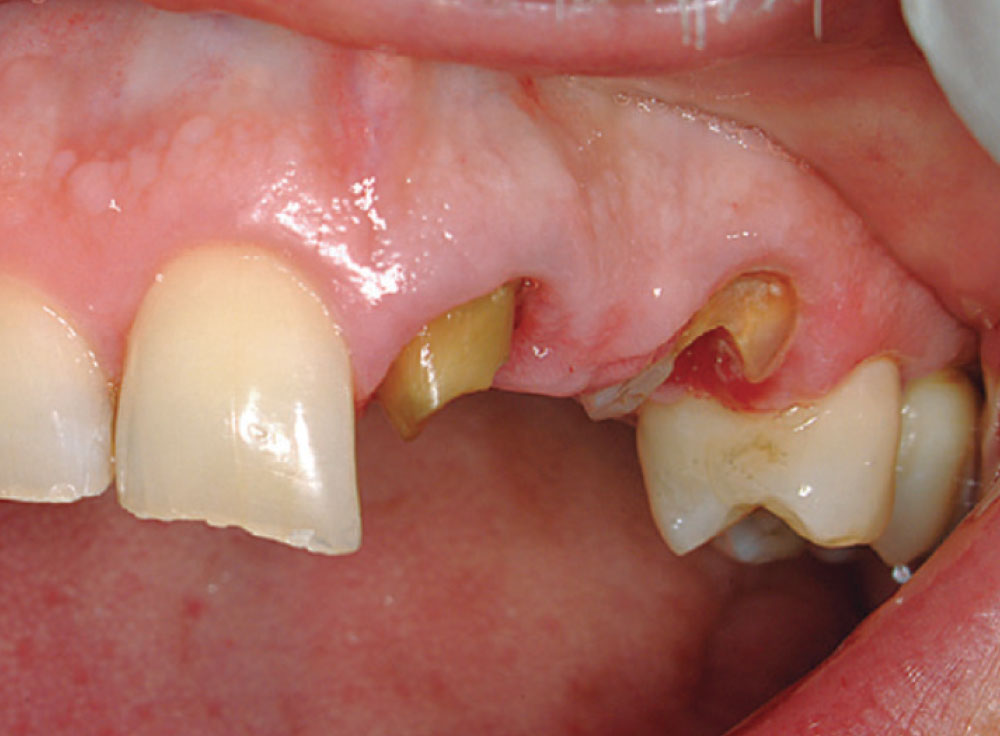
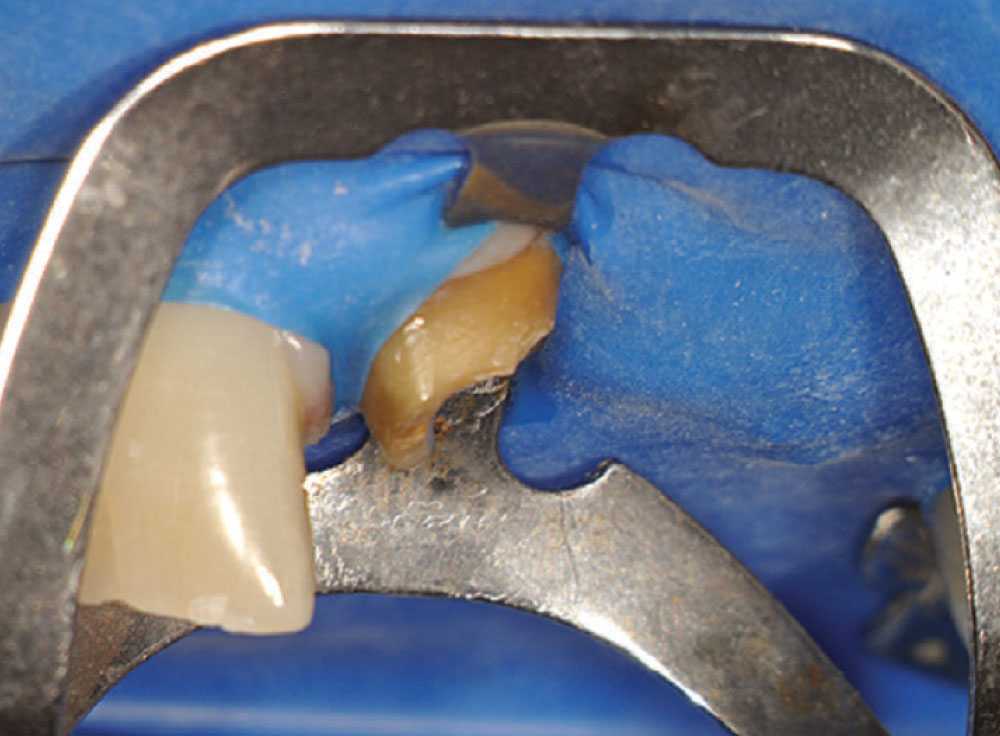
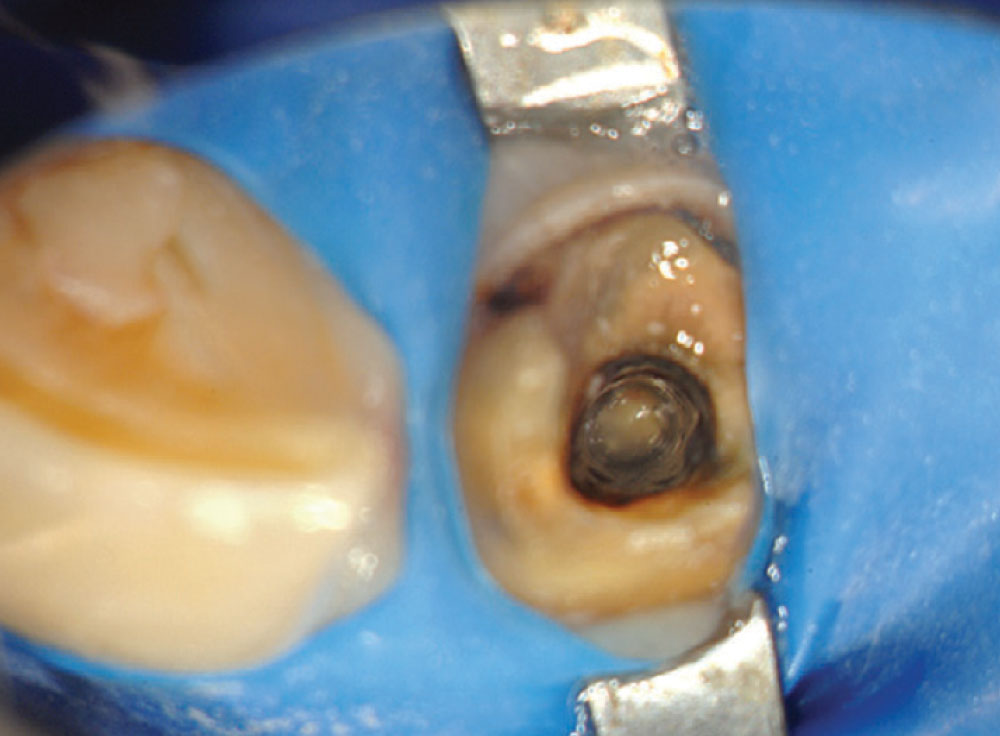
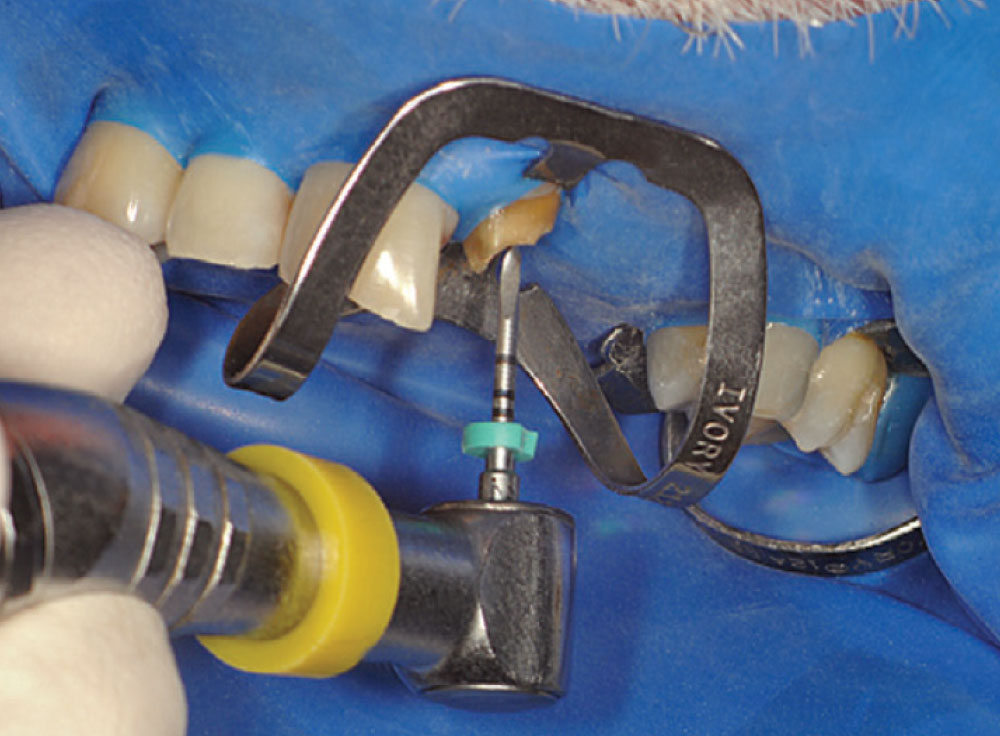
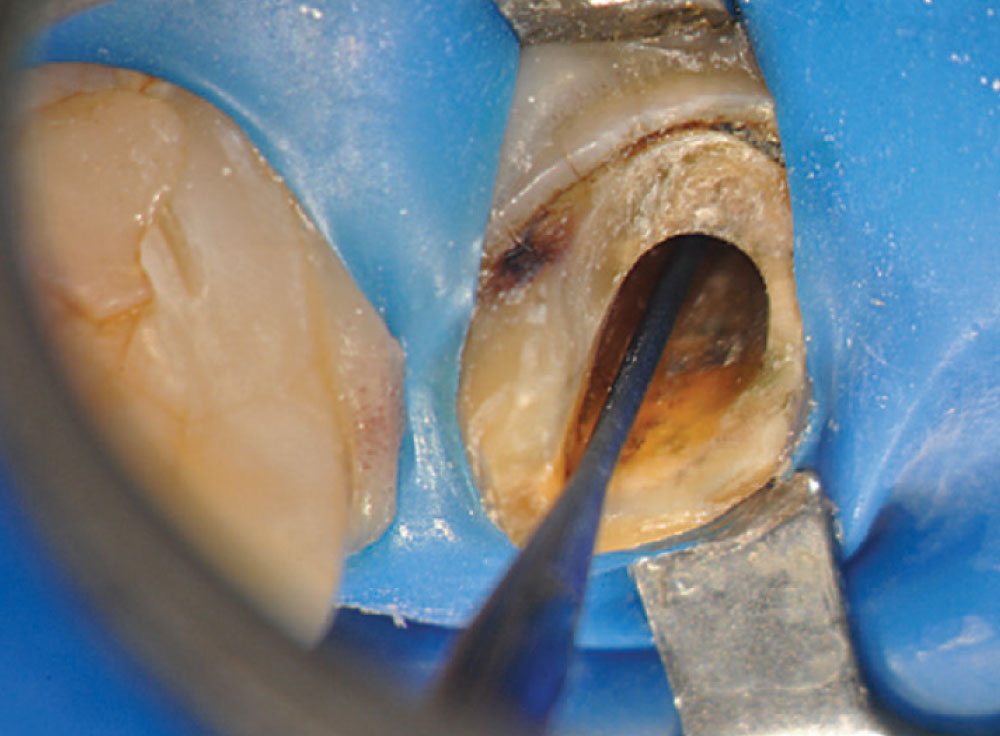
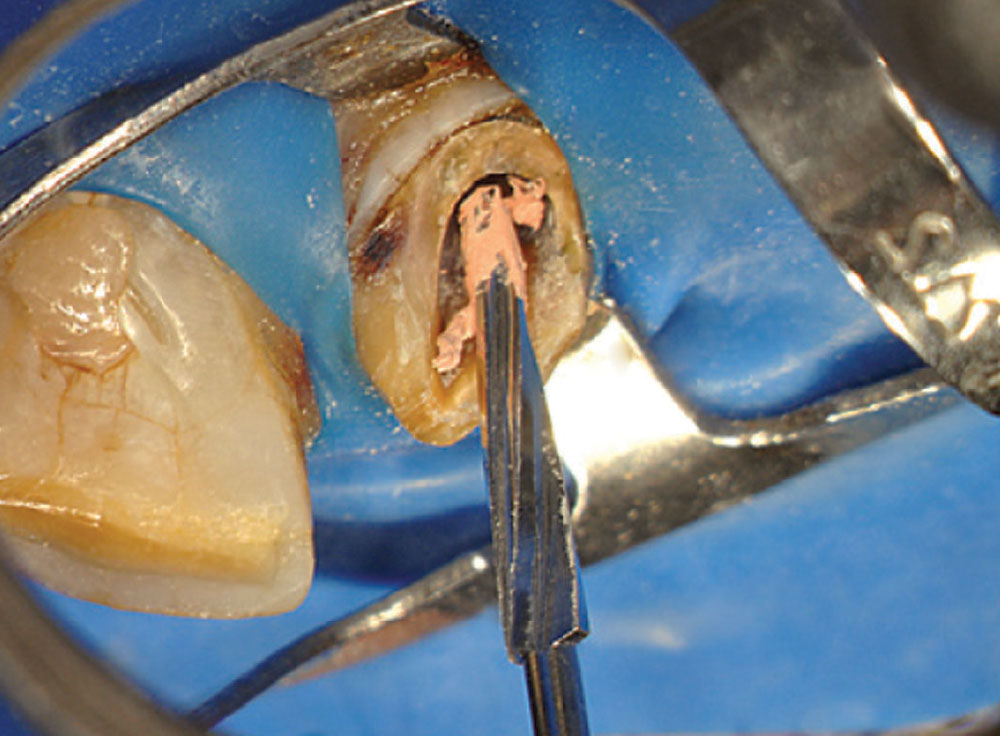
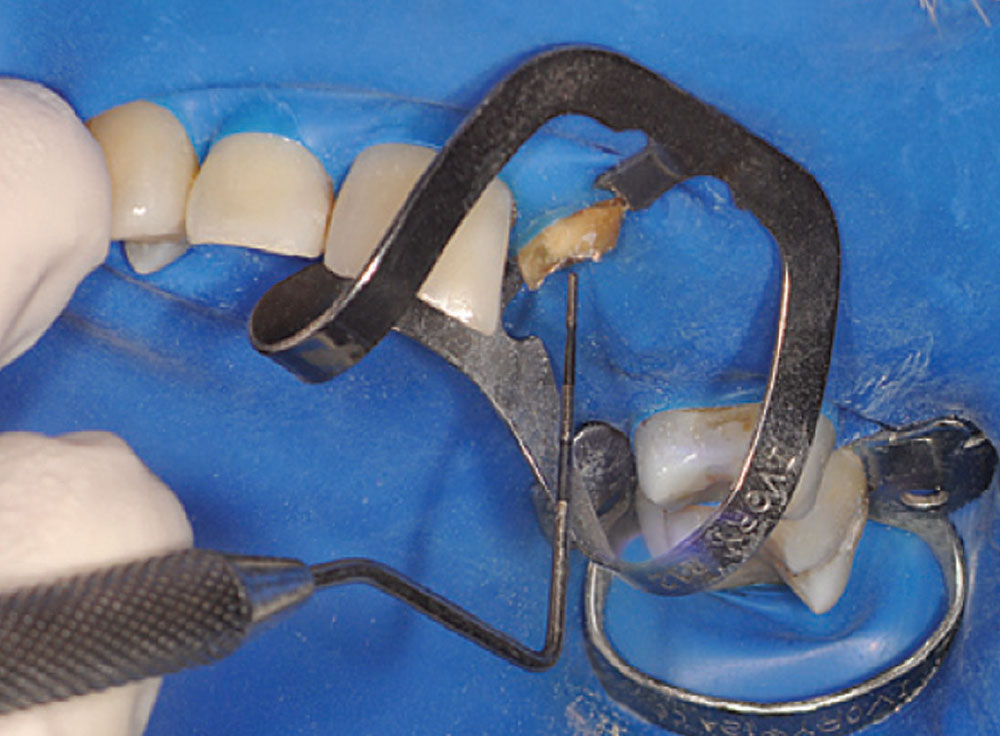
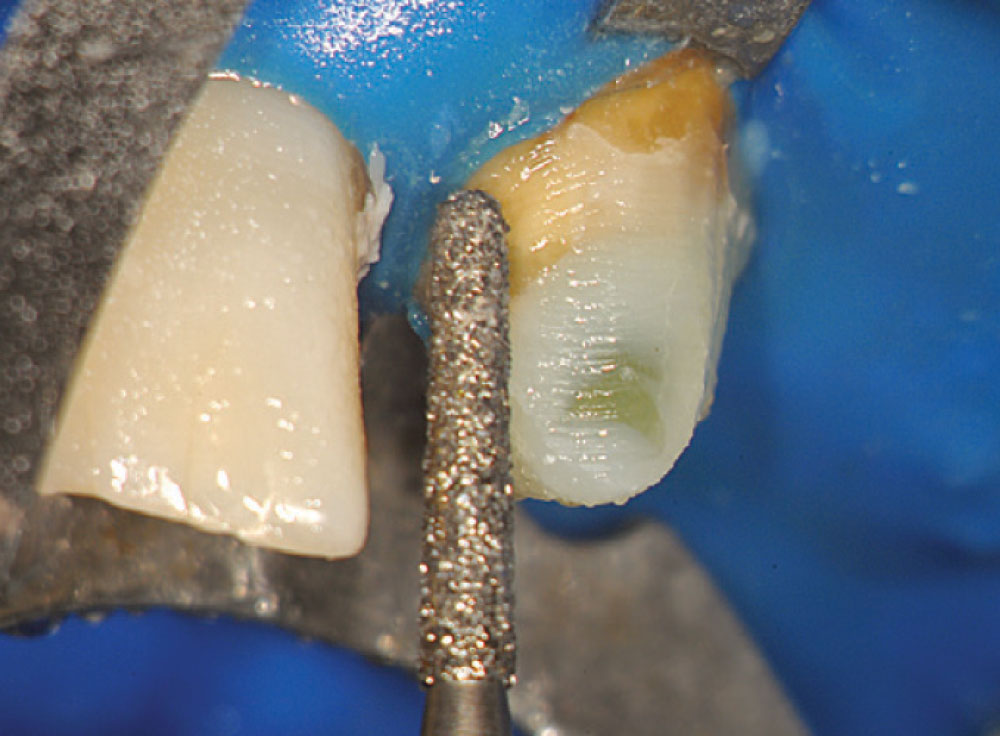
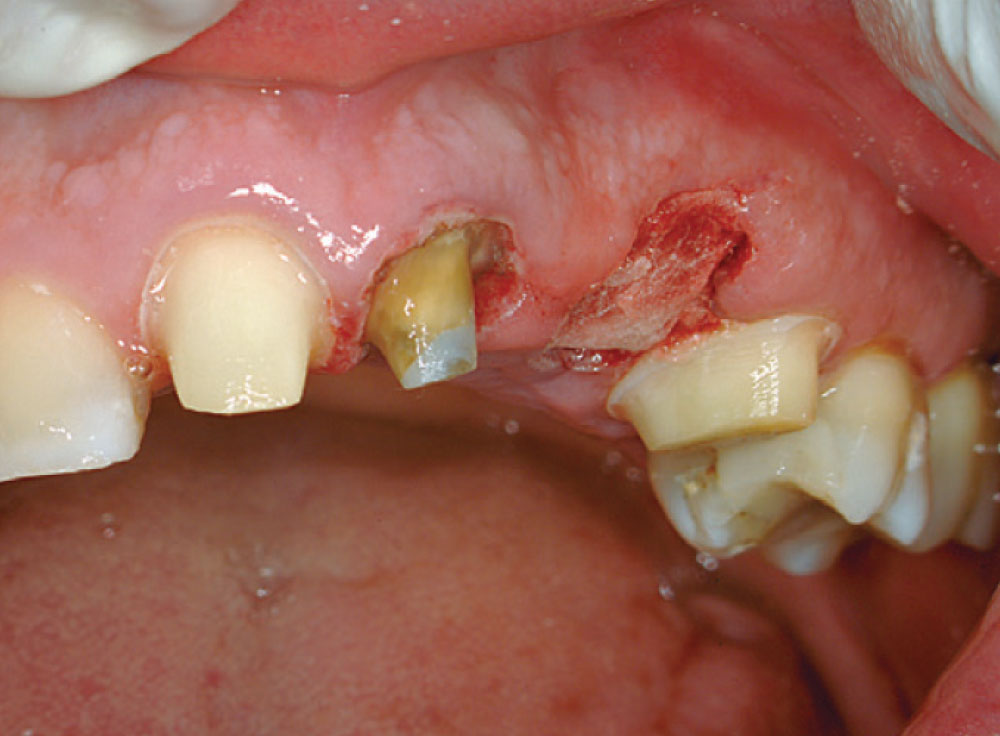
Access was difficult to negotiate at the canal terminus. The use of ultrasonic tips eventually removed the calcification deep into the canal at the apex and the tooth was re-treated endodontically. Figure 2 shows the preoperative photograph of the loose bridge before removal. At removal of the bridge (Fig. 3), it was confirmed that #11 was unrestorable, necessitating its extraction and the preparation of #12. Figure 4 shows the rubber dam application on tooth #9, with the occlusal view of the access into the canal in Figure 5. Twisted rotary endo files were used to remove the gutta-percha (Fig. 6), and ultrasonic tips were used to open the apical part of the canal (Fig. 7).
As an added clinical benefit, fiber posts can have twice the fatigue resistance of ceramic or metal posts. Statistically … resin-supported polyethylene fiber and glass-fiber dowels show the lowest coronal leakage when compared with stainless steel and zirconia dowels at all time periods.
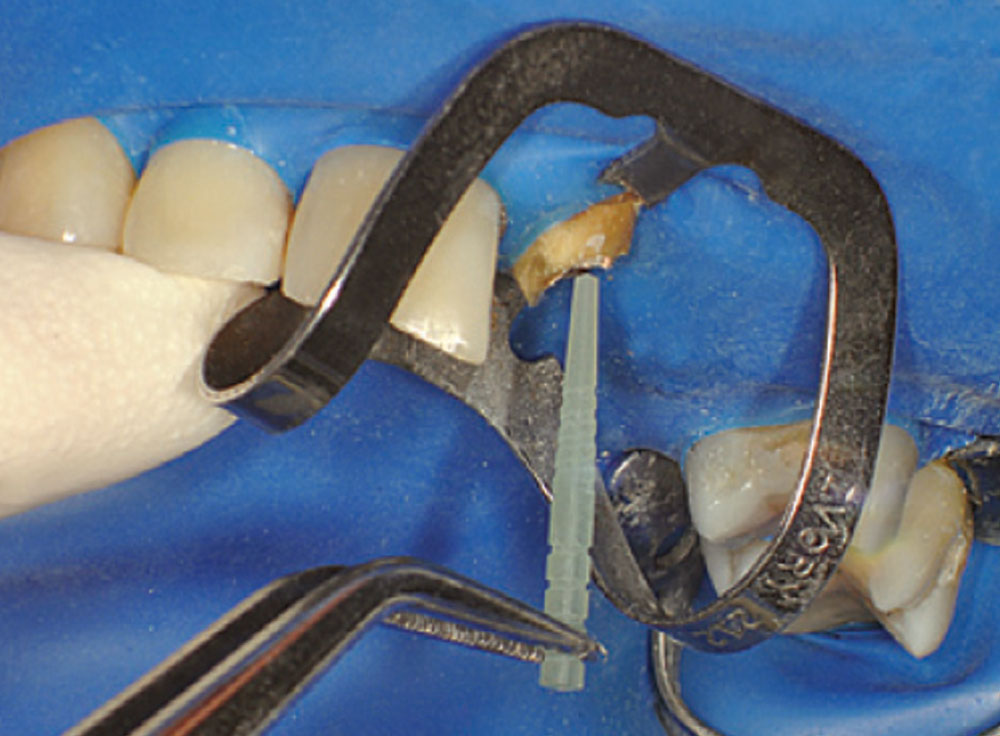
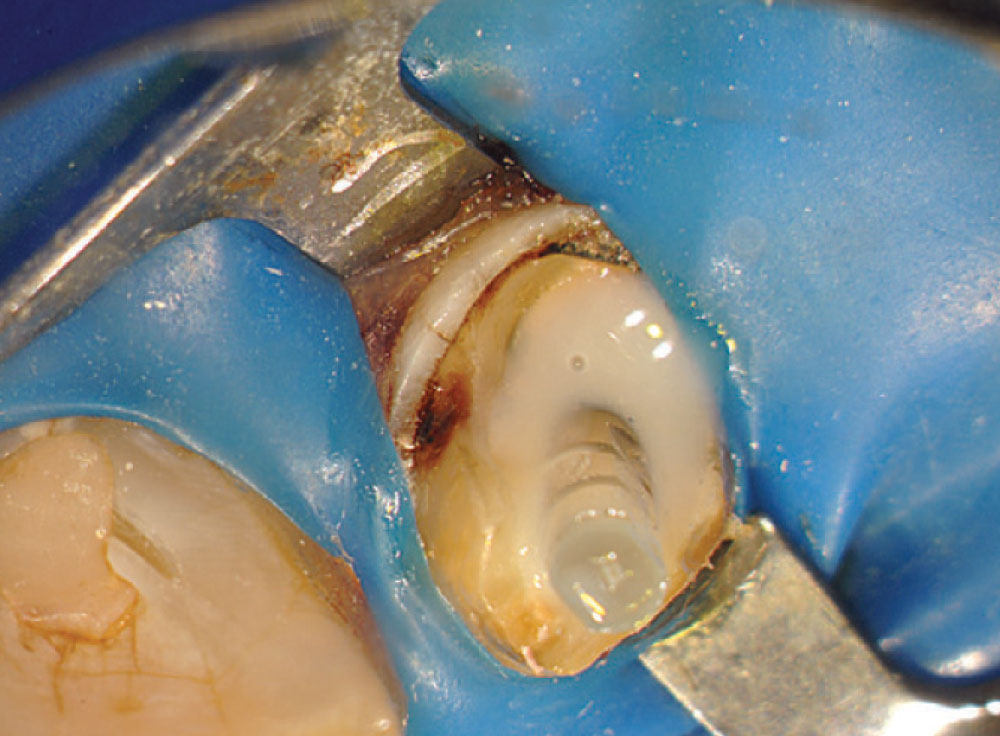
The trial cone was inserted and verified with a trial cone radiograph (Fig. 8). A warm vertical downpack was achieved with the System B™ (SybronEndo; Orange, Calif.) and the canal was backfilled with the Obtura II (Obtura Spartan; Algonquin, Ill.). The green Macro-Lock Illusion post drill #4 (RTD) (Clinical Research Dental; London, Ontario, Canada) was used to create the post space (Fig. 9). The post space depth was measured at 15 mm on a 19 mm root (Fig. 10). The post was inserted to verify fit and position (Fig. 11).
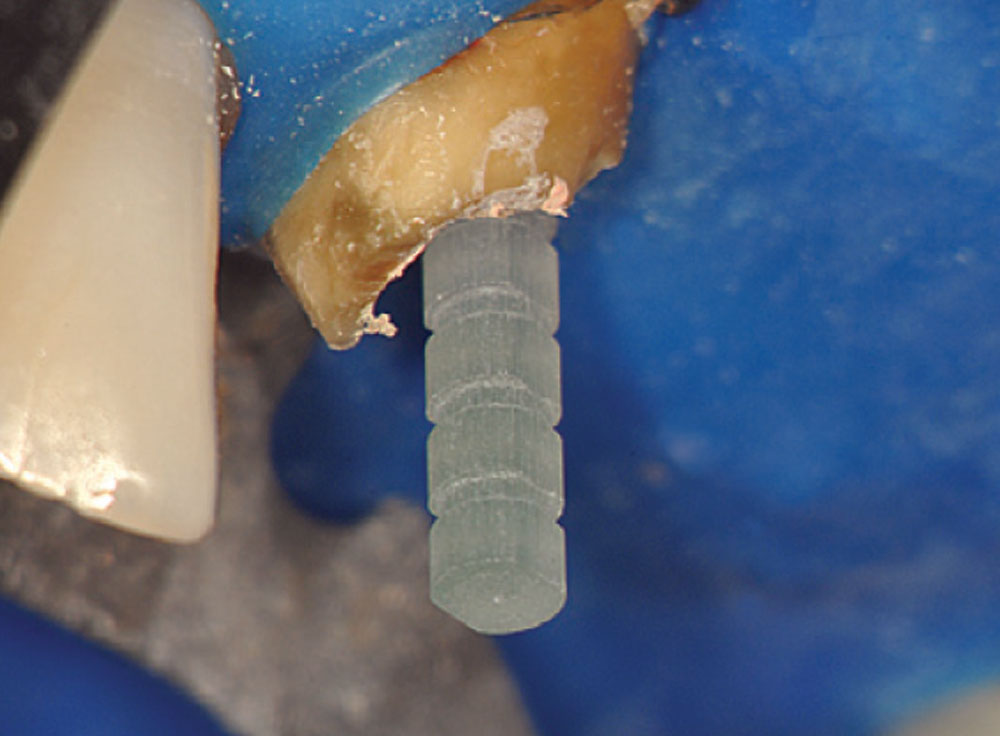
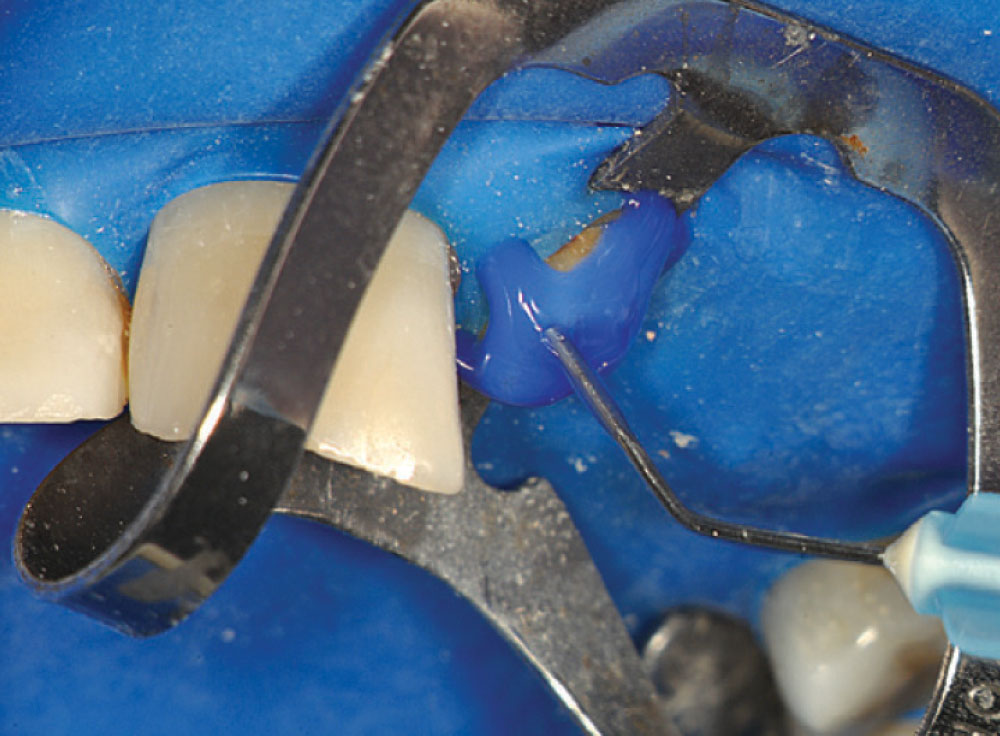
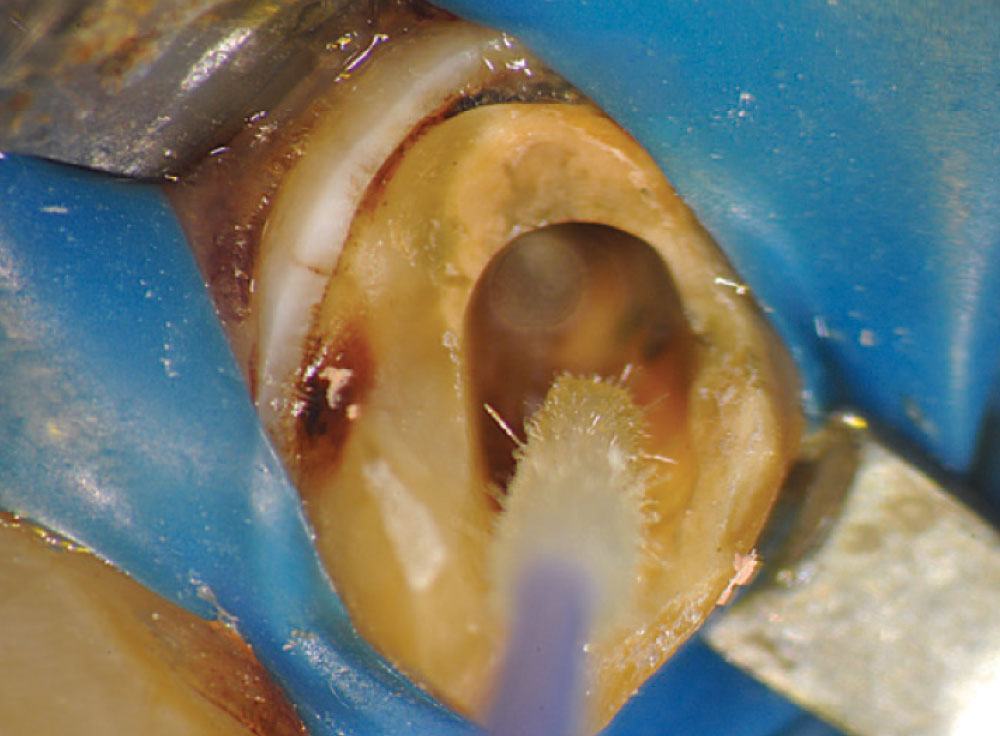
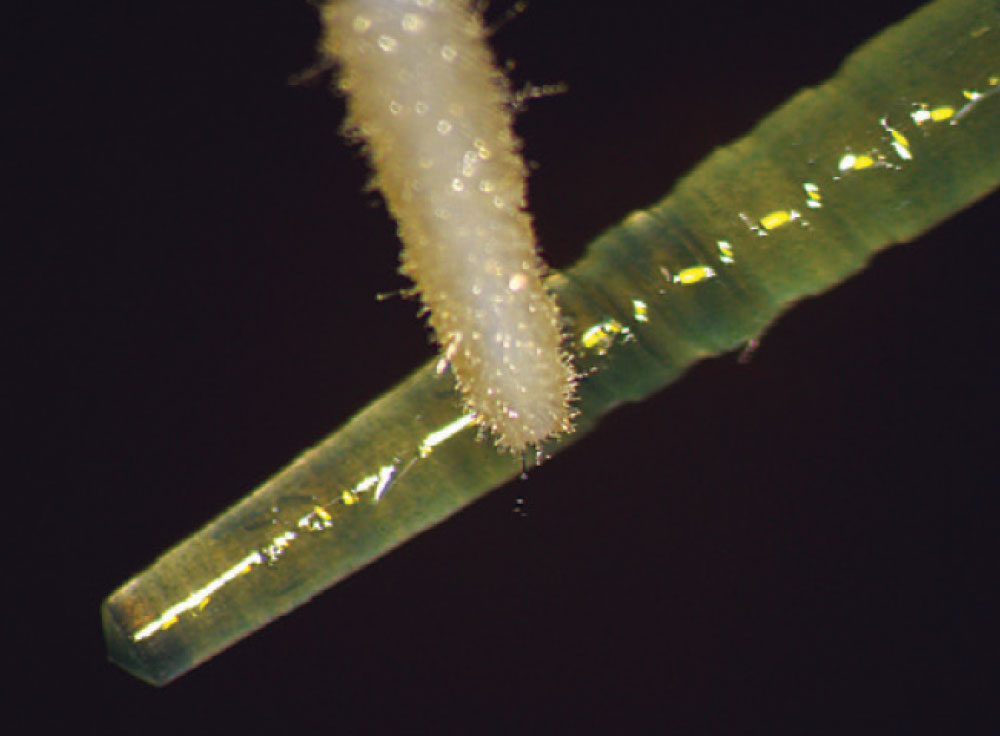
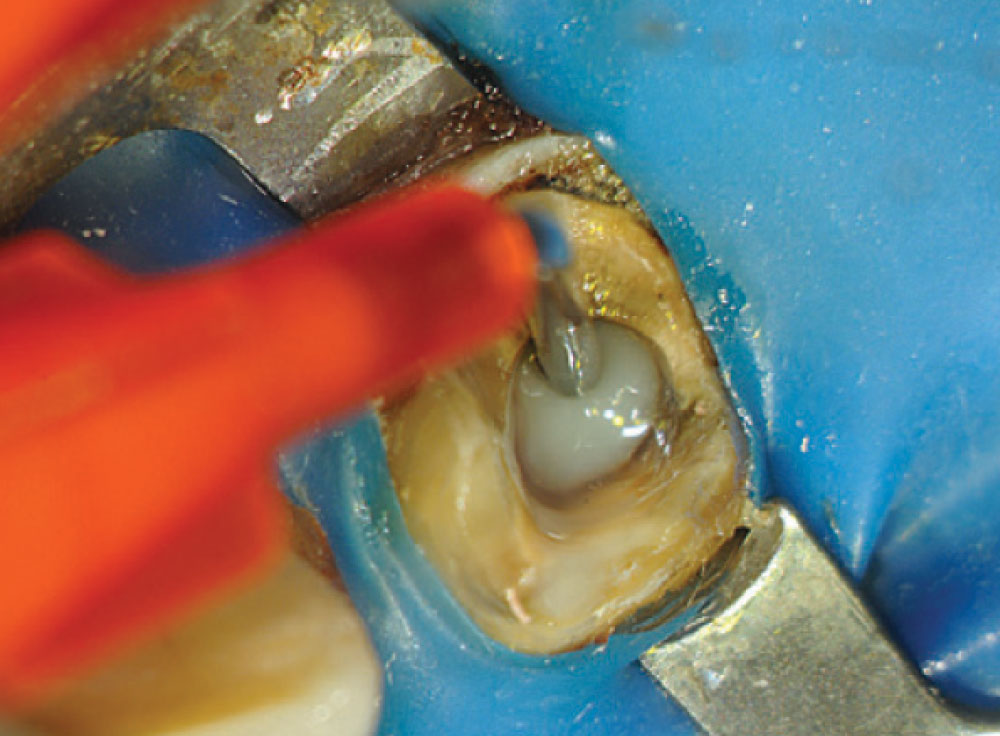
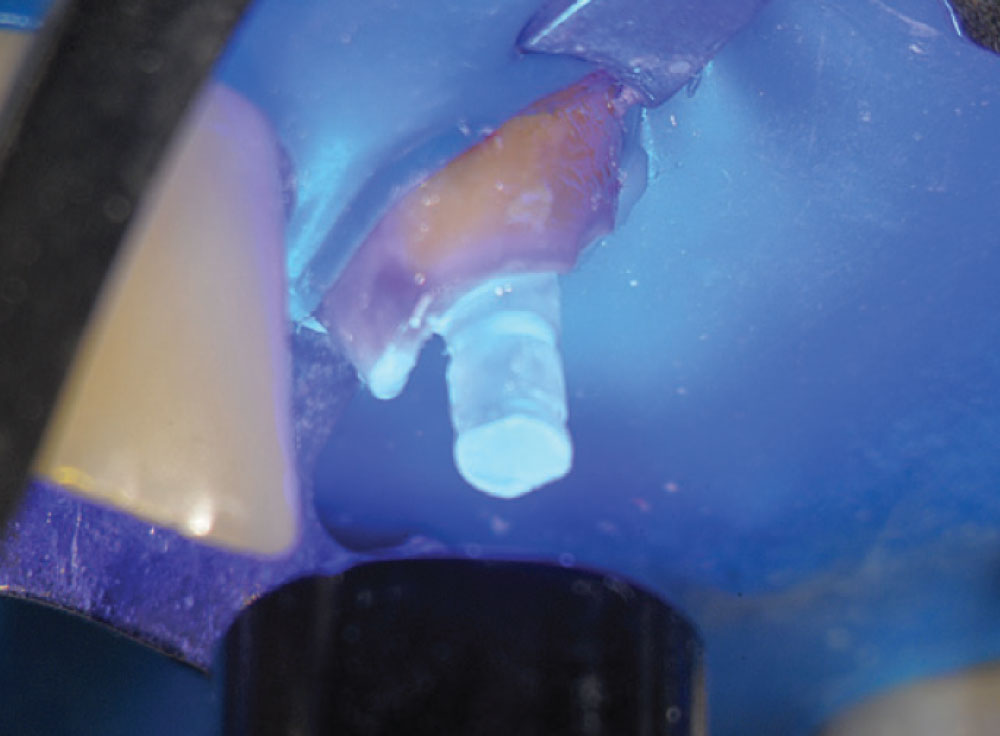
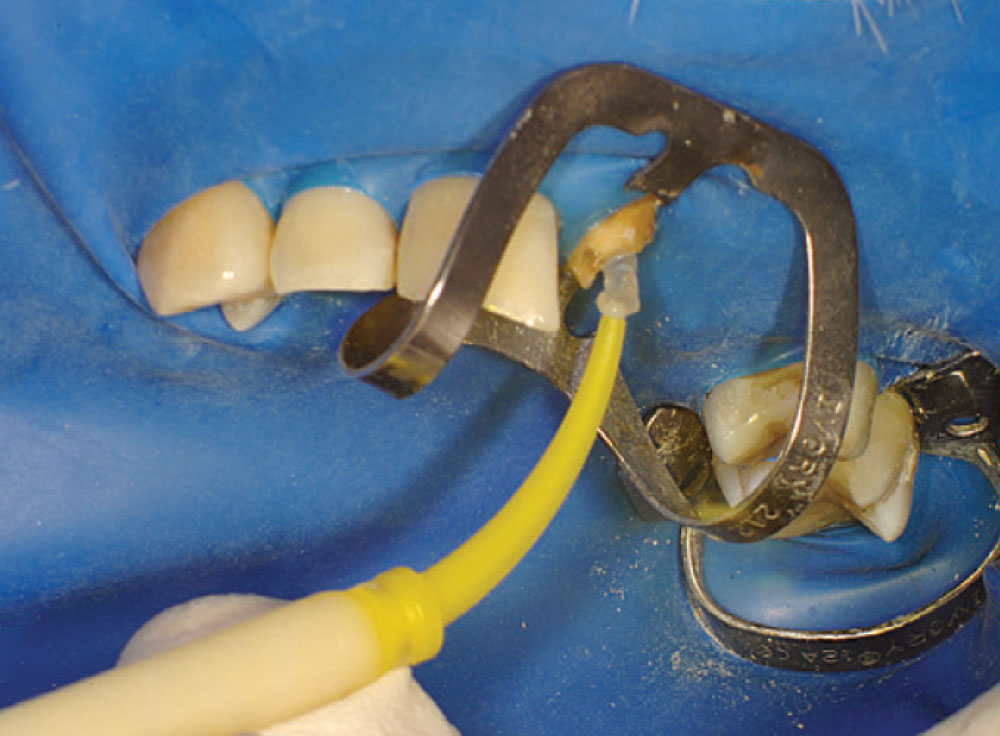
Figure 12 shows a magnified view of the Macro-Lock Illusion post seated in the canal. The post was trimmed with a diamond disc (Fig. 13). The post space was etched with Ultra-Etch® (Ultradent; South Jordan, Utah) for 15 seconds using an Endo-Eze™ tip (Ultradent) (Fig. 14) to reach the apex of the post preparation and inject from the apex to the incisal, so as not to entrap any air. The post space was thoroughly rinsed and a purple Capillary tip (Ultradent) was used to lightly dry the canal. A light-cure adhesive, proven to be compatible with dual-cure cements, was applied to the canal with a tapered brush long enough to reach the bottom of the post space (Fig. 15), and at the same time the light-cure adhesive was placed on the Macro-Lock Illusion post (Fig. 16).
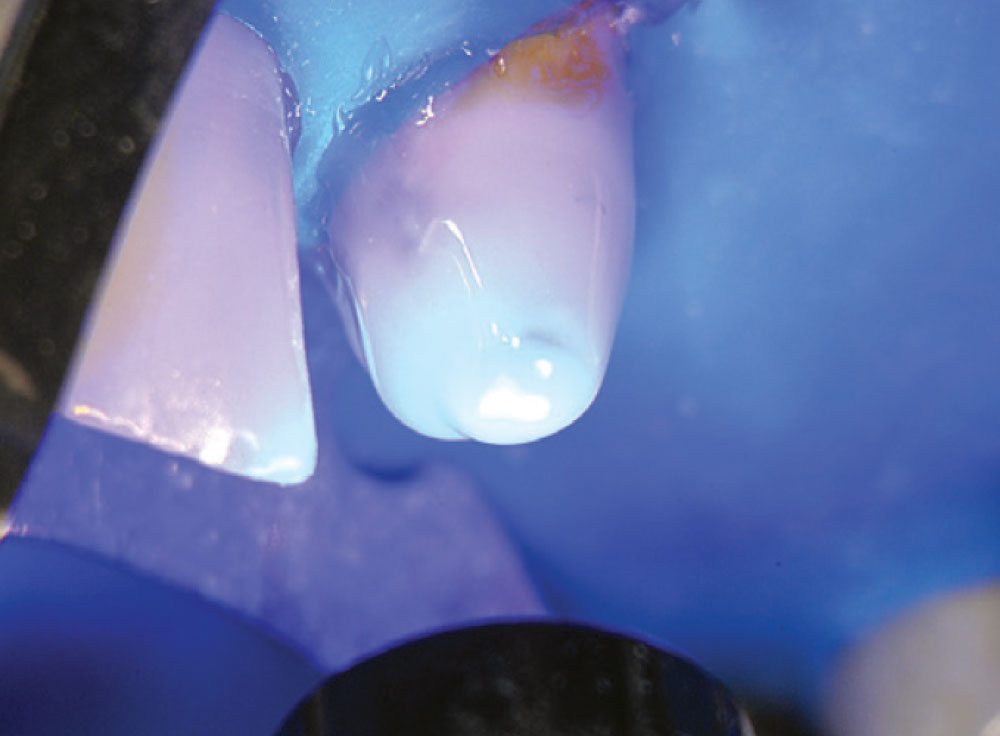
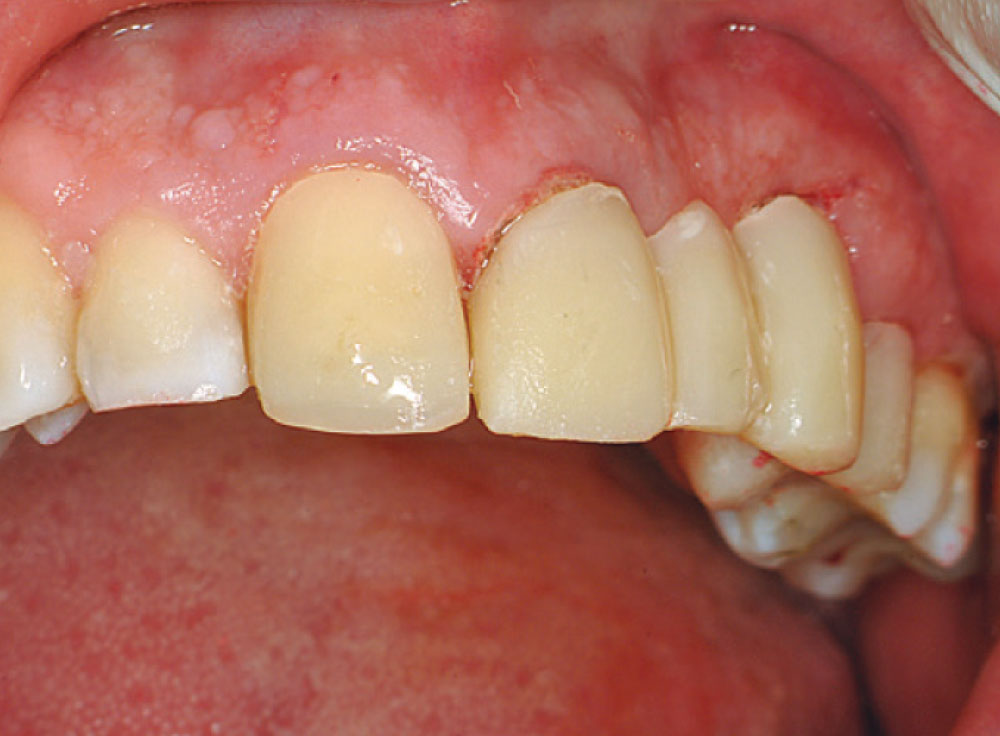
The solvent was evaporated with a light airflow and the bond cured in the post hole and the post (Fig. 17). A dual-cure resin cement was injected into the canal space from the bottom up (Fig. 18), and the post was seated into the dual-cure cement (Fig. 19). After curing the cement (Fig. 20), CosmeCore™ (Cosmedent, Inc.; Chicago, Ill.) was used to create the core buildup (Fig. 21), followed by a cure of 20 seconds (Fig. 22). CosmeCore can be used as the dual-cure cement and the core buildup simultaneously. Figure 23 shows preparation of the CosmeCore/Macro-Lock Illusion post-and-core for full coverage (note the color of the post when exposed to cold water). Teeth #8 and #12 were prepared and tooth #11 extracted (Fig. 24). A provisional bridge was fabricated using Temptation® (Clinical Research Dental) and cemented with Cling2 Temporary Cement (Clinical Research Dental) (Fig. 25). A final postoperative radiograph (Fig. 26) shows the opacity of the Macro-Lock Illusion post.
Dr. Boksman is director of clinical affairs for Clinical Research Dental/Clinician’s Choice. He maintains a private practice in London, Ontario, Canada. Contact him at lboksman@clinicalresearchdental.com.
Dr. van As has lectured and published on lasers and the dental-operating microscope in practice. He maintains a private practice in North Vancouver, British Columbia. Contact him at glennvanas@mac.com.
References
- ^ Kishen A. Mechanisms and risk factors for fracture predilection in endodontically treated teeth. Endodontic Topics. 2006;13(1):57-83.
- ^ Sorensen JA, Engleman MJ. Ferrule design and fracture resistance of endodontically treated teeth. J Prosthetic Dent. 1990 May;63(5):529-36.
- ^ Naumann M, Preuss A, Frankenberger R. Reinforcement effect of adhesively luted fiber reinforced composite versus titanium posts. Dent Mater. 2007 Feb;23(2):138-44.
- ^ Ferrari M, Cagidiaco MC, Grandini S, De Sanctis M, Goracci C. Post placement affects survival of endodontically treated premolars. J Dent Res. 2007 Aug;86(8):729-34.
- ^ Dikbas I, Tanalp J, Ozel E, Koksal T, Ersoy M. Evaluation of the effect of different ferrule designs on the fracture resistance of endodontically treated maxillary central incisors incorporating fiber posts, composite cores and crown restorations. J Contemp Dent Prac. 2007 Nov 1;8(7):62-9.
- ^ Scotti R, Malferrari S. Prosthetic aspects of endodontically treated tooth restoration – proceedings from the 5th International Symposium. 2001:27-33.
- ^ Goto Y, Nicholls JI, Phillips KM, Junge T. Fatigue resistance of endodontically treated teeth restored with three dowel-and-core systems. J Prosthet Dent. 2005 Jan;93(1):45-50.
- ^ Ferrari M, Vichi A, García-Godoy F. Clinical evaluation of fiber-reinforced epoxy resin posts and cast post and cores. Am J Dent. 2000 May;13(Spec No):15B-18B.
- ^ Heydecke G, Peters MC. The restoration of endodontically treated, single-rooted teeth with cast or direct posts and cores: a systematic review. J Prosthet Dent. 2002 Apr;87(4):380-6.
- ^ Lanza A, Aversa R, Rengo S, Apicella D, Apicella A. 3D FEA of cemented steel, glass and carbon posts in a maxillary incisor. Dent Mater. 2005 Aug;21(8):709-15.
- ^ Barjau-Escribano A, Sancho-Bru JL, Forner-Navarro L, Rodríguez-Cervantes PJ, Pérez-Gónzález A, Sánchez-Marín FT. Influence of prefabricated post material on restored teeth: fracture strength and stress distribution. Oper Dent. 2006 Jan-Feb;31(1):47-54.
- ^ de Castro Albuquerque R, Polleto LT, Fontana RH, Cimini CA. Stress analysis of an upper central incisor restored with different posts. J Oral Rehabil. 2003 Sep;30(9):936-43.
- ^ Aminsalehi E. Strength of incisors restored by metallic, fiber and ceramic posts. J Dent Res. 2005;84 (Spec Issue B), African and Middle East section (dentalresearch.org).
- ^ Hayashi M, Sugeta A, Takahashi Y, Imazato S, Ebisu S. Static and fatigue fracture resistance of pulpless teeth restored with post-cores. Dent Mater. 2008 Sep;24(9):1178-86.
- ^ Sidoli GE, King PA, Setchell DJ. An in vitro evaluation of a carbon fiber-based post and core system. J Prosthet Dent. 1997 Jul;78(1):5-9.
- ^ Plotino G, Grande NM, Bedini R, Pameijer H, Somma F. Flexural properties of endodontic posts and human root dentin. Dent Mater. 2007 Sep;23(9):1129-35.
- ^ Nakamura T, Ohyama T, Waki T, Kinuta S, Wakabayashi K, Mutobe Y, Takano N, Yatani H. Stress analysis of endodontically treated anterior teeth restored with different types of post material. Dent Mater J. 2006 Mar;25(1):145-50.
- ^ Oliviera LCA, Candido MSM, Duarte S, Oliviera SAG. Comparative study of stress distribution in upper incisors; biometri behavior of post systems. 2003. AADR Abstract #0548 (dentalresearch.org).
- ^ Akkayan B, Gü̈lmez T. Resistance to fracture of endodontically treated teeth restored with different post systems. J Prosthet Dent. 2002 Apr;87(4):431-7.
- ^ Fokkinga WA, Kreulen CM, Vallittu PK, Creugers NH. A structured analysis of in vitro failure loads and failure modes of fiber, metal, and ceramic post-and-core systems. Int J Prosthodont. 2004 Jul-Aug;17(4):476-82.
- ^ Boudrias P, Sakkal S, Petrova Y. Anatomical post design meets quartz fiber technology: rationale and case report. Compend Contin Educ Dent. 2001 Apr;22(4):337-40, 342.
- ^ Wiskott HW, Meyer M, Perriard J, Scherrer SS. Rotational fatigue-resistance of seven post types anchored on natural teeth. Dent Mater. 2007 Nov;23(11):1412-9.
- ^ Usumez A, Cobankara F, Ozturk N, Eskitascioglu G, Belli S. Microleakage of endodontically treated teeth with different dowel systems. J Prosthet Dent. 2004 Aug;92(2):163-9.
- ^ Bae S, Kim E-J, Chang H-S, Microleakage and fracture aspects of posts treated with repeated loading. J Dent Res. 2006;85 (Special Issue B) Abstract #1516 (dentalresearch.org).
- ^ Jung SH, Min KS, Chang HS, Park SD, Kwon SN, Bae JM. Microleakage and fracture patterns of teeth restored with different posts under dynamic loading. J Prosthet Dent. 2007 Oct;98(4):270-6.
- ^ Seefeld R, Wenz HJ, Ludwig K, Kern M. Resistance to fracture and structural characteristics of different fiber reinforced post systems. Dent Mater. 2007 Mar;23(3):265-71.
- ^ Freedman G, Jain C. Restoration of the endodontically treated tooth – a buyers guide to pins and posts. Dent Today. 2008 Jul:108-21.
- ^ Posts a shift away from metal? CRA Newsletter. 2004 May;28(5):1-3.
- ^ Bassi M. Light diffusion through double taper quartz-epoxy fiber posts. Proceedings from the 5th International Symposium. 2001:21-6.
- ^ Boudrias P, Sakkal S, Petrova Y. Anatomical post design applied to quartz fiber/epoxy technology: a conservative approach. Oral Health. 2001 Nov:9-16.
- ^ Grandini S, Goracci C, Monticelli F, Borracchini A, Ferrari M. An evaluation using a three-point bending test of the fatigue resistance of certain fiber posts. Il Dentista Moderno. 2004 Mar:70-4.
- ^ Glazer B. Endodontic post evolution: from metal to quartz (light post by LTD). Oral Health. 2002 May:402-45.
- ^ Dallari A, Mason P, Rovatti L, Dallari B. Effect of surface treatments on retention of quartz fiber posts. J Dent Res. 2008;87 (Special Issue C) Abstract #383.
Reprinted by permission of Oral Health, November 2008.