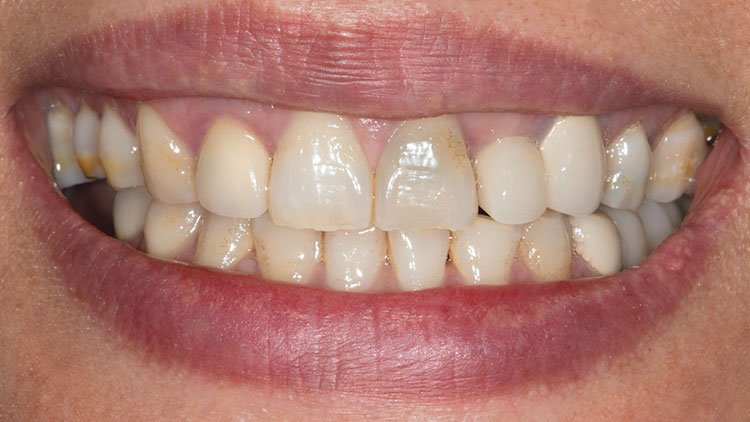
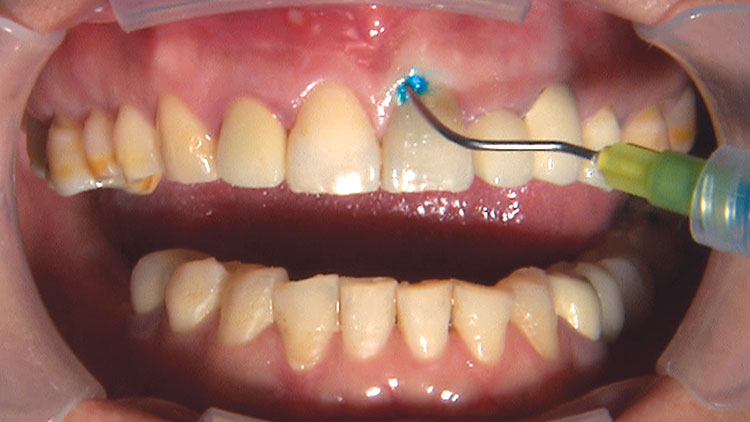
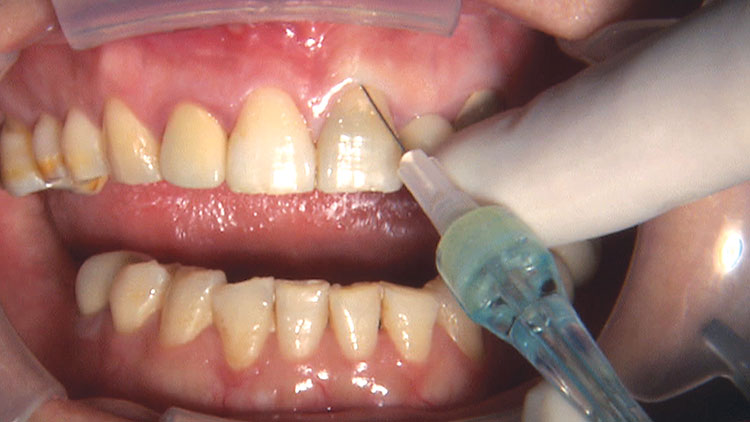
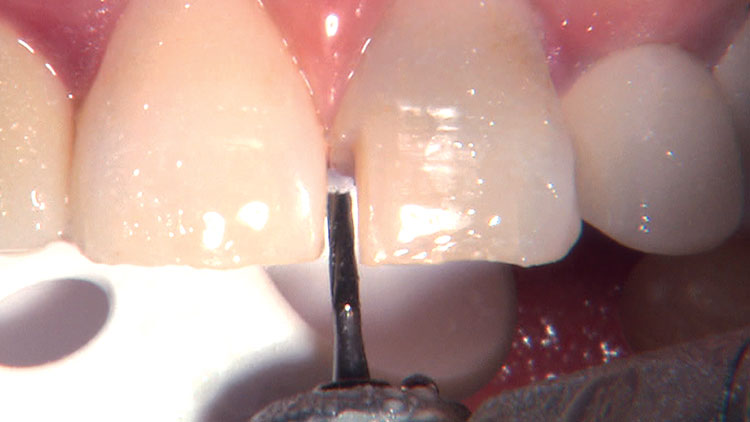
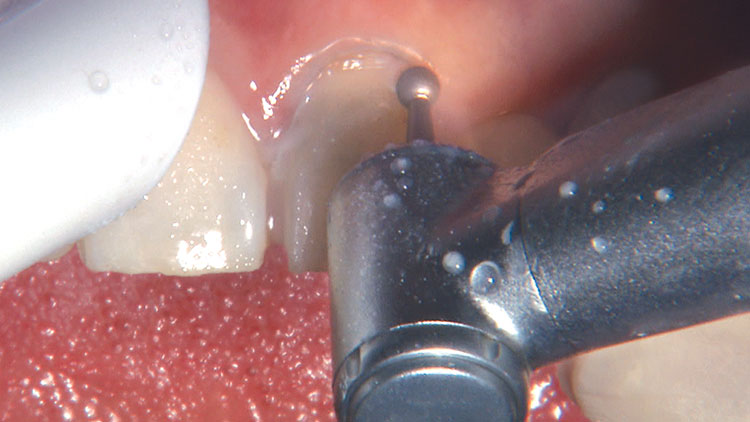
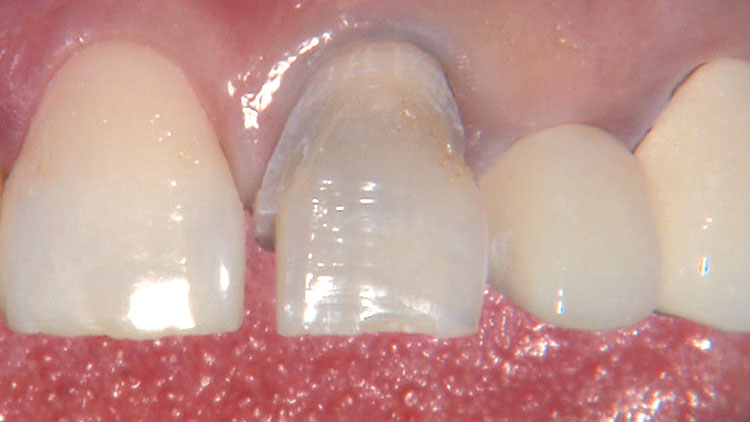
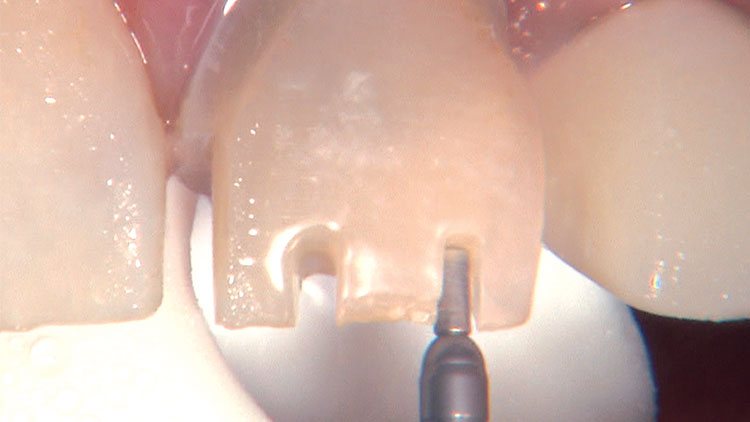
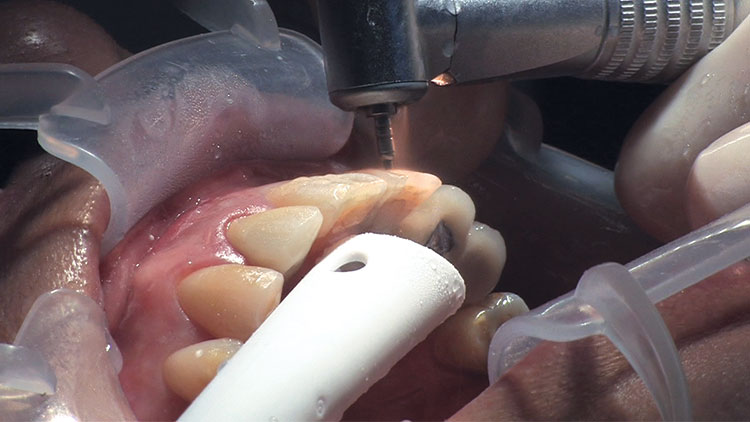
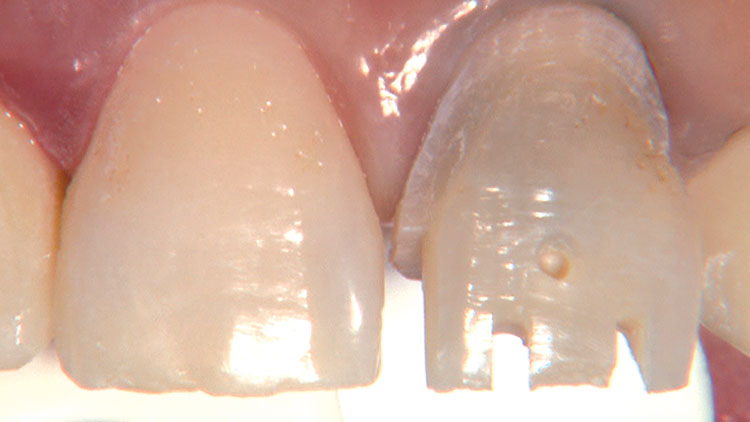
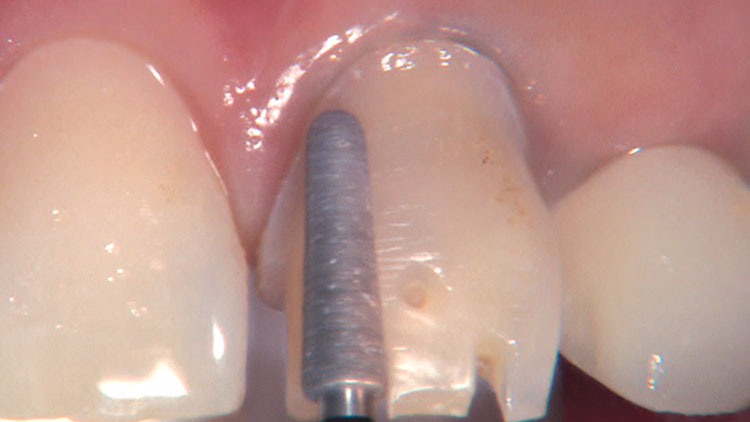
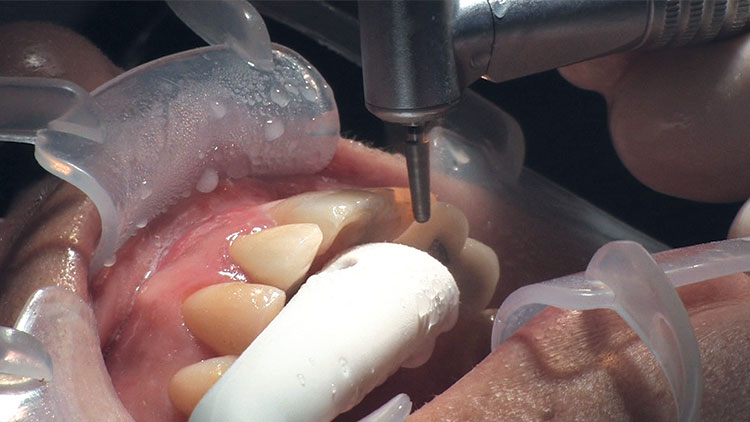
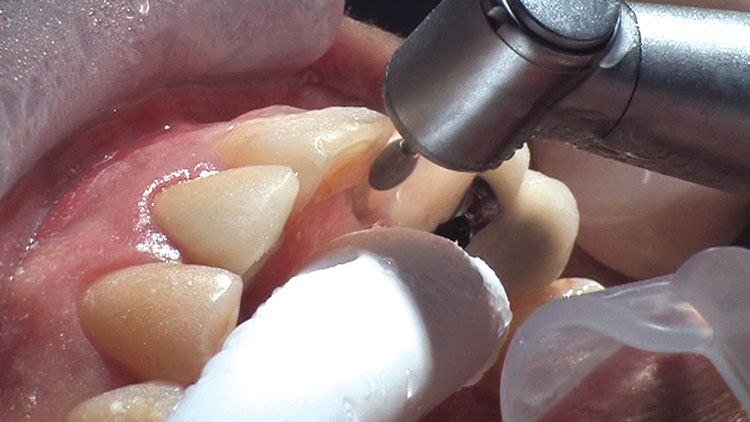
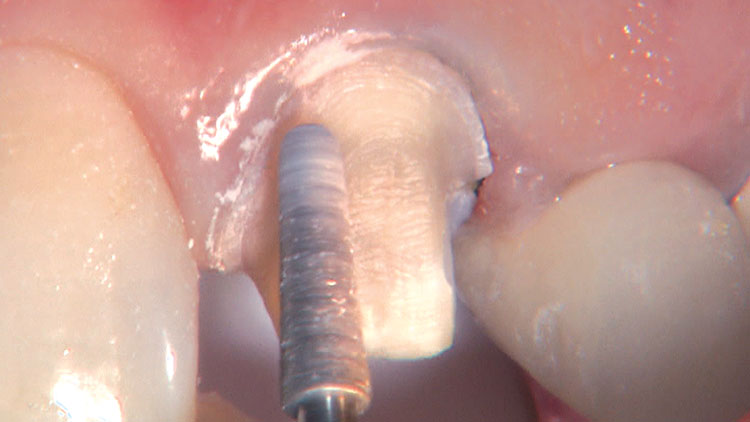
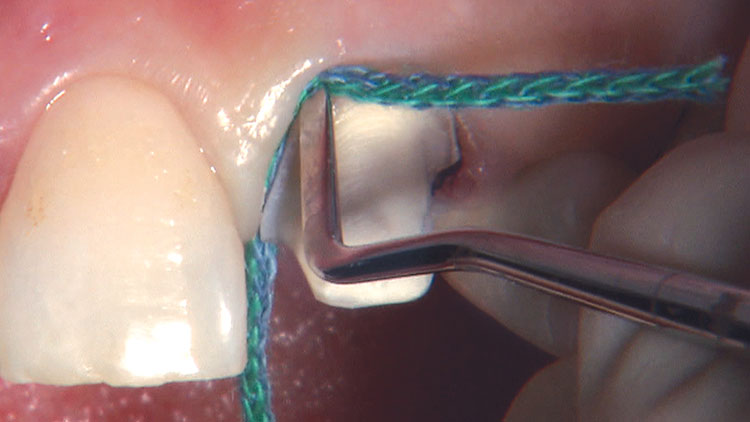
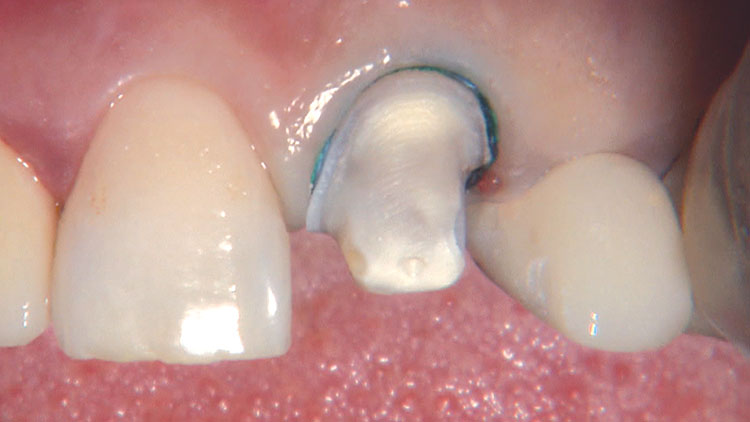
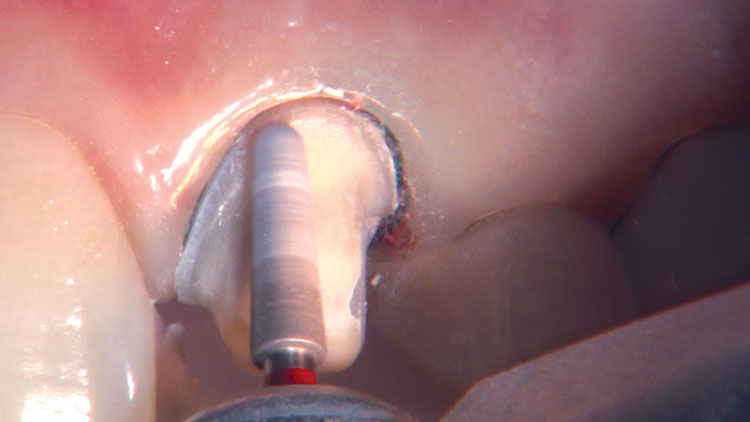
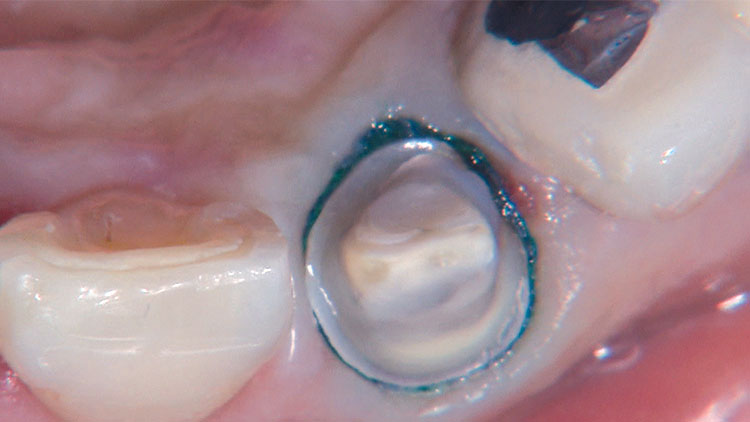
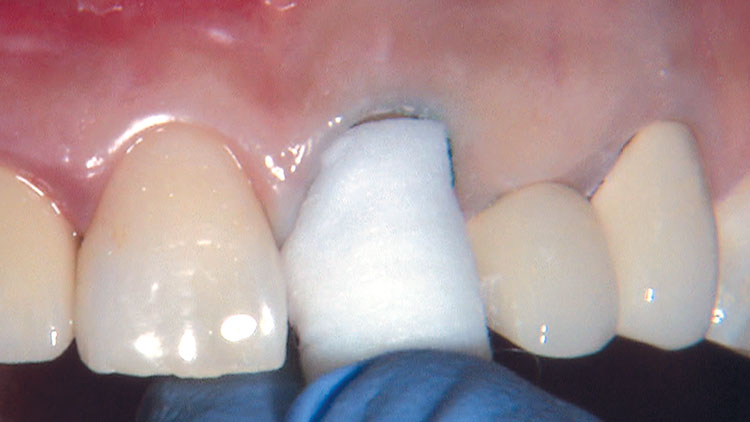
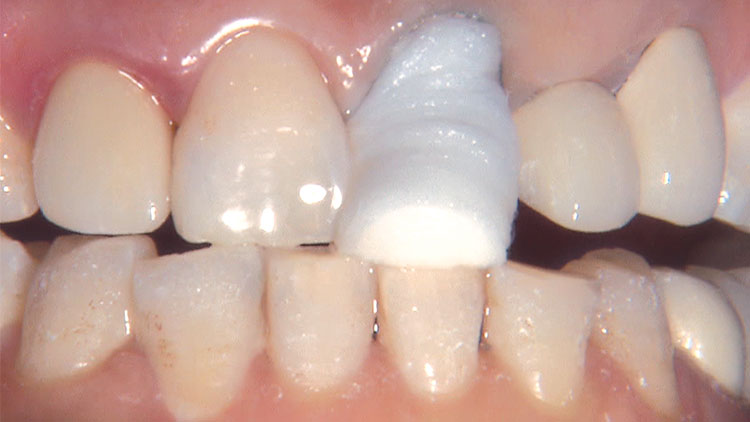
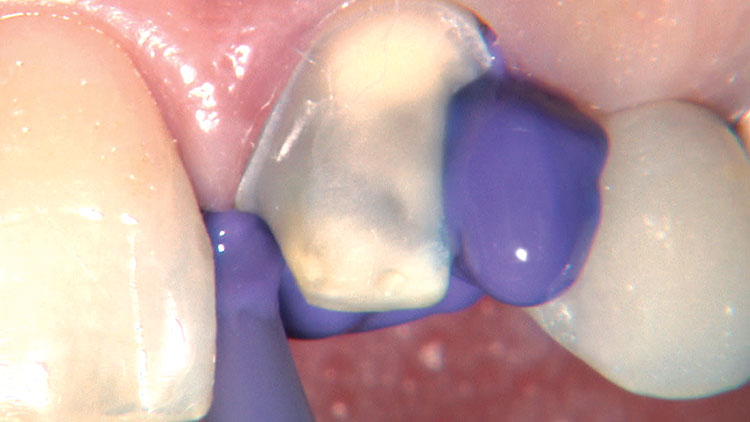
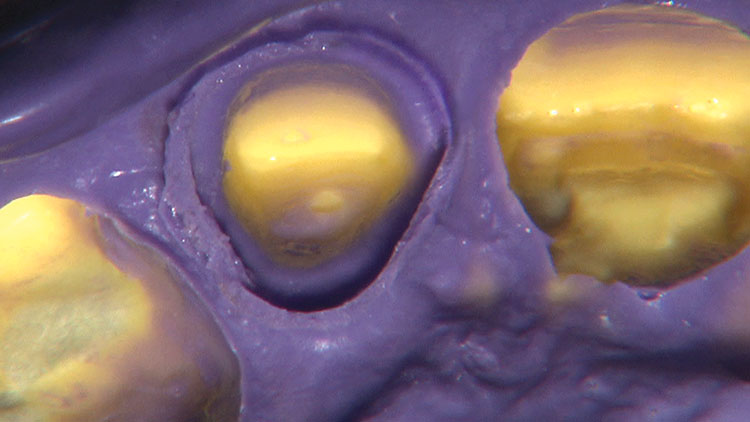
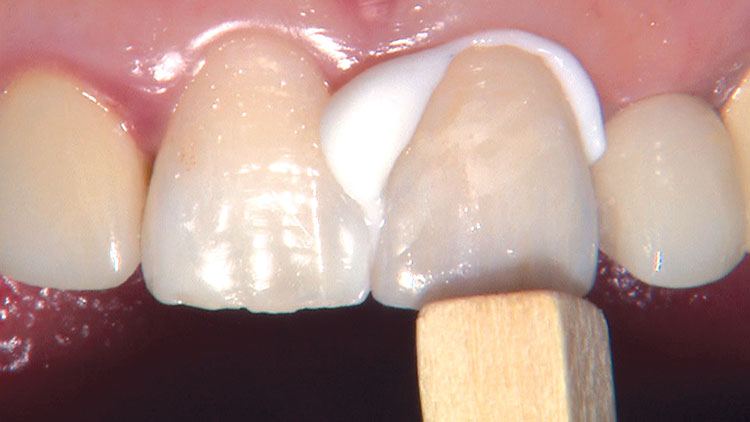
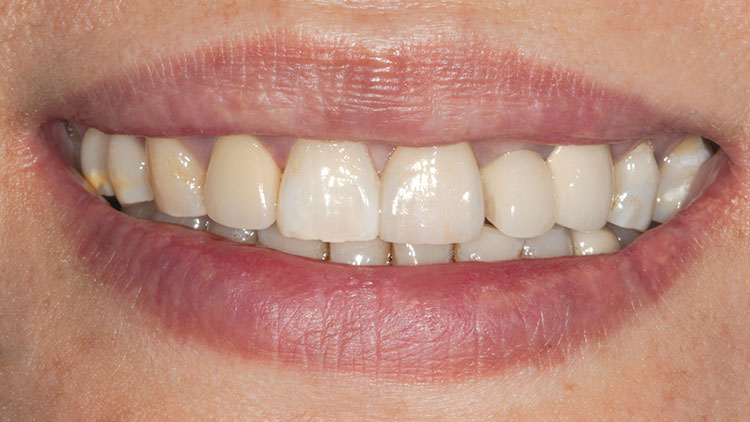
Photo Essay: Ensuring Sufficient Reduction with the Reverse Preparation Technique
If you skipped over my Editor’s Letter at the beginning of this issue, take a peek at it so I don’t sound like too much of a broken record. Using a prep technique based on depth cuts not only ensures that you have given the technician enough room for whatever restorative material you have prescribed, but it also fashions the preparation into the ideal shape without requiring the sculpting skills of Rodin.