Interview with W. Keith Thornton, DDS: Pioneer of Dental Sleep Medicine

Dr. W. Keith Thornton is the founder, chairman and chief technical officer of Airway Management Inc., the company that produces the Thornton Adjustable Positioner (TAP®) line of products for the treatment of sleep-disordered breathing. A practicing dentist in Dallas, Texas, for 37 years, he invented the first TAP device in 1994. In this interview, Dr. Thornton discusses how he began providing oral appliance therapy, the mechanics involved in TAP devices, and why the practice of dental sleep medicine is not more commonplace.
DR. NEIL PARK: How did you get involved in dental sleep medicine?
DR. W. KEITH THORNTON: I had a lot of experience treating temporomandibular disorders (TMD), and I taught TMD treatment at The Pankey Institute for many years. I was working with an ear, nose and throat physician, and the doctor had unsuccessfully tried to treat a patient suffering from sleep-disordered breathing with both continuous positive airway pressure (CPAP) therapy and surgery. CPAP devices fail in about 75 percent of sleep-disordered breathing cases in the first year because they often leak and cause patient discomfort — and patients stop wearing the device because it doesn’t help them. In this particular case, which was also my first dental sleep medicine case, the patient was probably one of the most medically compromised people I’ve ever treated. She had cardiovascular disease, hypertension, congestive heart failure and atrial fibrillation, and she was massively obese. The person who sent this patient to me was the head of sleep medicine at UT Southwestern Medical School. He said: “We’ve done everything we can. Maybe a dentist can help — would you be able to take a look?” In this case, all that needed to be done to treat this patient was to move the jaw forward, like performing CPR. It was absolutely simple.
NP: And, of course, you’re well-known as the inventor of the TAP appliance. Tell me a little bit about this device and how it’s different from other appliances.
KT: When I developed the TAP appliance, I thought to myself, how do we keep the airway open? How do we normally breathe? Do we breathe with our teeth together? No, we breathe with our jaw down and forward. Why do we make dentures with at least 3 mm of freeway space? Because our tongue is forward and out of the airway — and our jaws are apart to allow room for our tongue. Also, while people who breathe normally have their tongue in the palate, people with sleep apnea have their tongue between their teeth, which is why scalloped tongue is common in sleep apnea patients.
One crucial thing is that you need to have an adjustment mechanism that can move the jaw forward and get the airway open. It should be simple enough that patients can make modifications themselves. This device is designed to keep teeth apart and provide enough room for the tongue to move forward. While your tongue is trapped when you put your teeth together, if you open your mouth a little bit, your tongue can go between your teeth. That’s what you want to do.
Ultimately, the main guiding principle of the TAP is jaw placement, particularly how far you move the jaw forward. With this appliance, we have a screw device on the lower portion that moves the jaw forward as much as the patient would like. We tell people to screw the key every other night. And we always tell the patient: “You are in control of your therapy, not the doctor. Make sure you maintain the comfort level that works best for you. If it’s not comfortable, move it back.” So patients have the ability to adjust the appliance out and back until they stop snoring and feel better. With the TAP, there are no precision bites you have to take or difficult procedures from a dental standpoint, and fitting can be done by assistants.
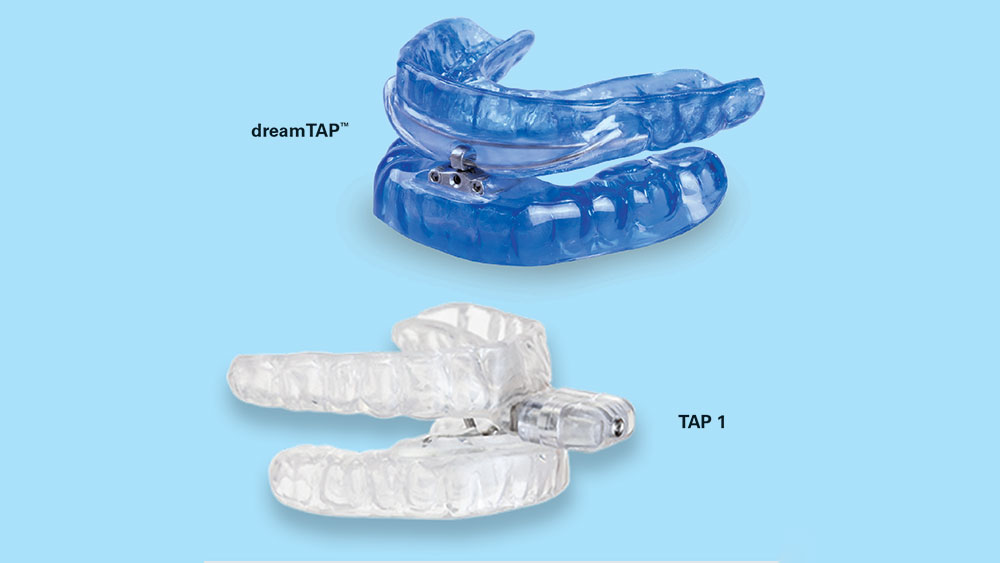
The TAP 1 appliance was released in 1996. As the first adjustable device that was immediately effective for OSA patients, the TAP 1 was quickly adopted by pioneering dentists in the burgeoning field of dental sleep medicine.
NP: I hear from many dentists who are concerned about appliance side effects related to occlusion and bruxism. What are your thoughts about this?
KT: Preventing tooth movement in patients has always been a major focus of mine, dating back to when I taught occlusion at The Pankey Institute. TAP appliance users also receive an AM Aligner, which minimizes any side effects associated with TAP use. You can certainly prevent tooth movement and jaw-position movement if you have the patient use the AM Aligner every morning. And studies have shown that TAP can actually improve the occlusion in Class II patients if that’s what the dentist wants. Even though our company has made more than 500,000 appliances, the FDA has not received complaints of the device moving teeth.
NP: For my whole career, I have viewed Dr. Gordon Christensen as an unbiased evaluator of clinical devices. Did an opportunity arise to have Dr. Christensen and the Clinicians Report® group take a look at this?
KT: Yes, I visited with him a number of years ago. Gordon certainly understands occlusion about as well as anybody in dentistry. I explained the appliance to him, he reviewed the literature I gave him, and he came back with complimentary words about the appliance. I was thrilled about that.
NP: So we all know the statistics: Many, many patients suffer from snoring and obstructive sleep apnea (OSA), yet they’re not getting treated, and only a small percentage of dentists actually perform dental sleep medicine. Why is dental treatment of sleep-disordered breathing not more widespread?
KT: The American Academy of Sleep Medicine (AASM) has served as the industry spokesperson on the diagnosis and treatment of sleep-related breathing disorders. Historically, physicians have been the only ones involved. We, as dentists, screen for medical problems every day. However, there is a disconnect when it comes to sleep-related breathing disorders. I believe most dentists do not screen for or treat this condition due to the politics and misunderstandings surrounding the issue and scope of practice. However, to really tackle this massive public health crisis, collaboration with all physician groups and other stakeholders must take place
NP: What you’re saying now is a major departure from what so many courses and lectures say. Here’s the standard workflow I hear about: The dentist screens for OSA, and then, if he believes this patient may be suffering from it, he will send that patient to a physician to order a sleep study, because only a physician can diagnose OSA. And then, once the physician makes that diagnosis, there’s sometimes a back-and-forth struggle — is it going to be treated by a physician with CPAP, or is it going to be treated by a dentist with an oral appliance? That’s where I understand the state of the art to be.
KT: Well, that’s the state of the financial art.

According to Dr. W. Keith Thornton, after treating the patient for sleep-disordered breathing symptoms, the dentist should have the patient visit his or her primary care physician for a medical diagnosis.
NP: [laughs] OK.
KT: So, in addition to the AASM, there’s the American Academy of Dental Sleep Medicine (AADSM), which is a group of 200 or so “accredited members” who say they’re the only people who can do dental sleep medicine. But any dentist can do this, and do it well — it’s within the scope of dental practice. We can treat snoring and airway problems, and we can do it with a dental appliance.
NP: But, whether the patient snores or has OSA, the treatment is essentially the same. Is that correct?
KT: Yes, but let me explain something about OSA: It is now pretty much a fairly bogus diagnosis, because what doctors are doing is trying to determine certain numbers so that they can prescribe a CPAP device. There is a whole group of phenotypes that are not sleep apnea but are within the same continuum of airway collapse, and which have all of the associated symptoms and consequences, including cardiovascular disease, hypertension, atrial fibrillation, fatigue and tiredness. This group has all of the problems associated with OSA but as a whole does not quite qualify as OSA — therefore, these cases fall through the cracks. In addition, 83 percent of sleep doctors will not send patients to a dentist if CPAP does not work for them. Physicians have a problem because they’re failing their patients.
NP: Describe the workflow that works for you.
KT: Every six months the patient has a recall appointment for hygiene and examination by the dentist. I just apply that timetable to oral appliances. When I had a general practice, my hygienist always asked patients if they snored. The patient would often say something along the lines of: “Yeah. In fact, I’ve got a CPAP, but it’s in my closet.” And the hygienist would say, “OK, we can start treating you for snoring.” The hygienist only has to ask a few screening questions and provide informed consent to the patient: “We are not treating you for OSA. All that we are doing is treating you for bruxism, snoring and dry mouth. We’re treating you for various conditions that fall under our scope of practice.” If we say we’re treating the patient for OSA, we need an OSA diagnosis by a physician. The key is to send the patient to their primary care physician and have the physician determine what the medical issue is and whether the patient needs a sleep study.
NP: OK, so under the workflow that you describe, you do not have a medical diagnosis, so does that mean patients cannot use their medical insurance?

According to Dr. Thornton, in some states, dentists can order sleep studies for patients as long as it is specified that the studies are intended for screening instead of diagnosis.
KT: Absolutely not. We give patients the option — if patients want OSA treatment to be paid for by their medical insurance, they will need a medical diagnosis. You provide a screening, and you treat patients for snoring and other conditions related to sleep-disordered breathing. And it works: The patient is less sleepy and has lower blood pressure. But that’s merely a screening, not a diagnosis, and we use the oral appliance as a screening device for sleep apnea. We tell the patient, “You may have sleep apnea, because this appliance works,” and then we send them to the sleep physician. The physician will conduct a sleep study of the patient without the oral appliance in, and then the physician can determine whether or not the patient has sleep apnea. During the same study, though, I want that patient tested with the oral appliance to determine the effectiveness of the appliance. So, if the sleep physician you work with diagnoses OSA in a patient without an oral appliance, yet does not detect OSA after testing that same patient with an oral appliance, you are legally covered for treating OSA.
NP: So we as dentists can order a sleep study.
KT: In some states, such as Texas, we certainly can — it is within our scope of practice. It’s on a state-by-state basis. Ordering a sleep study falls under our scope of practice as long as we say we’re providing a screening instead of a diagnosis. It’s no different from referring a patient to a cardiologist. If that’s the case, then we can order a level 3 sleep study. We never tell patients that they have OSA, but we can screen them with the oral appliance and tell them, “Now that you are using our oral appliance, the odds of you having OSA are less than 3 to 5 percent.”
NP: With millions of undiagnosed and untreated patients, along with thousands of dentists looking for new practice revenue streams, you would think dental sleep medicine would be more common. So how do we get started?
KT: Ask patients if they snore, and if they do, ask whether CPAP has worked for them. CPAP has not worked for thousands of people, so there’s lots of opportunities to provide dental sleep medicine to people who need it. However, there are several problems with getting an OSA diagnosis. The patient will get a CPAP first. Unless their CPAP device failed within a month, they will not be able to get an oral appliance. You need to emphasize that appliance therapy should be the first line of sleep-disordered breathing therapy — it can treat 95 percent of people. You should do it as part of dentistry and get paid for it.
The other thing is — and this is absolutely critical — this patient has a chronic problem. The only way you can fix it is through orthognathic surgery, frankly. And that’s why I say this is a dental problem with a dental solution. You need to have the patient back every six months or every year, and every three to five years you need to remake the appliance. Half of my business involves remaking appliances. Getting the patient to initially adopt the appliance may be difficult, but getting the patient to adopt the remade appliance is much, much easier. If patients break their appliance, they’re at your doorstep that morning saying: “Doc, this is an emergency. You’d better fix my appliance because I can’t sleep without it.” So they aren’t going to leave your practice. You’ve got instant patient loyalty right there.

Dr. Thornton (right) with Dr. Neil Park (left), vice president of clinical affairs at Glidewell Dental.
NP: Keith, it’s been a great pleasure chatting with you.
KT: Thank you very much. I’m really happy working in this field. And I greatly enjoy working with Glidewell Dental as a partner. I really think that your company is playing one of the biggest roles in dental sleep medicine — and in dentistry as a whole.
NP: Well, thanks. I learned a lot today, and I really enjoyed talking with you.




