Prosthetic Tooth Repositioning: A Viable Treatment Option for Select Cases
Introduction
For many years, patients with esthetic and functional problems due to tooth malposition have had few treatment options. Orthodontics is the first option to correct tooth malposition; however, not all patients are willing to follow through due to the length of time it takes to complete treatment. In a certain percentage of these cases, orthognathic surgery is also suggested to correct maxillary and mandibular jaw position prior to orthodontic therapy. Often, the patient is still faced with the prospect of restorative dentistry when these therapies are completed to gain a full esthetic and functional correction. Therefore, many patients never have the opportunity to receive the treatment they seek unless they agree to this lengthy regimen.
For a select group of patients with minor tooth malposition … esthetic and functional correction may be accomplished purely by restorative means.
With the advent of dentin bonding and advancements in dental porcelains, elective esthetic dentistry has never before been in such high demand. For a select group of these patients with minor tooth malposition, such as spacing (diastemata), crowding (mesial and distal overlapping), minor rotations and facial-lingual arch form displacement, esthetic and functional correction may be accomplished purely by restorative means. The patient, however, must understand that correction of these malpositions will require a more aggressive preparation of the teeth involved to align the arch form.
A diagnostic wax-up is absolutely necessary to help determine the amount of tooth preparation that will be required. A silicone or plastic preparation guide, or stent, is fabricated from the diagnostic wax-up that is approved by the patient. In some cases, intentional endodontics is required to gain the proper space for the correction of tooth position. It is imperative that the patient be aware of this possibility before any treatment is started. However, as long as the patient is fully informed of all treatment options, the patient should have the opportunity to pursue this type of elective treatment, if that is what the patient desires.
Case Preparation
In order to determine if a patient is a candidate for prosthetic tooth repositioning, mounted study casts are required. It is recommended to duplicate the models so a preoperative model can be kept as part of the permanent record. The second model is prepared to assess how much tooth reduction is required to gain an optimal result. Depth cuts and preparation dimensions can be recorded for use during the operative phase of treatment. Once the teeth are prepared, a wax-up is done to correct tooth contour and position. Keep in mind proper tooth length and width when designing the esthetics, or “Golden Proportion,” of the case.
When preparing crowded dentition, the first step is to perform an enameloplasty on teeth that are outside of the proposed arch form to bring them into better alignment. Next, the proximal contacts between the teeth are broken. Crowded or overlapped teeth will require wrap-around veneers or full-coverage crowns. It is recommended to use a very thin diamond instrument, such as a 30-micron interproximal composite finishing diamond, or mosquito diamond, to shape opposing proximal surfaces and vertically break the contact between the roots. These surfaces can later be highly polished with 50-micron finishing burs, discs and fine curettes.
One key to achieving good results is having adequate interradicular space for development of a healthy gingival papilla that can easily be cleaned by the patient. Teeth that are out of line in the buccolingual dimension must be corrected by over-preparing the side of the tooth that is out of alignment. The opposite side of the tooth, in most cases, will only need slight preparation in the marginal area. It is important to mention that so-called “no-prep techniques” cannot possibly correct misalignment of functional surfaces without adding thickness to the tooth form, resulting in overcontoured teeth.
Case Report #1
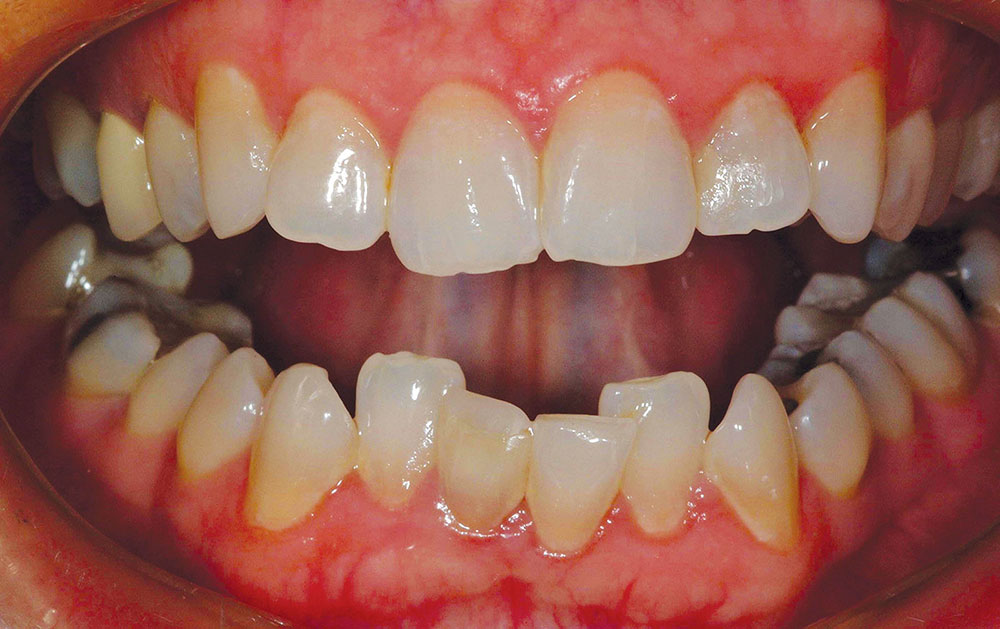
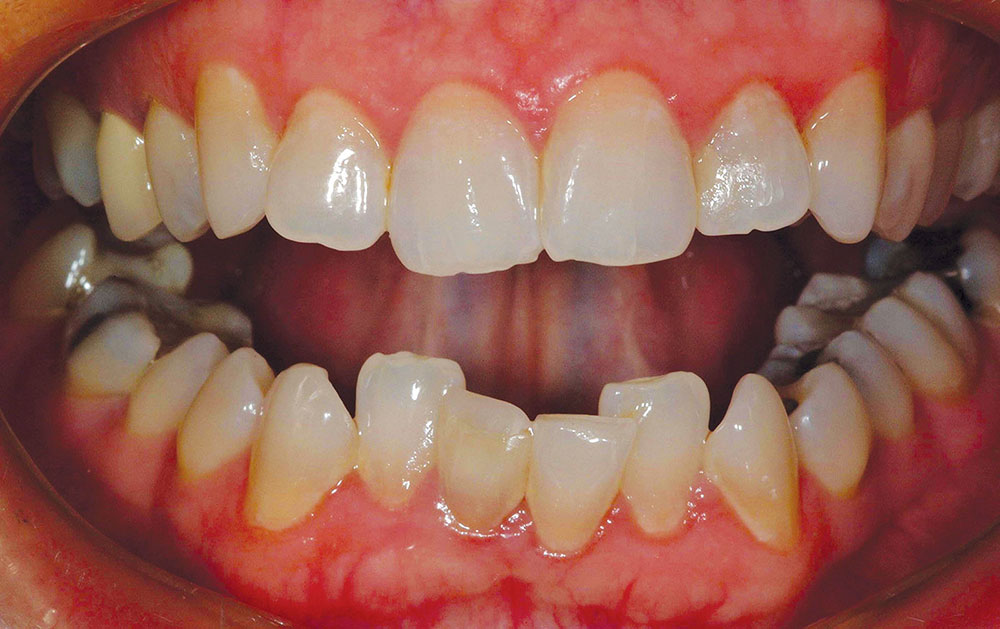
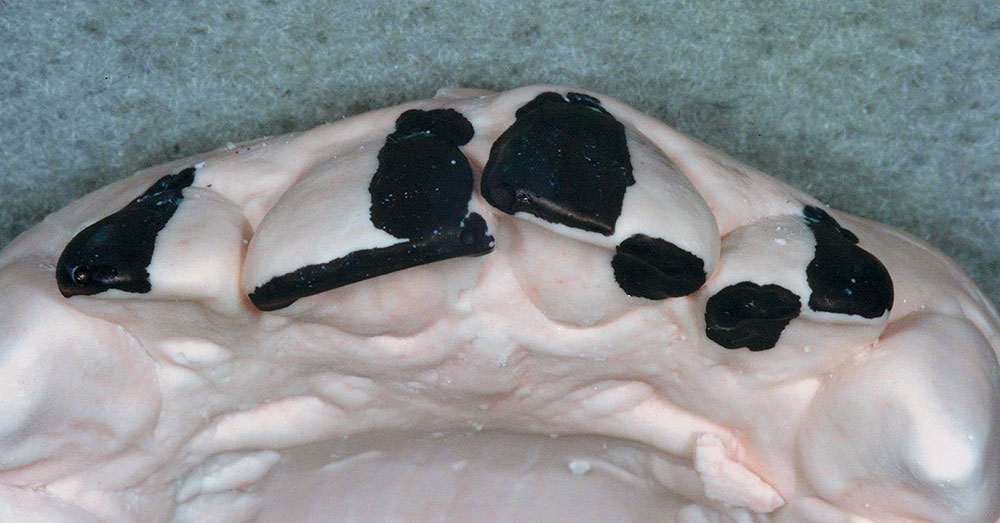
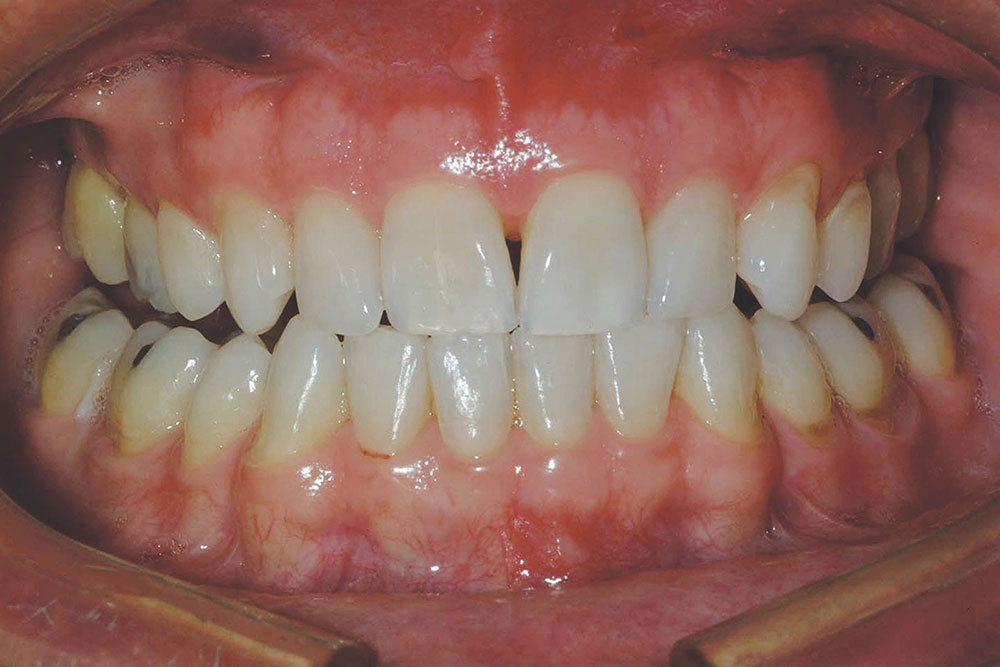
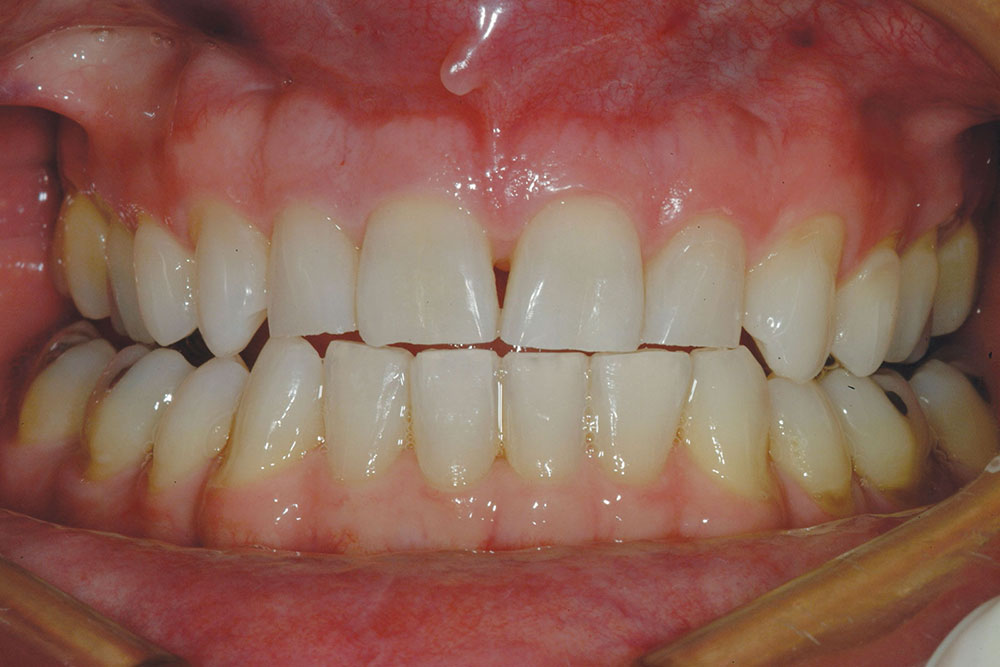
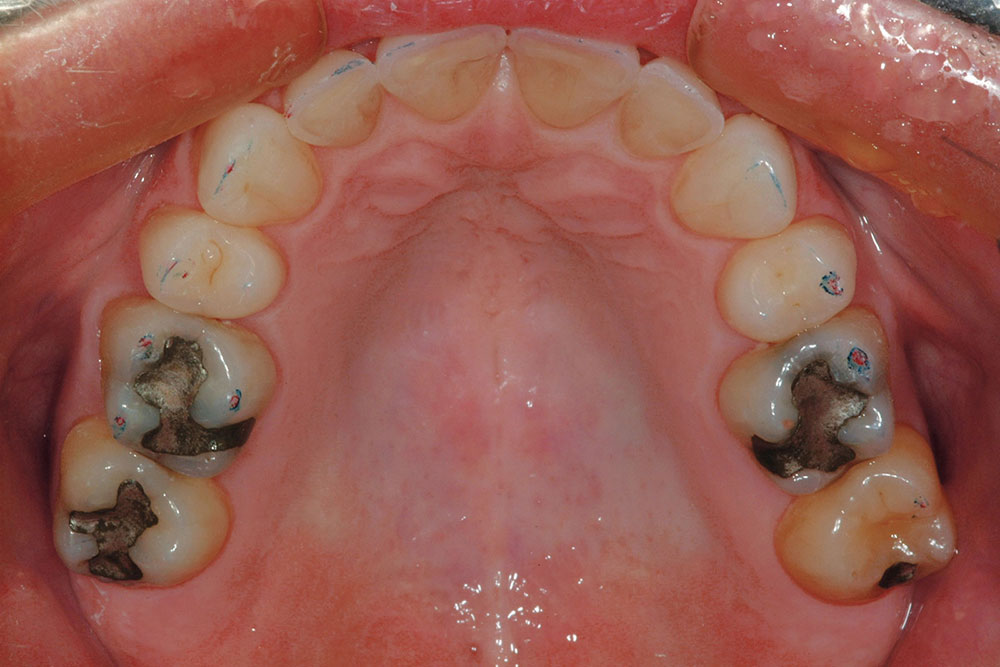
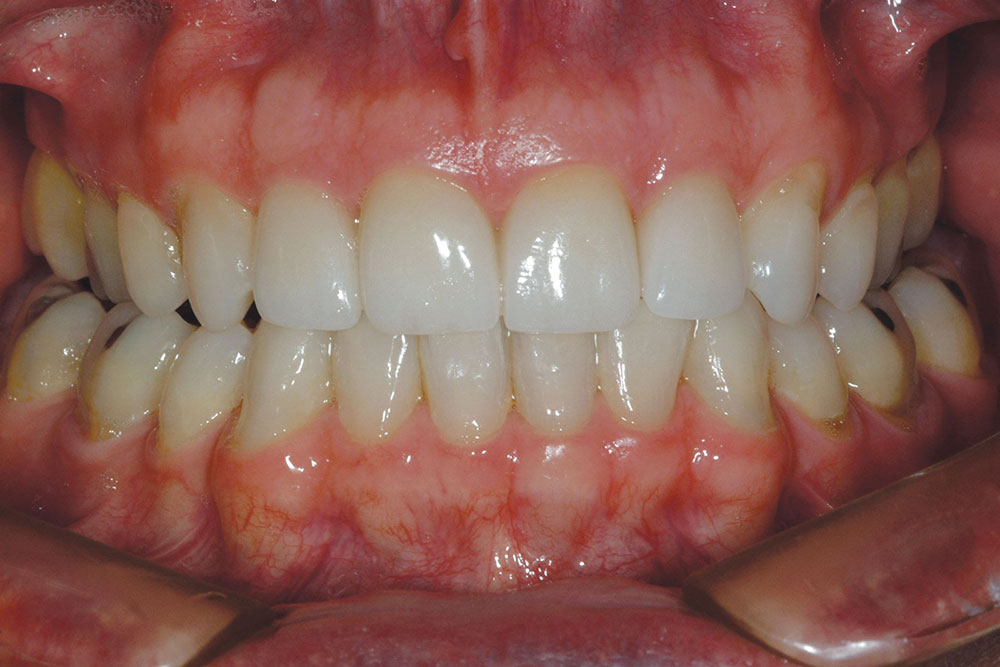
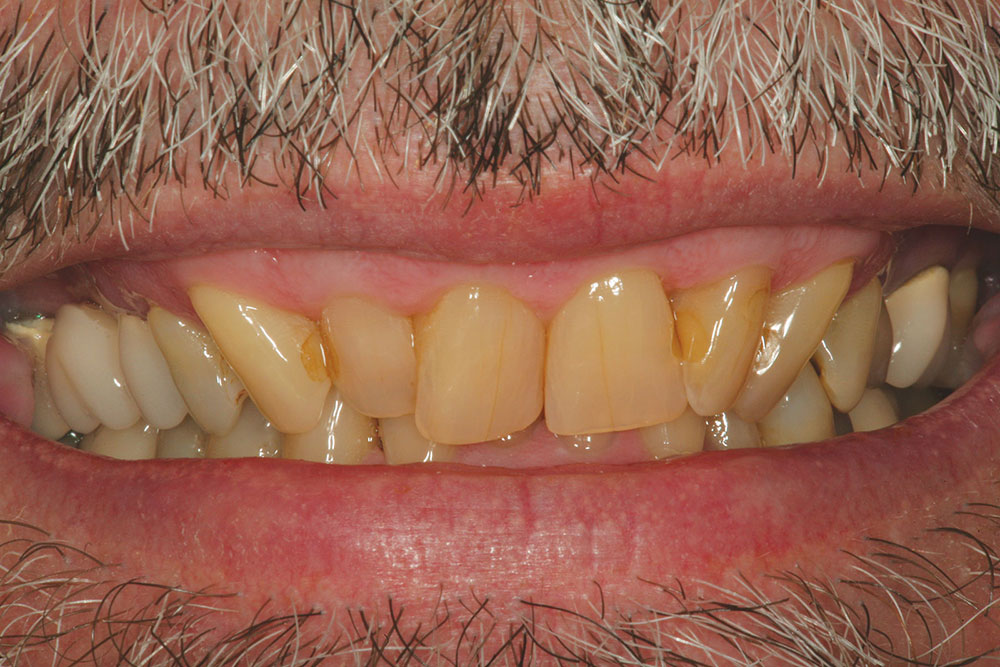
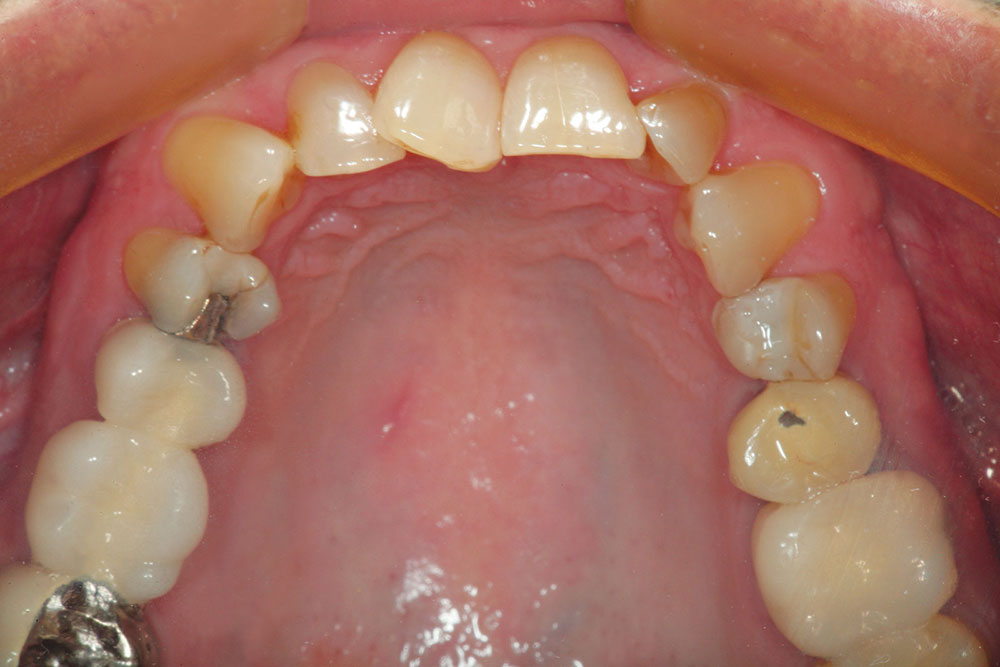
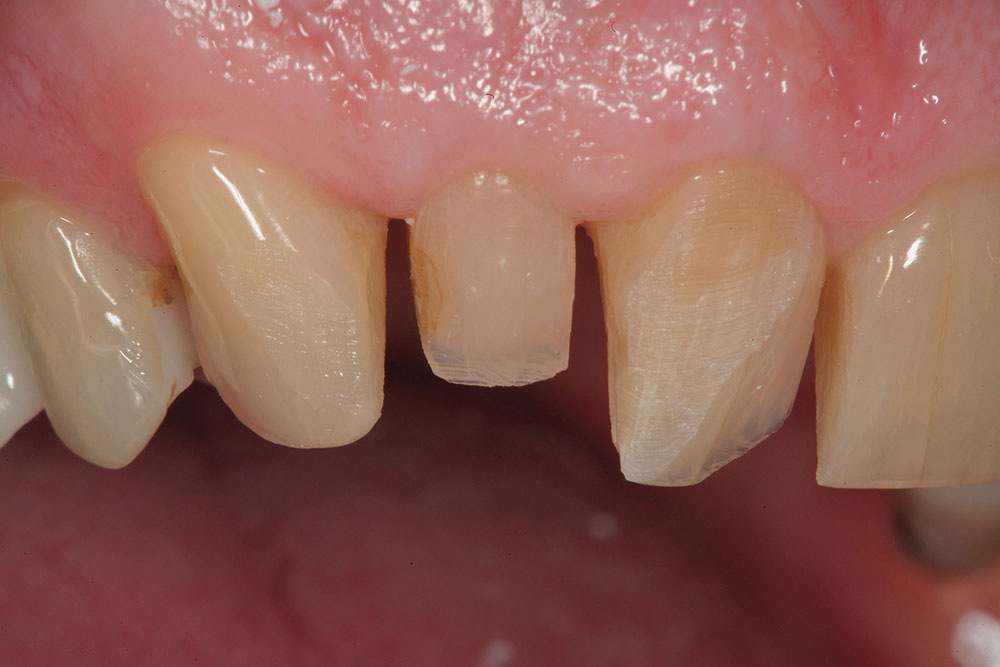
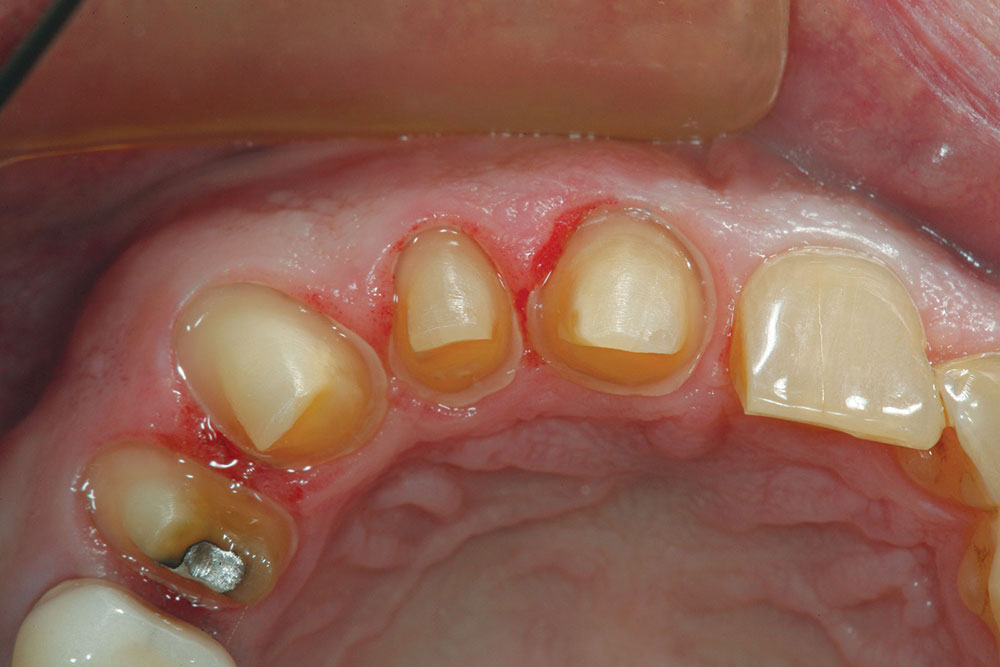
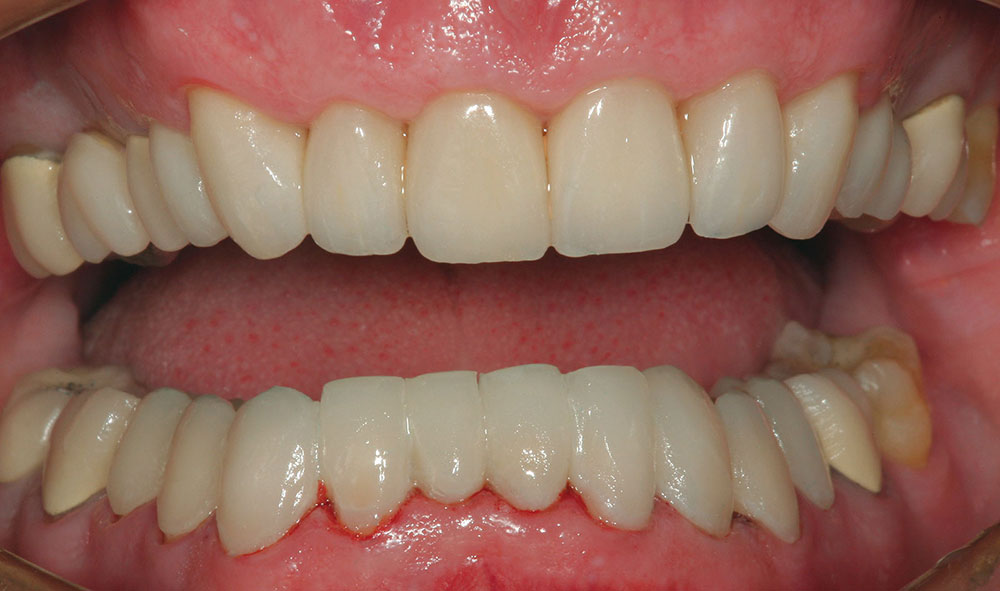
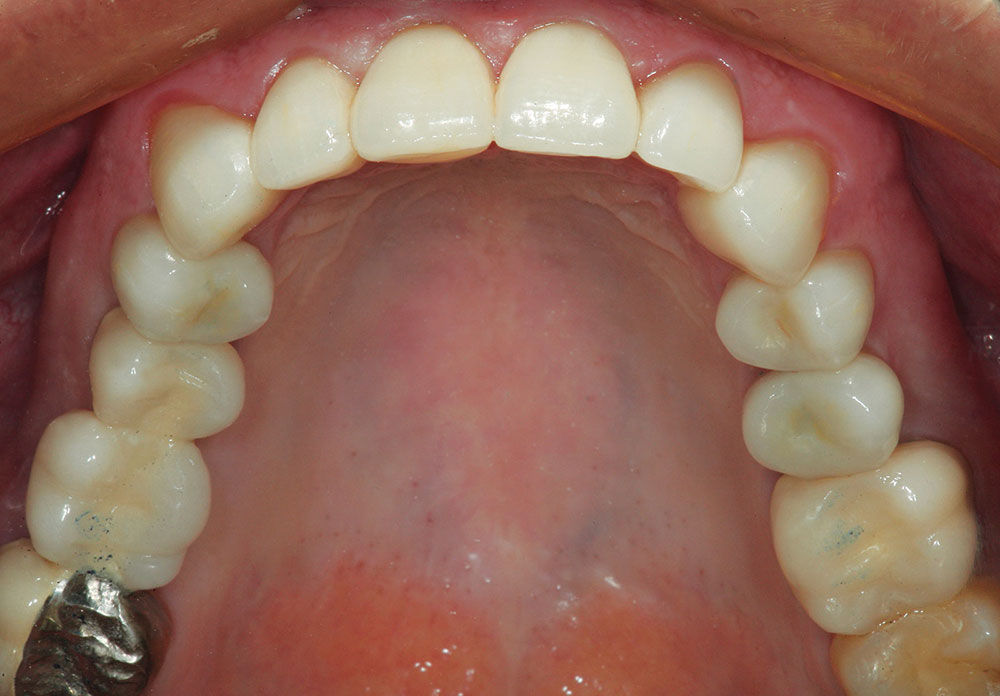
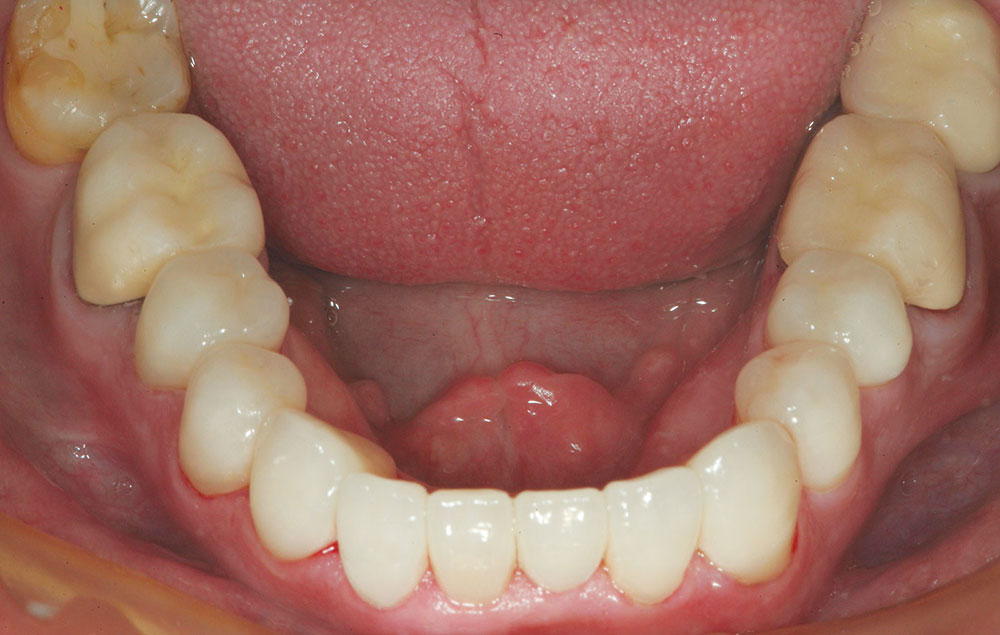
The patient in this case has a Class II Division 1 malocclusion with normal overjet and crowding of the maxillary and mandibular anterior segments (Figs. 1, 2). The areas of tooth structure outside the proposed arch form are marked on the preoperative study model (Fig. 3). For labiolingual malpositions, the proposed arch form will be positioned halfway between the most facially positioned tooth and the most lingually positioned tooth. This will allow for more conservation of tooth structure by avoiding a full correction on any one malpositioned tooth.
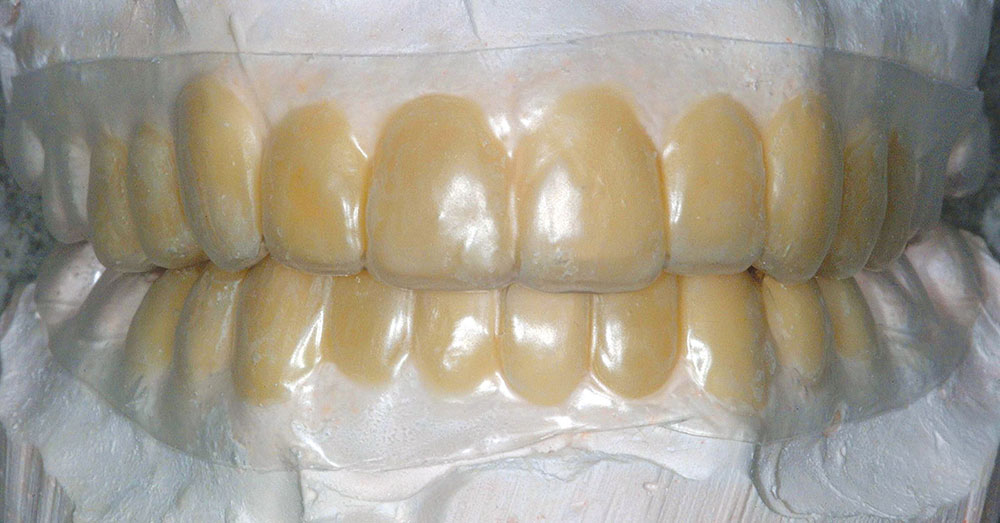
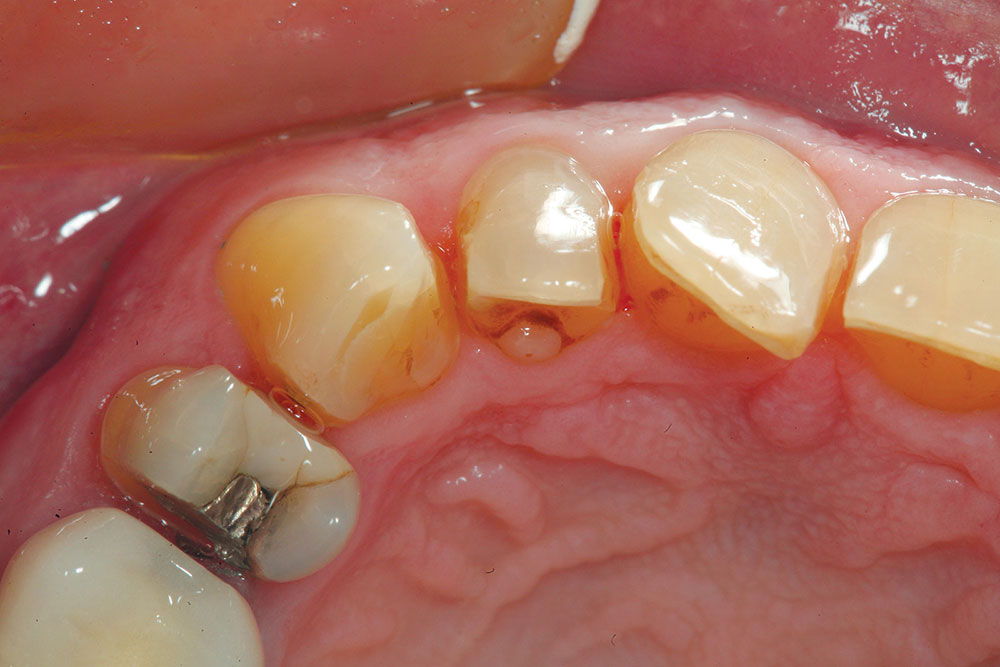
It is important to inform the patient that this type of case may require correction of both arches because, with normal overjet, the mandibular malpositioned teeth will get in the way of correcting the maxillary teeth in the lingual direction if only a maxillary arch alignment correction is attempted. This must first be verified by preoperative cast preparation and composite mock-up (Fig. 4).
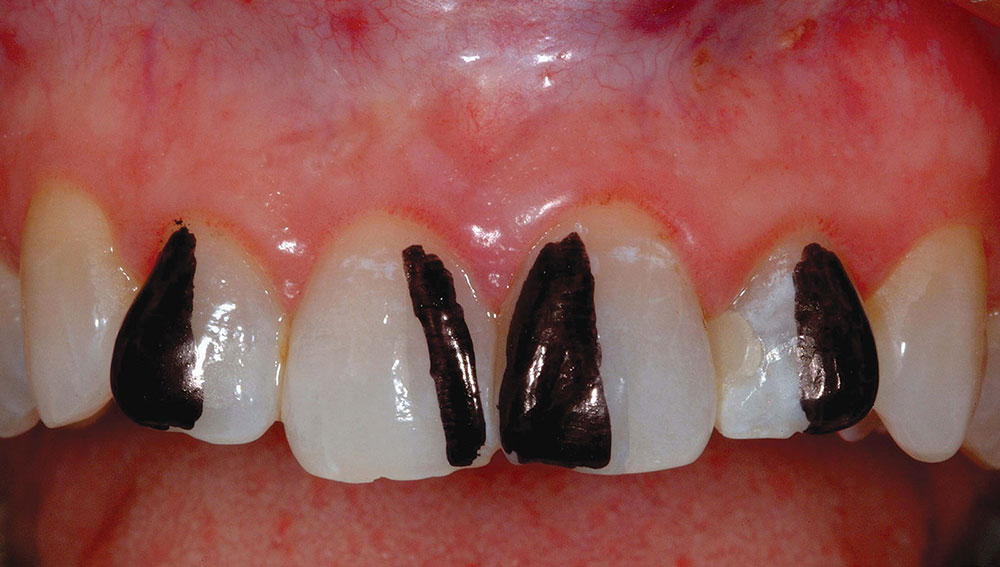
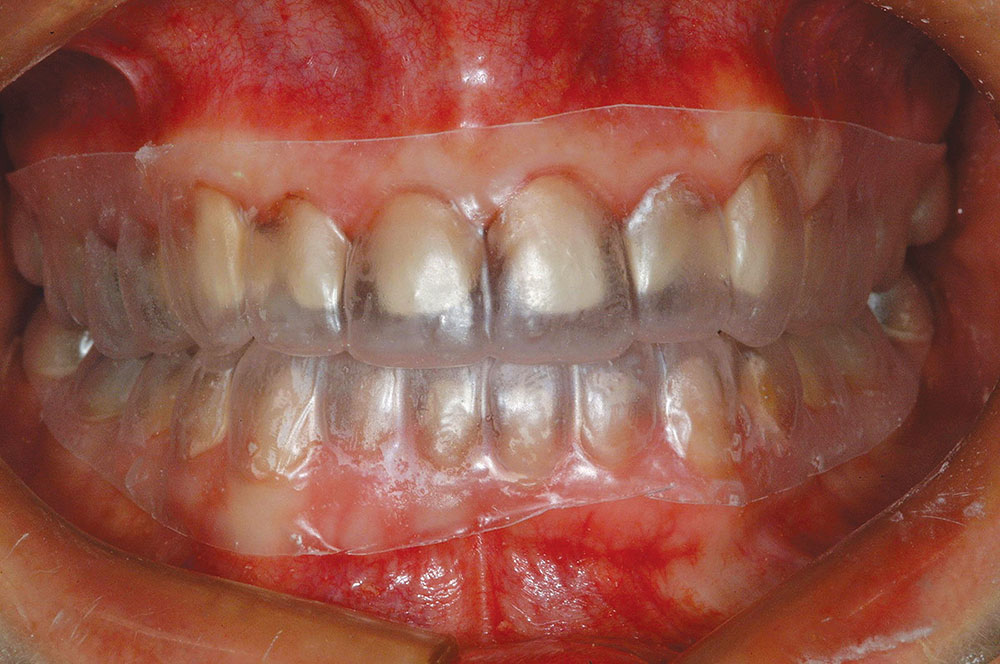
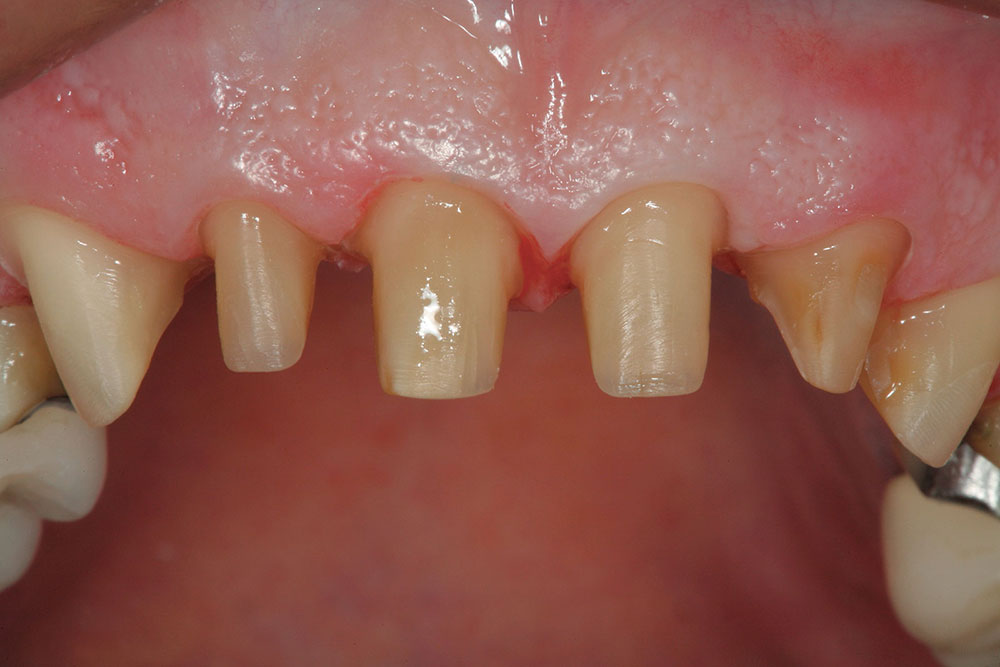
If the case is determined to be reasonable to perform, the patient must then approve the mock-up to ensure that the proposed correction will meet his or her expectations. If desired, the actual teeth can be marked in the same fashion as the study models using a sterile marker to show where the teeth need to be reshaped prior to depth-cut placement and tooth preparation for the restorative material (Fig. 5). Clear provisional stents made from the composite mock-ups can also serve as three-dimensional preparation guides to verify proper tooth reduction (Fig. 6).
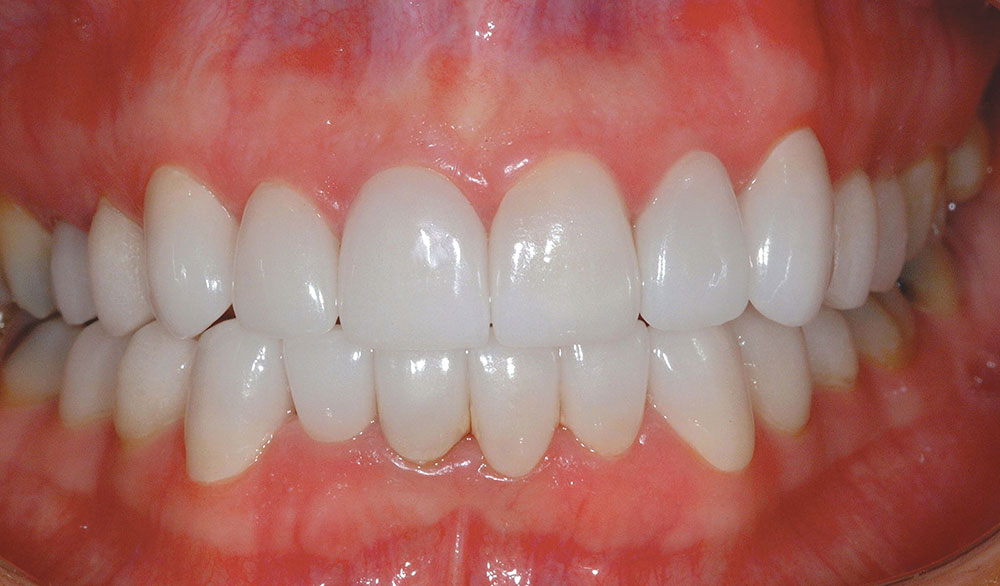
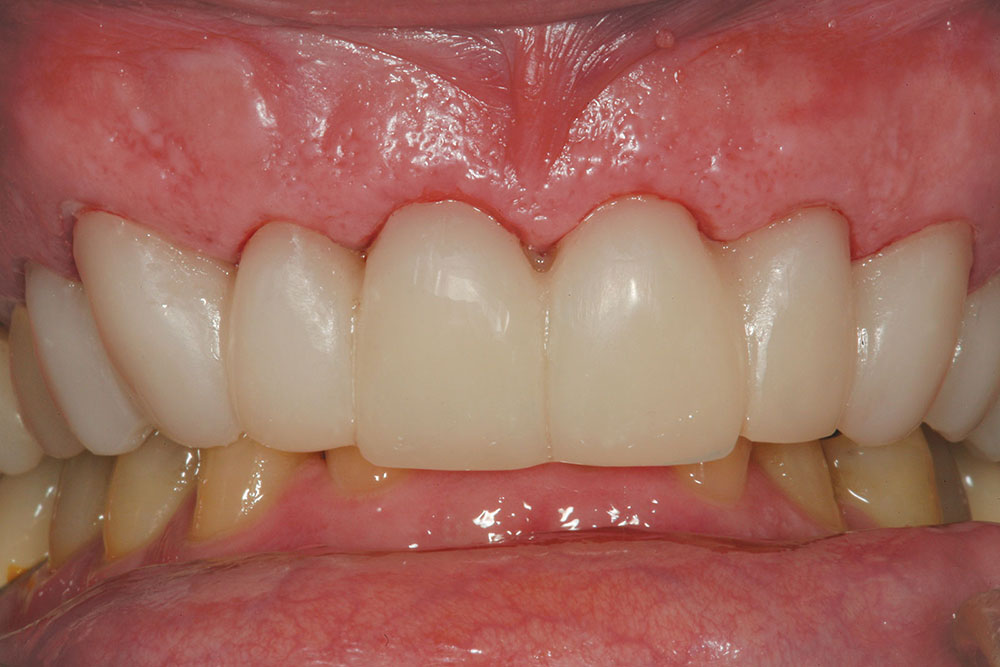
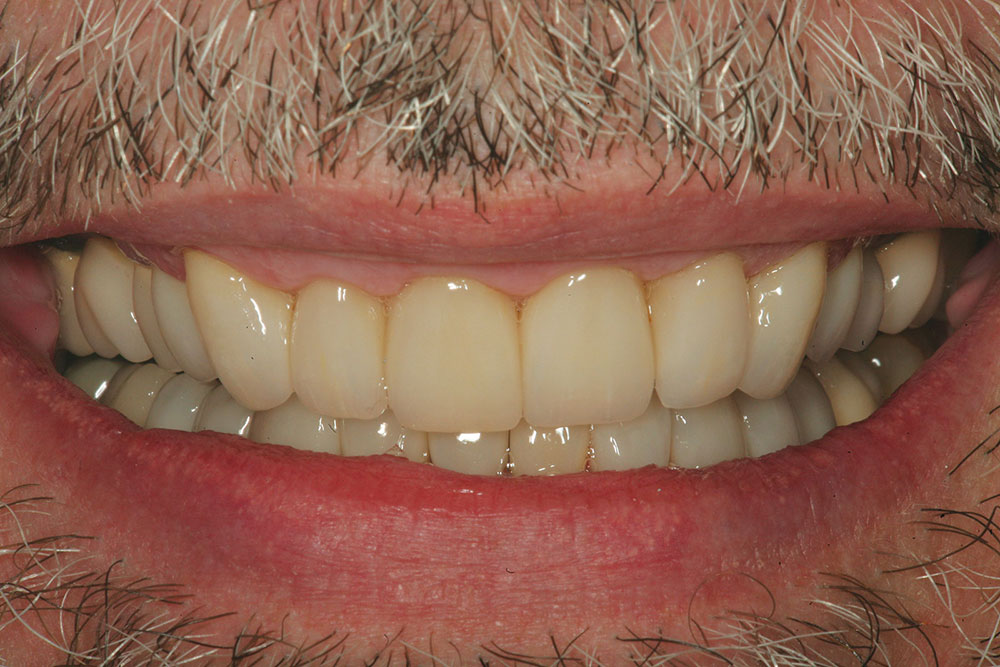
A completed incisal view and full-smile retracted view are shown in Figures 7 and 8. Compare these to the preoperative views (Figs. 1, 2) to visualize prosthetic corrections. Figure 9 is an eight-year postoperative, full-arch, retracted facial view. This case has been esthetically and functionally stable over this period of time.
Case Report #2
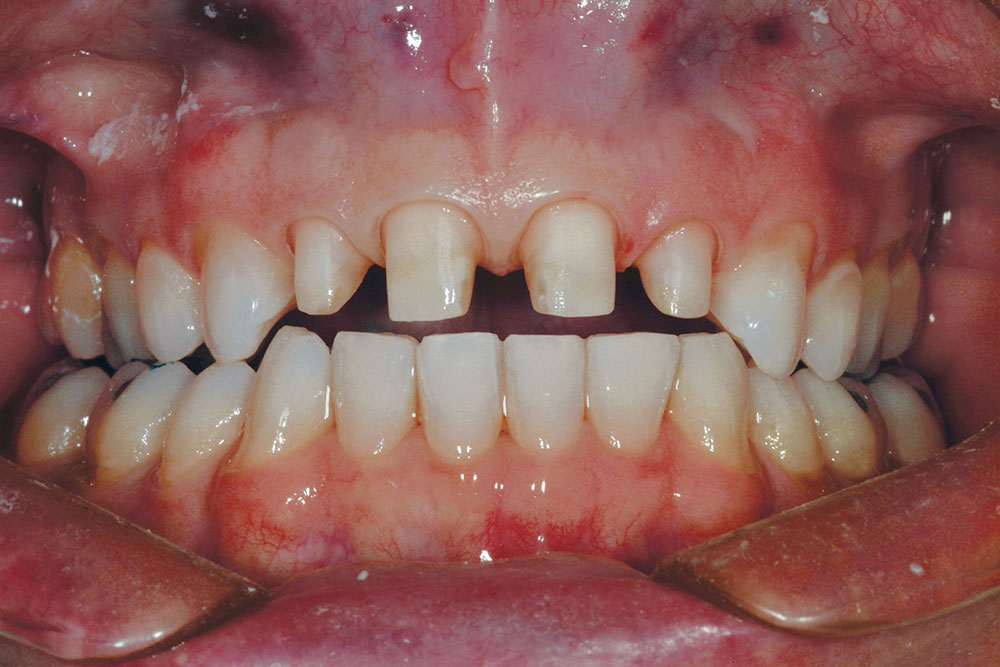
The patient shown in a preoperative, retracted view in Figure 10 is positioned in centric relation. It is evident that this patient is occluding on the anterior only and has no posterior tooth contact. He has been told that his only option is to have jaw surgery followed by orthodontics and restorative therapy. After mounting the preoperative study models in centric relation on a semi-adjustable articulator, it was determined that if the maxillary anterior arch form could be slightly expanded facially (increasing the overjet), it would likely allow the mandible to close and the posterior teeth to contact.
When the maxillary teeth #7–10 are reduced incisally, the posterior teeth will come into contact. Therefore, the operative plan will be to prepare teeth #7–10 and place 360-degree ceramic restorations to correct the arch form in the facial direction and tilt the long axis of the crowns slightly toward the facial aspect, creating overbite and overjet. As the incisal edges are shortened, the posterior teeth come into contact (Figs. 11, 12). Once this occurs, the teeth must then be depth cut on the facial and palatal aspects to allow for the thickness of the ceramic material (Fig. 13).
Figure 14 shows the case completed after the four maxillary incisor restorations are delivered. Note the functional contact that now exists in centric occlusion for the patient. Although the crossbite cannot be addressed without restoration of the posterior teeth and a full-mouth reconstruction, the patient has gained a stable occlusal situation by the restoration of four teeth without invasive orthognathic surgery.
Case Report #3
The patient shown in Figure 15 presented with a dentally compensated Class II malocclusion. He had never pursued esthetic dental treatment because he was consistently told that his functional and esthetic dental problems could not be corrected without orthognathic surgery and orthodontics prior to restorative therapy. In his opinion, the cure was worse than the disease.
After working up the case on study models as previously described, it was determined that this patient could be helped prosthetically without surgical intervention. Figure 16 is an occlusal/incisal view of the preoperative maxillary arch. The orthodontic approach to unraveling this crowded arch would be expansion, or tipping the teeth in the labial direction. This would increase the arch length and allow for proper tooth alignment. It would also increase the overjet, resulting in a more Class II-like appearance.
When planning to orthodontically prepare these teeth, it is important to note that correcting the lingual inclination of the clinical crowns will have the same effect in gaining arch length. There will be very little need to prepare these teeth on the facial surfaces. The majority of the tooth reduction will be on the proximal and lingual surfaces to orthodontically correct the clinical crown angulation with the bur (“diamond-driven orthodontics”).
Interproximal reduction, or IPR, is performed in a similar fashion to that of conventional orthodontics. The goal is to separate the prepared teeth at the free gingival crest (Fig. 17). The facial surfaces of the rotated teeth are reshaped in areas that are facial to the proposed completed arch form (Fig. 18). Lastly, depth cutting and two-plane reduction is performed to allow for the proper positioning and thickness of the definitive restorations (Fig. 19).
Figure 20 shows the completed preparations from the facial view. Looking only at the final shape of the final preparations of the teeth prior to master impression-making, one would be hard-pressed to know how severe the preoperative crowding and rotations were.
After making the master impression, taking a facebow transfer and making interocclusal records, the preparations are provisionalized using a rubberized urethane provisional material and a clear plastic stent made from a diagnostic mock-up of the case (Fig. 21).
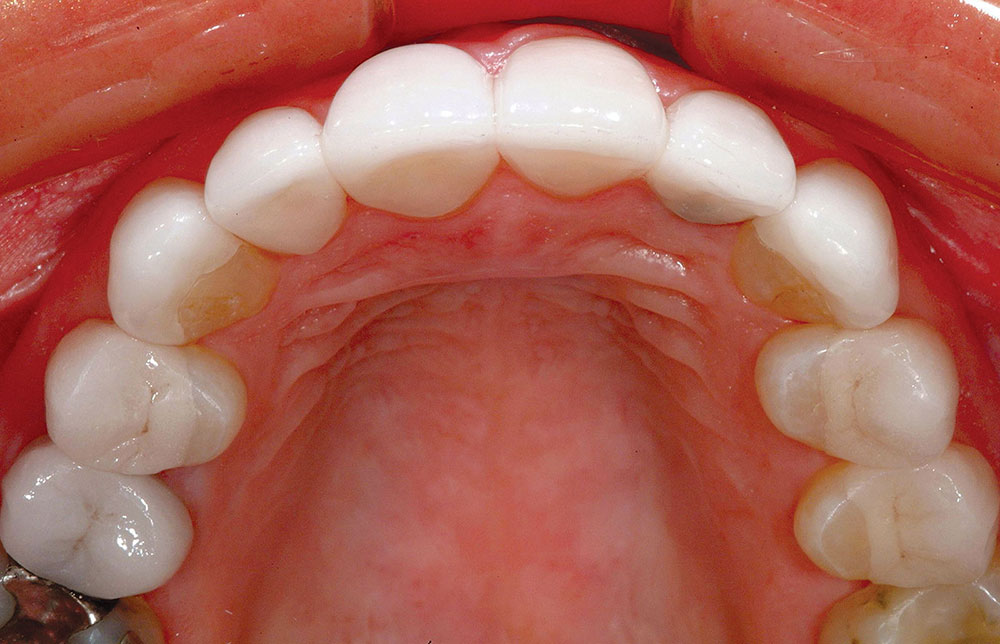
At the following appointment, the maxillary restorations are delivered and the mandibular arch is prepared in the same fashion as previously described, and then provisionalized (Fig. 22). Figure 23 shows the completed maxillary arch from the occlusal/incisal view after delivery of the definitive restorations on teeth #5–13. Figure 24 shows the completed mandibular restoration from the occlusal/incisal. The completed smile view is shown in Figure 25. Compare this final result to the preoperative smile view in Figure 15 to see the remarkable transformation!
Prosthetic tooth repositioning is a viable treatment option for select malocclusions that require esthetic and functional correction. The stability of these cases has been shown clinically when proper guidelines have been followed.
Conclusion
Prosthetic tooth repositioning is a viable treatment option for select malocclusions that require esthetic and functional correction. The stability of these cases has been shown clinically when proper guidelines have been followed. Some specialists have editorialized that this type of treatment is a “quick-fix cop-out,” arguing that patients should be talked into the ortho/surgical approach for these types of cases. It is important to note that crowded dentition is very difficult to clean, which can pose a challenge to maintaining proper periodontal health, so it is very common to see these patients with chronic marginal and interproximal gingivitis and, in later years, full-blown periodontitis when these problems are not addressed and corrected. Therefore, it is important to emphasize to patients that these corrections, no matter how they are accomplished, are needed for dental health reasons as much as they are for esthetic correction. Just ask these patients if the sacrifice of a little more tooth structure versus the more “conservative” surgical approach was worth it for them. It is always best to present all of the treatment options and let patients help decide the course of treatment that best suits their needs.
Dr. Robert Lowe is in private practice in Charlotte, North Carolina. He also lectures internationally and publishes on esthetic and restorative dentistry. Contact him at boblowedds@aol.com or 704-450-3321.
Acknowledgment
The author would like to acknowledge the ceramic artistry of William “CK” Kim, CDT, of Yes Dental Lab in Case #1; Mike Felgenhauer, CDT, of Dental Arts Precision Laboratory in Case #2; and Nadar Hedeshi, CDT, in Case #3.