Interview with Suzanne Haley, DMD
Check out this Q&A with dental sleep expert Dr. Suzanne Haley for her insights on:
· Providing treatment options for multiple sleep disorders
· Growing a practice with dental sleep medicine
· Forming partnerships with and obtaining diagnoses from physicians
Dr. Suzanne Haley is a general dentist from St. Simons Island, Georgia, who is a recognized expert in the area of sleep dentistry. Through the incorporation of dental sleep medicine, Dr. Haley has transformed her practice, improved lives, and saved marriages from the perils of snoring and obstructive sleep apnea. In this interview, Dr. Haley shares her journey into sleep dentistry, life-changing cases, her own practice philosophy and her vision for what dentistry should look like in the future.
DR. NEIL PARK: Dr. Haley, thank you for joining me.
DR. SUZANNE HALEY: Thank you for inviting me. I am very happy to be here.
NP: We chatted earlier, and it sounds like your practice is really not the everyday general practice — it’s a little different. Did you design it that way, or did it just organically develop?
SH: My practice developed into what it is today — it was not originally designed this way. I have been in practice for 25 years, and when I first began practicing, I performed general dentistry restorations, crown & bridge, root canals and extractions. However, in the past seven to 10 years, my practice has become more focused on the overall health of my patients — I am looking beyond their teeth.
NP: A big part of that is sleep dentistry, right? Tell me about how you got involved with that.
SH: Yes, that is correct. I got involved with dental sleep medicine purely by chance. I was lecturing for a course and I happened to meet Jeff Wyscarver, RPSGT, who was instrumental in the development of the bruxism software for the Nox T3® home test (Nox Medical; Reykjavik, Iceland).
NP: And what is his background?
SH: Jeff is a registered polysomnographic technologist and has been involved with sleep for a long time, so he knows everything about sleep. I started talking to him at a meeting, and he sparked my interest. After I left the meeting, I started to review any piece of literature I could find on sleep, any course I could take. As I started looking into it, I thought it was something I would like to do. I wanted to bring this service into my practice and offer it to my patients.
NP: How did you see the need among your patients?
SH: I had a personal experience, as a matter of fact. My husband is a pilot, and because he’s based in New York City, he typically shares a place to sleep with six other pilots. His snoring became so loud that they asked him to move out. If you look at my husband, he does not look like what you’d imagine a sleep apnea or snoring sufferer would look like; he’s in shape, he doesn’t have a large neck. I prescribed him an EMA® (Elastic Mandibular Advancement) appliance (Glidewell Laboratories; Newport Beach, Calif.), which positions the jaw forward to open the airway, and it stopped his snoring.
NP: And that’s all that’s needed in some cases — just reposition the mandible anteriorly?
SH: Correct. And that’s what we did. He stopped snoring with the EMA sleep appliance, but then I started thinking more about it because I would occasionally hear him gasp in his sleep. So, I had his primary physician order a sleep test for him.
NP: And that’s to differentiate someone who snores from someone who has obstructive sleep apnea?
SH: Right. Snoring, bruxism and sleep apnea are all closely related, so I wanted to make sure that this was the right appliance for him. His physician ordered a sleep test, and when it came back, the diagnosis was that he had mild sleep apnea, which surprised us because he does not fit the criteria. Obstructive sleep apnea is the disruption of regular breaths during sleep, so you’re not getting enough oxygen, you’re not going through the much-needed sleep cycles; therefore, you’re not getting the rest your body needs. You may be sleeping 10 hours, but it’s not quality sleep. Patients often get diagnosed for depression, but they are not depressed; they are lacking proper sleep.
Obstructive sleep apnea is the disruption of regular breaths during sleep, so you’re not getting enough oxygen.
NP: There are some serious health consequences associated with sleep apnea.
SH: Yes, especially if it’s moderate to severe. The appliance was able to address my husband’s mild sleep apnea, allowing him to get a good night’s sleep. His six roommates were happy, too, and even started coming to my practice for their own snoring. That’s how my practice began with sleep.
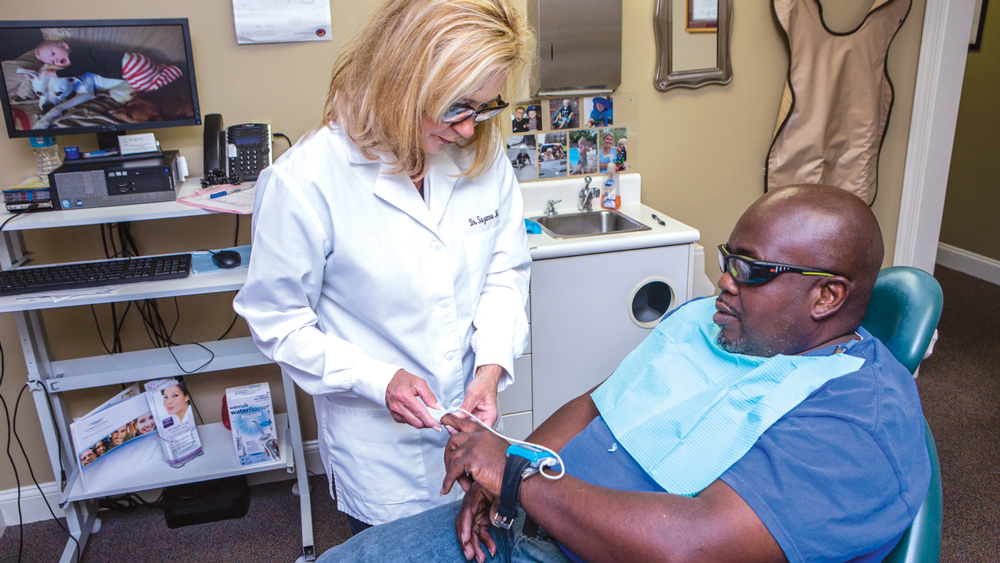
Dr. Suzanne Haley’s practice in St. Simons Island, Georgia, uses dental sleep medicine to focus on patients’ overall health.
NP: It sounds like you save marriages, too.
SH: Yes, we actually have a term for when a person snores, causing their partner to lose sleep: “sleep divorce.” It’s called that because they start sleeping in separate rooms and that’s not healthy for a relationship. So, if you can bring them back together with a dental sleep appliance, everyone is happy.
NP: Has practicing sleep dentistry changed the nature of your practice? Does your practice look different now?
SH: Yes, my practice has totally changed since I incorporated dental sleep medicine. Now, when a patient comes in for a dental hygiene exam, I am not only looking at their dentition or for oral cancer, but I’m also screening to see if they have some kind of airway issue. We’ve updated our health history form to screen for patients with sleep-disordered breathing, including asking if they snore, if they wear a CPAP (continuous positive airway pressure), if they’ve ever had a sleep test, and if their partner tells them that they snore. These are things people don’t talk about and, as dentists, we’re in a unique position to offer much-needed treatment. Dentists probably see their patients and their patients’ families more frequently than any other health care professional does, so if we see that the mother or father wears a CPAP, we know there is a higher likelihood of one of their children having airway issues. We are also working in the oral cavity and have a clear access to the patient’s airway. I want to do everything in my power to give my patients longer, healthier lives.
As dentists, we’re in a unique position to offer much-needed treatment. Dentists probably see their patients and their patients’ families more frequently than any other health care professional does.
NP: Has the addition of dental sleep medicine affected the growth or development of your practice?
SH: Yes. It has allowed me and my staff to provide better overall care for my patients besides just oral care. While dentists can only diagnose bruxism and snoring, we are still able to see a broader picture of patients’ overall well-being thanks to dental sleep medicine training. And my practice has grown with patient referrals.
NP: Dentists can diagnose snoring and bruxism, but they cannot diagnose sleep apnea?
SH: That’s correct. As dentists, we only diagnose bruxing and snoring, but we can treat sleep apnea. By working closely with physicians, we co-treat patients who have been diagnosed with sleep apnea by a certified sleep physician.
NP: How do you get that diagnosis?
SH: When we screen a patient, we are examining the airway, which includes the tongue, tonsils, uvula, palate, neck size, and listening and talking to our patients. If we see an airway issue, I refer them to a sleep physician or to their primary physician to evaluate and possibly order a sleep test.
I also utilize a screening tool that every dentist who is screening their patients should have. The device is called the GEMPro Wellness Monitor (Glidewell Direct; Irvine, Calif.). Not only can you use it to focus in on snoring and bruxism, but you can also get a glimpse into other health issues that your patients may have. When I suspect something, I’ll ask the patient to wear the GEMPro. It tells us if the patient is snoring or if the patient is bruxing — that’s what we’re looking for — and it also tells us if there’s oxygen desaturation going on, which is very important information that dentists can use. If there are airway issues, a dentist does not want to place an appliance to treat only bruxism or snoring and interfere with the patient’s airway even further. If desaturations are noted, we refer them to their primary physician for a sleep test. The GEMPro screening tool guides the dentist to the best-suited appliance for their patient.
NP: As you mentioned, it’s an important part of your practice now. Do you recommend that other dentists get involved in this field as well?

Dr. Haley prescribes dental appliances to treat bruxism, snoring and obstructive sleep apnea.
SH: Oh yes, I certainly encourage all dentists to educate themselves on dental sleep medicine and screen their patients. Every patient should be screened, and all dentists should be screening for OSA. Dentists do not have to treat, but they should be screening — it takes an extra 60 seconds. You’re doing your patients and their families a favor, and you’re expanding your practice. You’re going to help patients, and your productivity is going to increase dramatically.
NP: How does a dentist get involved in sleep medicine?
SH: The best way for dentists to get involved in sleep medicine is to educate themselves and their staff. So many dentists are afraid to implement dental sleep medicine into their practice because they believe they have to make a large investment to get started, and they are reluctant due to the medical billing. Many dentists become overwhelmed. However, in September, I’ll be lecturing at the Glidewell International Technology Center to show dentists and their staff step-by-step how to implement sleep medicine into their dental practice and how to incorporate dental sleep medicine by simply using two screening tools: their eyes and the GEMPro.
NP: Your new two-day course, which is an introduction to sleep dentistry, will include everything from screening to management of cases, correct? How about the practice management aspect of dental sleep medicine?
SH: The first day will be all about what to look for — how to identify patients, how to screen patients. We’ll also cover how to get patients diagnosed by a certified sleep physician and discuss treatment options. It’s going to be a hands-on course where I will teach dentists how to screen their patients, how to use the George Gauge™ (Great Lakes Orthodontics, Ltd.; Tonawanda, N.Y.), and proper impression techniques to deliver a sleep appliance. Then, we are going to dig a little deeper into medical insurance — if you want to do it in-house or outsource it. We’ll also connect dentists to other companies to help the journey into sleep dentistry go smoothly.
I will also show how to market a dental practice that does sleep dentistry and how to build relationships with physicians, which is very important because that is where a majority of referrals come from. The course will consist of hands-on, participation and lecture components in a casual learning environment, and I will guide the dentists and their team on how to implement dental sleep medicine.
NP: Does getting involved in sleep dentistry require a significant investment?
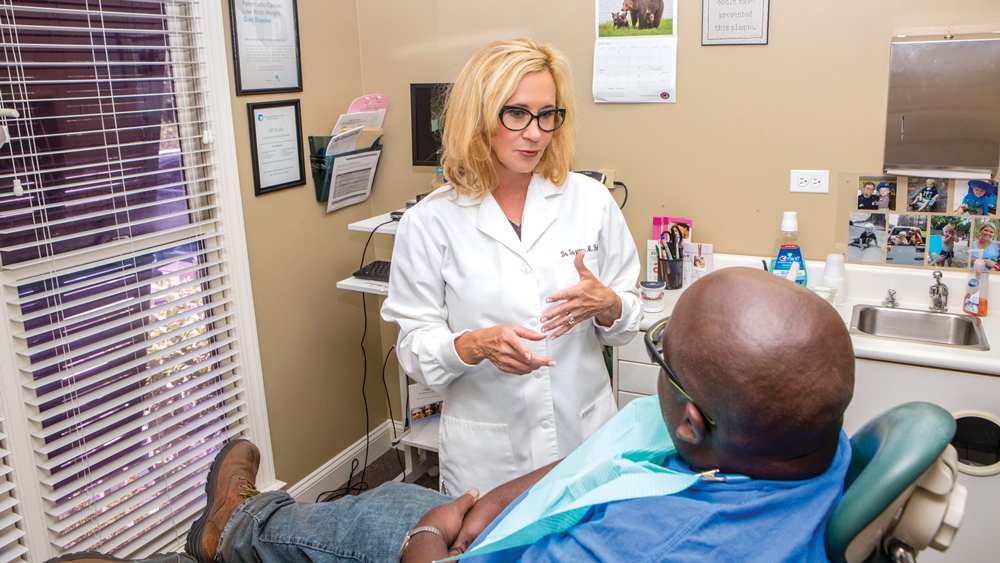
Dr. Haley’s practice provides life-changing treatments to patients who have sleep disorders, including snoring and obstructive sleep apnea.
SH: Not in the beginning it doesn’t, no. And you can spend as much or as little as you want. If you decide you just want to screen, the GEMPro is a great tool that is reasonably priced. With the GEMPro, you can test for bruxism and snoring, and if the patient’s test shows oxygen desaturation, you can refer them out to a physician. Depending on the diagnosis, you’re going to deliver a nightguard, a snore guard or a sleep appliance, and deliver the appliance that works best for your patient. This is a win-win for everyone.
NP: What are some of the mistakes dentists make when first incorporating sleep dentistry into their practice?
SH: The biggest mistake that I see in the beginning is dentists who do not take their team to the courses. I made this mistake, and so when I came back, my team asked: “What are you doing, Dr. Haley? You’re going to offer another service?” They were not educated in dental sleep, and I realized it is almost impossible to implement this service on your own. After that, I knew I needed to take my staff with me. You must have everyone on board to make this successful, and it has to be a team effort. It can’t be just the dentist.
Another mistake that dentists make is first looking outside their practice for patients. There are plenty of patients who can benefit from this treatment who are already in your practice. After attending a sleep dentistry course, your eyes are going to be wide-open because many patients you see are bruxing. Then, you’re going to look into their airway and see that many patients have an airway issue.
Not communicating with the referring doctor is another large mistake dentists make. Building a relationship of trust and accountability between you and other physicians can make or break your referral sources.
NP: How prevalent are these types of problems, like snoring and obstructive sleep apnea, among our patients? Are they fairly common?
SH: They are very common. Probably about 9 percent of women and 24 percent of men in the average dental practice snore or have sleep apnea.
NP: And how do you involve your staff in screening patients?
SH: I take my staff to courses and have “lunch and learn” meetings with them once or twice a month just to make sure we are implementing everything. You’d be surprised; sometimes when you look at a patient, you think they’re just bruxing and clenching because their neck size is not big and they are in really good shape, but they may have a small airway. In fact, smaller women are probably the loudest snorers, so it’s important to screen every patient — you just can’t assume. I remember a patient — a very large gentleman — we screened in our office. He had no apnea, which was very surprising; his airway was large enough to accommodate his tonsils, his uvula and his large tongue. Two major things to remember when incorporating dental sleep are to screen every single patient and to have relationships with physicians.
As dentists, we’re in a unique position to offer much-needed treatment. Dentists probably see their patients and their patients’ families more frequently than any other health care professional does.
NP: And what type of physicians are you talking about?
SH: Every physician — primary physicians, cardiologists, gastroenterologists, OB-GYNs, endocrinologists, pulmonologists, ENTs, psychiatrists — because a lot of people do not get enough sleep at night, and these physicians will be able to refer patients to you. You also need to build a good relationship with a certified sleep physician.
NP: And the sleep physician is who you refer patients to for a sleep test?
SH: Right. I refer a lot of my patients back to the sleep physician, especially Medicare patients. Medicare is a little different because they require patients to have a face-to-face with a primary physician, but I usually go straight to the sleep physician and they have the face-to-face, or I refer them to their primary physician and we work together. When patients have mild or moderate sleep apnea, the doctor usually refers them back to have a sleep appliance. If the patient has severe sleep apnea, the gold standard is a CPAP. If a patient is prescribed a CPAP and they can’t tolerate it, the patient will return to our office and be fitted for a dental appliance.
NP: I have a colleague who was telling me that was his biggest source of sleep referrals — patients who had a CPAP and couldn’t tolerate it.
SH: When a patient comes in who can’t wear a CPAP, we have them sign a form that says they can’t wear it, and those are your home-run patients — you go straight to an appliance. I can’t stress enough the importance of sleep dentistry. So many dentists are afraid to get started, but I can assure every dentist out there that there is no reason to be afraid. Every dentist should be screening and treating — you can save marriages and save lives. It’s an incredibly rewarding field.

Dr. Haley’s course at the Glidewell International Technology Center will consist of hands-on participation and lecture components in a casual learning environment.
NP: We spoke earlier and you shared some really interesting cases with me that show how it works in your practice. Would you care to share one of those cases?
SH: Of course. I live on a small island, so I will be out at a restaurant and a patient will come up and thank me for helping them. I had a case where a man and his wife had not slept in the same bedroom for 10 years because of his snoring and gasping. His wife happened to see one of the billboards I had around town promoting my dental sleep practice and to bring patients in, and they came in for a free consultation. We screened the patient and noted a few airway issues. I referred him to his primary physician for a sleep test. The sleep test came back that he had moderate sleep apnea. He did not want to wear a CPAP; he wanted a dental appliance. His physician signed a prescription for a sleep appliance, so we co-treated him and fit him for a dental appliance. Three months later, the patient and his wife came in and said they were back sleeping in the same bed together and they were thrilled. They hugged me. We did a video on it and put it on social media to show patients that snoring doesn’t have to happen; there is something that can be done to help people who snore. It allowed him to breathe better at night, which was most important, and it also solved the snoring issue that was secondary, but vital for their marriage.
There are tons of cases I could tell you about where we have changed lives.
NP: That’s incredible. You’ve been involved in sleep dentistry for years now, and it has certainly changed the nature of your practice. What do you see for the future of dentistry?
SH: Well, for one, humans are living longer, so we really need to screen our patients because sleep apnea can lead to a number of life-threatening medical issues, like heart attacks, strokes and high blood pressure. Unfortunately, obesity is on the rise and people are not taking care of their health, so we need to educate our patients on their overall health so that they live healthier, longer lives, and so we can prevent sleep-disordered breathing before it becomes more serious. Prevention and treatment are the hallmarks of all health care disciplines, and sleep dentistry is no different.
NP: It sounds to me like you’re envisioning a future where dentistry is much more involved with the overall health of the patient, not just the teeth.
SH: Yes, and that’s what dentists need to do. We are doctors of the oral cavity, but we see beyond that. The health of the mouth is so closely related to overall health. When we look at a patient’s oral cavity and see inflammation or bleeding gums, that’s an infection going on, and if the patient is diabetic or has heart disease, that’s not healthy. Patients really trust us, and we must do our part to ensure they live healthy lives.
NP: I agree. Thank you so much for your time, Dr. Haley.




